Case Report
Primary Hydatid Cyst in the Subcutaneous Tissues of the Neck in the Sub-Occipital Area: An Unusual Site of Hydatid Cyst
Manucher Aghajanzadeh1*, Sharokh Yousefzadeh Jabock2, Hossein Hemmati1, Mohammad Sadegh Esmaili Delshad2, and Piroze Samidost1
1Department of Thoracic and General Surgery, Guilan University of Medical Sciences, Iran
2Department of Neurosurgery, Guilan University of Medical Sciences, Iran
*Corresponding author: Manucher Aghajanzadeh, Department of
Thoracic and General Surgery, Guilan University of Medical Sciences,
Rasht, Iran, Tel: +98-9113-311-881; Email:
maghajanzadeh2003@yahoo.com
Submitted: 08 April 2015; Accepted: 30 April 2015; Published: 04 May 2015
Cite this article: Aghajanzadeh M, Jabock SY, Hemmati H, Esmaili Delshad MS,
Samidost P (2019) Primary Hydatid Cyst in the Subcutaneous Tissues of
the Neck in the Sub-Occipital Area: An Unusual Site of Hydatid Cyst. JSM
Clin Cytol Pathol 1: 3.
Introduction: Hydatid cyst is a condition commonly affecting liver and lungs caused most commonly by Echinococcus granulosus
where as musculoskeletal or subcutaneous hydatidosis is very rare. and Usually are secondary and resulting from the spread of cysts from
other organs, either spontaneously rupture or after spreading from operations for hydatidosis in other regions.
Case Presentation: We present an unusual case of a primary hydatid cyst found in the subcutaneous scalp tissue under occipital
region in a 36 year man. Clinical presentation of patient was a huge cystic mass. Ultrasound findings revealed a cyst lesion in the posterior
aspect of neck under the occipital region. MRI show a cystic lesion. We removed the entire part of cyst lesion surgically. Macroscopic and
microscopic histopathological examinations confirmed the diagnosis of subcutaneous hydatid cyst.
Conclusion: In regions where hydatid disease is endemic, a cystic lesion in any part of the body should be considered a hydatid cyst.
The best treatment is surgery and total evacuation of the cyst elements without any spillage of cyst contained and postoperative albendasol therapy.
Hydatid disease is a parasitic infection caused by the
tapeworm Echinococcus granulosus. This parasitic diseaseis a
significant public health concern in endemic country [1]. Hydatid
disease is endemic in the Middle East, India, Africa, South
America, New Zealand, Iran, Australia, Iran, Turkey and Southern
Europe [1-4].
Life cycle of Echinococcus involves two hosts, one definitive
carnivore host (dogs, cats and certain wild carnivores) and
the other intermediate herbivore host (sheep, goats, swine,
small rodents and other wild herbivores) [5]. Humans act as an
accidental intermediate host is infected after ingesting viable
oncosphere-containing eggs, which have been shed in the feces
of the definitive host [2]. But the liver and lungs are the main
locations [2,3]. Various parts of body may be involved with
hydatid cyst but Hydatid cyst develops most frequently in the liver (65%), the lungs (25%), and the remaining 10% occurs in
muscle, spleen, bones, kidneys, brain, eye, heart, subcutaneous
and pancreas [2,6,7]. Occurrence of hydatid cyst is extremely rare
in the head and neck region even in endemic areas wherehydatid
cyst infestation is frequent. Only a few cases of hydatid cyst
located in head and neck have been reported in the literature
[5,7]. We will present our experience in treating a case of hydatid
cyst located in the subcutaneous neck area, which is considered
one of the few cases published due to the relative rarity of the
disease in the fore mentioned anatomical location.
A 36 year old man, who is not known to have any medical
history, presented to the head, neck and maxillofacial Surgery
department of Poorsina and Razi hospital, with a chief complaint
of a posterior under occipital and neck swelling, noted about
4 month back. The general condition of the patient was good; he
had no history of fever or weight loss. The patient lived almost
in a city near the mountain. He reported that the swelling was
gradually increasing in size with pain.
Clinical examination revealed a well-defined, non-tender
posterior and upperneck under occipital region swelling of
about 8 cm in diameter, other part of neck and scalp was normal.
Systemic examination of chest, abdomen and extremities was
unremarkable, On the ultrasonography (USG), a complex, cystic
lesion (10x4x5 mm) with septet and debris in the subcutaneous
adipose tissue was detected. On CT-scs in sagittal and coronal
view, a cystic lesion was presented in the base of skull posterior
ofneck (Figures 1-3). Anti-faciola tests was negative. Upon the
clinical diagnosis of the subcutaneous cyst, the patient underwent
surgery in prone position under general anesthesia. After prep
and derep and aspiration 30 CC clear fluid from cyst cavity (Figure 4). 30CC hypertonic salin was injected in the ruminant cavity.
After 10 minuet cyst was opened, a white laminated membranes
was exposed and removed intraoperative with presentation of
laminated membrane (Figure 4), our diagnosis was hydatid cyst.
The cavity was irrigated with providing-idon and was closed with
a external drainage. Histopathological examination confirmed the
diagnosis of the hydatid cyst. Serological tests were negative for the Echinococcal antigens. No pathology was seen onabdominal
andother organs in the CT-scnnand USG. The patient was started
on an oral albendazole (800mg/daly) treatment for 28 days with
14 day interval in three periods. On follow-up, no recurrence was observed.
