JSM Clinical Cytology and Pathology
-
Case ReportSuboccipital Solitary Fibrous Tumor Diagnosed by Fine Needle Aspiration: Report of an Uncommon Tumor in a Rare Location and a Brief Review of the LiteratureCarolina Fonseca*, Gilmar Costa, Soubhi Alhayek, Abdel-rahman El-Mallah, and Mohamad AzizDepartment of Pathology, American University of the Caribbean, 1 University Drive at Jordan Road Cupecoy, USA*Corresponding author: Carolina Fonseca, Department of Pathology, American University of the Caribbean, 1 University Drive at Jordan Road Cupecoy, 5980 Inkster Road, West Bloomfield, MI, USA, Tel: 530-220- 7996; Email: fonseca.carolina9@gmail.comSubmitted: 14 June 2019; Accepted: 26 June 2019; Published: 28 June 2019
-
Solitary fibrous tumors are rare and difficult to diagnose. The occurrence of this entity in the head and neck region constitutes approximately 6% of the cases and is associated with higher rates of recurrence. We report a case of a 61-year old male diagnosed with this rare tumor by fine needle aspiration.Keywords: Solitary fibrous tumor; Head and neck region; Cytology; Fine needle aspiration
-
SFT: Solitary Fibrous Tumor; FNA: Fine Needle AspirationSolitary fibrous tumor (SFT), also known as fibrous tumor of the pleura, is a rare mesenchymal tumor originating from the pleura or at virtually any site in the soft tissue. This tumor was first described by Klemperer and Rabin in 1931 [1]. These neoplasms are rare, mostly benign and they usually develop in the pleura. Extrapleural SFTs are rarer and 10 to 15% show malignant behavior [2]. The diagnosis of SFTs relies on the lesion’s histological appearance presenting with hemangiopericytic pattern composed of spindle cells proliferating in a “pattern less pattern” [3]. The over expression of CD34 and the lack of S-100 expression distinguishes these tumors from other spindle cell neoplasms [2-4].Solitary fibrous tumors of the head and neck region constitute approximately 6% of all SFTs. Due to its rarity, sufficient data describing this tumor are lacking. According to recent publications, head and neck SFTs tend to have higher rates of recurrence than similar tumors in other locations [5]. The risk of recurrence and metastasis seems to be associated with the size of the lesion, and the histological status of the margins of the excised tumor [2]. Given the fact that SFTs in the head and neck are rare and potentially malignant, it is important to increase physicians’ awareness of this particular tumor, and its inclusion in the differential diagnosis of soft tissue mass in the head and neck.A 61-year-old man presented with an enlarged sub occipital mass which had been present for years but had recently increased in size. Computed tomography of the neck demonstrated a heterogeneous appearing soft tissue mass in the suboccipital region which had increased in size – from 6.8 x 5 x 6.8 cm (6 months prior) to 9.8 x 5.7 x 8.5 cm. Peripheral areas of intense enhancement and prominent peripheral vessels were noted. The mass extended cephalad just above the inion of the occipital bone and caudally to the level of the C2 spinous process. The mass abutted the adjacent extensor musculature and extended into the subcutaneous tissues on the left producing a contour deformity of the overlying skin. There was mild cortical irregularity and lucency in the region of the inion not noted previously. Physicians suspected a soft tissue sarcoma and performed fine needle aspiration with core needle biopsy of the posterior suboccipital mass. Diagnostic material was obtained utilizing Fine Needle Aspiration (FNA). Cytology study revealed sheets, clusters, and single cells with bland cytomorphologic features and prominent plasmacytoid morphology predominantly in perivascular arrangements. Rare mitoses and no necrosis were noted (Figure 1A,B,C). An extended immunocytochemistry panel was performed for tumor characterization. The only two antibodies with positive and strong staining were CD34 and CD99 (Figure 1D) with focal weak positive chromogranin staining negative stains included: S100, HMB45, Melan-A, EMA, AE1/AE3, CAM5.2, HMW-CK903, P40, CD31, GFAP, CD163, Desmin, SMA, and Synaptophysin. The tumor proliferation was low with less than 2% nuclear staining with Ki-67. A diagnosis of low grade mesenchymal neoplasm, more specifically solitary fibrous Tumor was made.
