Purpose: This review aims to evaluate diagnostic performance of dual-energy computed tomography (DECT) in follow-up examinations
after endovascular aneurysm repair (EVAR) and its radiation dose estimates compared to the standard triphasic protocol.
Materials and methods: A systematic search was conducted. Articles were screened against the inclusion and exclusion criteria.
A narrative review of the literature was performed. A summary statistic table of the calculated mean effective dose, percentages in dose
reduction and diagnostic performance of DECT were pooled.
Results: Data from the DECT acquisitions suggested a 98-100% overall accuracy for detecting type I and II endoleaks. The effective
dose delivered in the DECT protocol was approximately 61% lower than that delivered to patients by the standard triphasic protocol.
Conclusion: A DECT protocol can replace the standard triphasic protocol in follow-up imaging after EVAR for detecting type I and II
endoleaks. This acquisition protocol also significantly reduces the effective dose to the patients.
Keywords: Diagnostic Performance; Radiation Dose; EVAR; Endovascular Aneurysm
Since the introduction of endovascular aneurysm repair
(EVAR) by Parodi and his colleagues in 1991, this treatment
has become widely accepted for thoracic and abdominal aortic
aneurysms. It is also a more viable alternative to open surgical
repair with significant reductions in complications and mortality
[1,2]. Nevertheless, after this procedure, continuous imaging
surveillance is required to evaluate for potential complications
such as occlusion, stent migration, arteriovenous fistula formation
and endoleaks [3,4]. It is important to note that endoleaks are the
most common acute and delayed complication after EVAR which
occurs in up to 45% of all patients [5,6]. As this complication
might cause an enlargement of the aneurysm and hence
exacerbate the rupture risk, early detection and treatment are essential [7]. Multiple imaging techniques have been proposed
and utilized for the detection and classification of endoleaks for
the surveillance of patients who have undergone EVAR. These
include computed tomography (CT), magnetic resonance imaging
and ultrasonography [8].. Contrast-enhanced CT is the modality
of choice [9]. (Endoleak detection using CT is simply assessing a
peri-graft flow that reflects the flow of contrast out of the stentgraft
and into the aneurysmal sec [10]. The optimal contrastenhanced
CT imaging protocol, however, is still in discussion. The
literature has suggested that triphasic protocol is most commonly
used, including a non-contrast phase, an arterial phase during
contrast administration and a delayed phase to optimize the
detection of endoleaks [11,12]. Although this protocol is efficient,
after EVAR, patients are required to attend indefinite followups
and are exposed to substantial accumulative radiation dose
and hence, increased lifelong risk of developing cancers [13].
Therefore, considerable effort and research have been made
to examine the possibility of decreasing CT acquisition phases
without compromising diagnostic performance of the scan [9].
As such, a study by [14], has reported a comparable diagnostic
accuracy for endoleak detection by merely using the non-contrast
and delayed phases and ultimately suggested an elimination of
the arterial phase.
In the past decade, the use of dual-energy CT (DECT) has been
profoundly investigated and represents a promising advantage
in this field. With DECT, it is possible to simultaneously acquire
CT data with two different photon energy levels (typically at 80
and 140 kVp), resulting in different degrees of x-ray attenuation,
measured in House field units (HU) [15]. As a result, the difference
in energy spectra allows the software to characterize iodine,
calcium and other materials at low and high photon energies [16,17]. DECT has therefore been proposed as a preferable CT
technique because it has potential clinical implications in followup
imaging of patients after EVAR. The acquisition of dual-energy
data enables the generation of virtual non-contrast data which
might remove the need for a routine acquisition of true noncontrast
phase [18,16]. In effect, the use of this approach could
reduce the radiation burden to patients. To date, there has been
no literature review on the use of DECT protocol in patients
undergoing follow-up examinations after EVAR, especially
with the radiation dose associated with this protocol and the
diagnostic accuracy of this protocol compared to the standard
triphasic protocol.
Objectives
The purpose of this literature review is to evaluate the
following hypothesis and research questions:
DECT protocol can replace the standard triphasic protocol in
patients undergoing follow-up examinations after EVAR.
Research question 1
Does DECT protocol provide a significant dose reduction
relative to the standard triphasic protocol for these patients?
Research question 2
What is the diagnostic accuracy of DECT protocol in follow-up
examinations after EVAR, and how does its diagnostic accuracy
compare the standard triphasic protocol?
Selection criteria
A systematic search was conducted on 20th May 2018 on
the following databases: MEDLINE, PubMed, and Scopus. Terms
within each group were combined using “OR” and each group of
search terms were combined using “AND” (Table 1). The number
of hits for each database is outlined in Table 2. At the completion
of the database searches, results were pooled, and all duplicates
were removed.
Search strategy
The inclusion criteria were:
• The study:Was published between 2006 and 2018. This is because DECT technology was introduced in 2006.
• Was original and peer-reviewed.
• Reported quantitative measurements of the diagnostic accuracy of DECT in imaging follow-up of TEVAR.
The exclusion criteria were:
The study:
• Was published in languages other than English.
• Was conducted on non-human participants.
• Was a narrative review.
The rationale of excluding articles published prior to 2006
is because DECT technology was introduced in 2006 [16]. The
titles and abstracts of the original articles were initially screened.
Abstracts that were found to match the inclusion criteria were
obtained in full text to confirm their suitability for inclusion.