Hydatid disease is caused by the larval tapeworm of the genus
Echinococcus granulosus, E.multilocularis. E.granulosus is the
most common cause of hydatid disease [6]. the liver (50-70%)
and lung (20-30%) are the most common organ which involve
but may be found in any other organ of the body , including brain,
heart and bones and adrenal gland (<10%) [7]. It can also affect the
kidney, ureter, spleen, uterus, Fallopiantube, mesentery, pancreas,
diaphragm and muscles and subcutaneous [8]. Muscular hydatid
cysts may be primary, but may also occur secondarily when
cysts spread from other areas, either spontaneously or after
previous operations for hydatidosis in other regions of the body
[8,9]. Hydatid cysts in soft tissues are an unusual presentation
of hydatidosis [8]. Primary intramuscular hydatidosis is rare
because the intramuscular growth of cysts is hindered by the
muscle’s contractility, and by the lactic acid in the muscle.
Parasitic cysts tend to grow around the muscles of the neck,
trunk and roots of the limbs, perhaps because there is greater
vascularization and less muscular activity in these regions [2,8].
They develop very slowly and act as space-occupying lesions,
producing symptoms related to pressure on the surrounding
tissues [5]. Other possible primary locations of the disease must
be excluded by careful clinical and radiological examination
of the patient, and these examinations must form the basis of
the diagnosis. In particular, MRI images may identify various
patterns of intramuscular hydatidosis such as its peripheral rim,
peripheral edema, peripheral enhancement with gadolinium and
multilocular cystic lesion (daughter cysts) [2,3,8]. In our case we
used U&S and MRI for diagnosis. Percutaneous needle or Open
biopsy in this solid and cystic lesion risk for spreading must be
avoided [1,2]. Echinococcosis should be always suspected in differential diagnosis of cystic lesions in soft tissue until proven
otherwise. Once the diagnosis is established, the surgeon should
consider performing a radically [1,2,8].
The treatment of choice is complete surgical excision of the
cyst mass and thorough irrigation of the surrounding soft tissues
with hypertonic saline to prevent recurrence [5,10]. Before
the surrounding of cyst should de walling of with hypertonic
saline solution.Administration of benzimidazole derivatives
(albendasol) preoperatively and after surgery is advocated by
some authors [2,8]. In this case we use albendazole (800mg/
daily) after surgery. The patient must be kept under clinical
evaluation after surgery, for recurrence. Once the diagnosis is
established, the surgeon should consider performing a radical
procedure aiming in minimizing the possibility of a recurrence.
The patient must be kept under clinical evaluation after surgery,
for recurrence.
In regions where hydatid disease is endemic, Echinococcosis
should be always suspected in differential diagnosis of cystic
lesions in soft tissue until proven otherwise. The best treatment
is the total excision of the cyst with an intact wall.
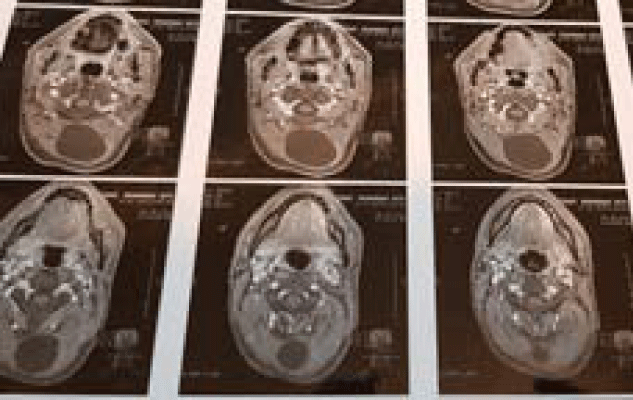 Figure 1: MRI of neck (T1 weighted, axial view) showing cystic lesion
the in sub-occipital area base of skull. View Figure
Figure 1: MRI of neck (T1 weighted, axial view) showing cystic lesion
the in sub-occipital area base of skull. View Figure
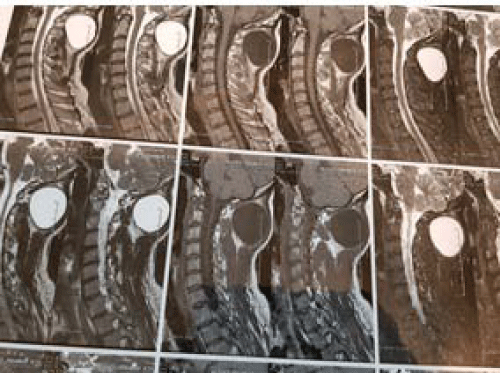 Figure 2: MRI of neck (T2 weighted, axial view) showing cystic lesion
in the neck just sub-occipital area. View Figure
Figure 2: MRI of neck (T2 weighted, axial view) showing cystic lesion
in the neck just sub-occipital area. View Figure
 Figure 3: Showing intraoperative aspiration of cystic lesion fluid. View Figure
Figure 3: Showing intraoperative aspiration of cystic lesion fluid. View Figure
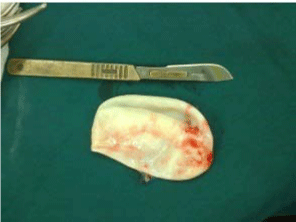 Figure 4: Showing Laminated membrane of cystic lesion, postoperative. View Figure
Figure 4: Showing Laminated membrane of cystic lesion, postoperative. View Figure