-
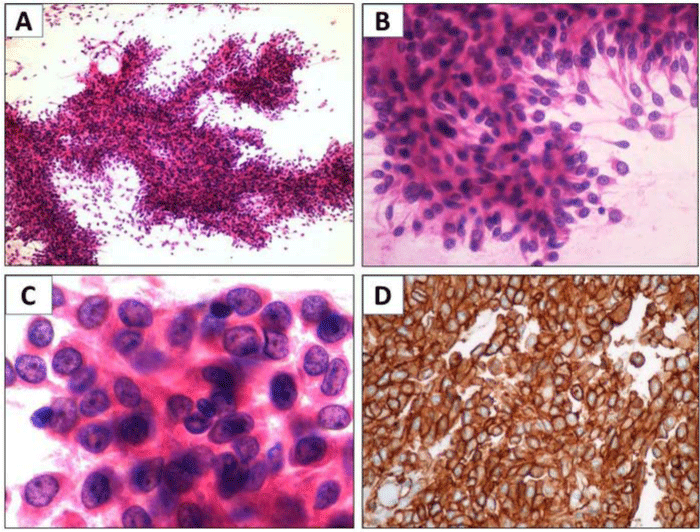 Figure 1: Fine needle aspiration of the subocciptal mass, cytology smears. View Figure
Figure 1: Fine needle aspiration of the subocciptal mass, cytology smears. View Figure
A & B: Sheets, clusters, and single spindle cells with bland cytomorphologic features composed of spindle cells proliferating in a “pattern less pattern” H&E stain; X 40
C: Prominent plasmacytoid morphology with mild atypical features showing irregular nuclear membrane, prominent nucleoli and no necrosis H&E stain; X 100
D: Immunocytochemistry CD99 positive for the tumor cells
The tumor was fully excised (10.2 x 8 cm) with wide safe margins. The patient did not require post-operative radiation or chemotherapy, and he was free of recurrence and metastasis at his 4 year follows up. Patient lost to follow up after that.We are presenting this case to contribute to the growing literature describing SFT and to emphasize that the diagnosis of SFT can be made on cytology samples alone including immunohistochemistry studies on cytologic preparation. The case being presented here was diagnosed with cytology sampling and immunohistochemistry alone. As emphasized by a recent publication in the Journal of Cytology, correctly diagnosing tumors like this preoperatively prompts an aggressive resection and decreases the chances of recurrence [6].The differential diagnosis of SFTs is broad and includes benign and malignant tumors [7]. The diagnosis can be difficult as the morphological features of this tumor overlap with a range of other myxoid spindle cell neoplasms such as dendritic fibromyxolipoma, lipomatoushemangiopericytoma, cellular angiofibroma and spindle cell lipoma [8]. The key features of SFT include abundant pale myxoid stroma, staghorn blood vessels and pattern less arrangement of spindle cells that are separated by collagen fibers [9-11].Only a few cases of solitary fibrous tumors in the occiptocervical region have been reported in the English literature, for this reason, physicians might not include this rare tumor in their list of differential diagnoses when presented with a mass in this region. However, extrapleural SFTs have been shown to present malignant behavior – including recurrence and metastasis [2] and should be considered in the differential diagnosis of extrapleural masses, particularly in the occiptocervical region [9]. The case presented here contributes to the recognition of this uncommon tumor in a rare location.Most recent molecular studies performed on SFT demonstrated numerous karyotypic aberrations in extrapleural SFTs. The most common included chromosome gain, loss and partial deletion. An intrachromosomal rearrangement has also been described. Although the etiology of the neoplasm remains largely unknown, the pathogenesis seems to be related to an NAB2–STAT6 fusion gene due to paracentric inversion on chromosome 12q13 [12].In 2014, a group of physicians reported a SFT that recurred ten years after the initial removal surgery and invaded the atlas [2]. This case exemplifies the potential malignant behavior of this particular tumor. The recurrence of SFTs in the head and neck region has been related to the incomplete excision of lesions [4,7]. This location is frequently regarded as challenging for surgeons, and it is not always feasible to attain clear surgical margins. When wide excision is not possible, marginal resection and radiotherapy may be an alternative treatment option if the patient is in low risk group according to the risk stratification model. And when wide excision is not possible close follow-ups including annual MRIs are recommended for at least 10 years [4,6,13]. Radiotherapy treatment has been suggested for patients with unresectable and/or recurrent tumors, but there is no data reporting the long term efficacy of this treatment approach [14,4].It is our hope that this report raises awareness of what remains an unmet need in the diagnosis and management of solitary fibrous tumors and that continued investigation drives further development of efficacious diagnosis and safe treatments for improving patient outcomes. -
-
- Klemperer PR. Primary neoplasms of the pleura. A report of five cases. Arch Pathol.1931; 11: 385-412.
- Tsutsumi N, Kojima Y, Nishida K, Maeno K, Kakutani K, Kawakami F. Surgical treatment for recurrent solitary fibrous tumor invading atlas. Head Neck.2014; 36: E121-E124.
- Piana S1, Putrino I, Cavazza A, Nigrisoli E. Solitary fibrous tumor of the spinal nerve rootlet: report of a case mimicking schwannoma. Arch Pathol Lab Med. 2004; 128: 335-337.
- Künzel J, Hainz M, Ziebart T, Pitz S, Ihler F, Strieth S, et al. Head and neck solitary fibrous tumors: a rare and challenging entity.Eur Arch Otorhinolaryngol. 2016; 273: 1589-1598.
- Smith SC, Gooding WE, Elkins M, Patel RM, Harms PW, McDaniel AS, et al. Solitary Fibrous Tumors of the Head and Neck.Am J Surg Pathol. 2017; 41: 1642-1656.
- Krishnamurthy V, Suchitha S, Asha M, Manjunath GV. Fine needle aspiration cytology of solitary fibrous tumor of the orbit." J Cytol. 2017; 34: 104-106.
- Cox DP, Daniels T, Jordan RC. Solitary fibrous tumor of the head and neck. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010; 110: 79-84.
- Hasegawa T, Matsuno Y, Shimoda T, Hasegawa F, Sano T, Hirohashi S. Extrathoracic solitary fibrous tumors: their histological variability and potentially aggressive behavior. Hum Pathol. 1999;30: 1464-1473.
- Hirakawa A, Miyamoto K, Hosoe H, Nishimoto Y, Shimokawa K, Shimizu K. Solitary fibrous tumor in the occipitocervical region: a case report. Spine. 2004; 29: 547-550.
- Vallat-Decouvelaere AV, Dry SM, Fletcher CD. Atypical and malignant solitary fibrous tumors in extrathoracic locations: evidence of their comparability to intra-thoracic tumors. Am J Surg Pathol.1998; 22: 1501-1511.
- Kim, Ji Hyun, Dong Chul Kim, Ryun Lee, Chi Ho Shin, Yea Sik Han, et al. Myxoid Solitary Fibrous Tumor on the Scalp. Arch Craniofac Surg. 2017; 18: 269-272.
- Ronchi A, Cozzolino I, Zito Marino F, Accardo M, Montella M, Panarese I, et al. Extrapleural solitary fibrous tumor: a distinct entity from pleural solitary fibrous tumor. An update on clinical, molecular and diagnostic features. Ann Diagn Pathol. 2018; 34: 142-150.
- Öztürk R, Arıkan ŞM, Şimşek MA, Özanlağan E, Güngör BŞ. Management of solitary fibrous tumors localized in extremity: case series and a review of the literature. Eklem Hastalik Cerrahisi.2017; 28: 121-127.
- Wushou A, Miao XC, Shao ZM. Treatment outcome and prognostic factors of head and neck hemangiopericytoma: Meta‐analysis. Head Neck. 2015; 37: 1685-1690.