Articles not matching the eligibility were then excluded. All
articles meeting the above eligibility criteria were then included
in the literature review.
Results of the Literature Search
The literature search yielded 25 potential relevant articles
which were exported to EndNote X6 reference management tool
(Thomson Reuters, New York City, USA). After the removal of
duplicates, eight articles remained. Screening of abstracts and
titles resulted in the exclusion of one article. Screening of the full
texts of the remaining articles led to the exclusion of a further
two articles. A summary of the search and screening process is
provided in Figure 1.
Results
This literature review identified five original studies
assessing the potential radiation dose reduction in using a DECT
protocol and reporting the diagnostic accuracy of this protocol
in follow-up imaging after EVAR compared to standard triphasic
protocol [19,18,20-22,20]. However, only compare diagnostic
performance and radiation dose between the DECT protocol and
the biphasic protocol (no arterial phase was performed).
CT Acquisition protocol
All examinations in five studies were performed using a dualsource
DECT scanner (Somatom Definition, Siemens Medical
Solutions) [19,18,20-22]. A triphasic protocol was performed
and comprised of a non-contrast, an arterial and a delayed phase.
Besides the delayed phase being acquired in the dual-energy
mode, other phases were performed using the single-energy
mode. The dual-energy delayed phase was acquired 300-seconds
post-contrast injection because the timing has been reported
to be optimal for the detection and classification of low-flow
endoleaks (which is often missed during the arterial phase
[15,12]. The area of coverage was the same as the coverage range
for the non-contrast acquisition.
Radiation dose estimates
Due to a frequency of complications after EVAR, patients
need a lifelong follow-up imaging which is undertaken every
1-3 months after the procedure and every 6-12 months if the aneurysm is stable or decreases in size. As a result, to decrease
the radiation dose to patients having surveillance scans, the
number of acquisitions can be reduced [14]. For each of the CT
acquisitions, patient effective dose (ED) (mSv) was calculated
from the dose-length products (mGv x cm) recorded from the
CT console. A normalized conversion factor (k) for the chest
or abdomen was used to calculate ED (k was 0.014 and 0.017
mSv/mGy x cm, respectively) [15]. The calculated mean ED and
percentages in dose reduction was pooled from five studies (see Table 3).
The use of the DECT protocol resulted in a reduction in
radiation exposure of 61-64.1% compared with the exposure
from standard triphasic acquisition [19,18,21,22]. The study
by [20] only examined the dose differences between the DECT
protocol and the biphasic protocol (no arterial phase was
performed) which resulted in a reduction of 28% in dose. This
is particularly important in patients after EVAR as they will
undergo lifelong follow-up imaging examinations.
As stated previously, imaging during arterial phase is not
essential in diagnosing endoleaks [12]. However, if imaging is
performed immediately after EVAR, arterial phase is required
to evaluate arterial injuries such as arteriovenous fistulas and
pseudoaneurysms [19]. True non-contrast CT images may
also be beneficial after stent deployment for assessing type
IV endoleaks. This is because the isolated contrast material in
type IV endoleaks could be eliminated on virtual non-contrast
CT images [12]. Therefore, the use of a triphasic protocol is still
critical for immediate imaging after EVAR, but DECT protocol
should be then utilized in follow-up examinations to reduce the
patient’s radiation burden [12].
Five studies tested the feasibility of a single-phase DECT
protocol for endoleak detection using a dual-energy mode during
a delayed phase, without reducing diagnostic accuracy [19,18,20-
22]. The inter-rater agreement in the detection of endoleaks was
approximately 100% between the standard and DECT protocols
among all studies. Virtual non-contrast images were enough to
determine whether the high-attenuating material within the
aneurysm was a calcified thrombus or an endoleak. All endoleaks
were depicted during the delayed phase [19,18,20-22]. All studies have confirmed that DECT protocol has a potential to
replace the standard protocol in follow-up imaging after EVAR
with 98-100% overall accuracy for the detection of type I and II
endoleaks (see Table 4).
In-line with the literature [19,21] also reported results
comparing between DECT protocol and biphasic protocol (noncontrast
and delayed phases) and demonstrated that eliminating
the arterial phase does not significantly decrease the diagnostic
accuracy [12].
Limitations
There were some limitations found in these studies. First,
each study examined a relatively small number of participants/
patients (n=24, 48, 74, 118, 148 respectively) [19,18,20-22].
However, all studies have significantly demonstrated that true
non-contrast CT may not be necessary for the surveillance of
patients after EVAR. Secondly, only type I and II endoleaks were
included in all studies. Therefore, it is not possible to assess
the diagnostic performance of DECT in detecting type III, IV or
V endoleaks. However, these classifications are rarely observed
[21,23]. It is also important to note that due to the inherent
limitation in the DECT scanner, authors noticed a minimal oversubtraction
of the calcification in the virtual non-contrast images
compared to the calcification subtraction in the true non-contrast
images [19,24]. This could potentially result in a false-positive
diagnosis of endoleaks. A larger population might be able to
demonstrate this downside of DECT.
In summary, a virtual non-contrast and delayed phase
dataset reconstructed from a single DECT acquisition can replace
the standard triphasic protocol in follow-up imaging after EVAR
for the detection of type I and II endoleaks. Further technical
refinements and studies with larger population are required to accurately validate the diagnostic performance of this application.
This protocol also significantly reduces the effective dose to the patients.
 Table 1:Search terms for systematic review.
Table 1:Search terms for systematic review. 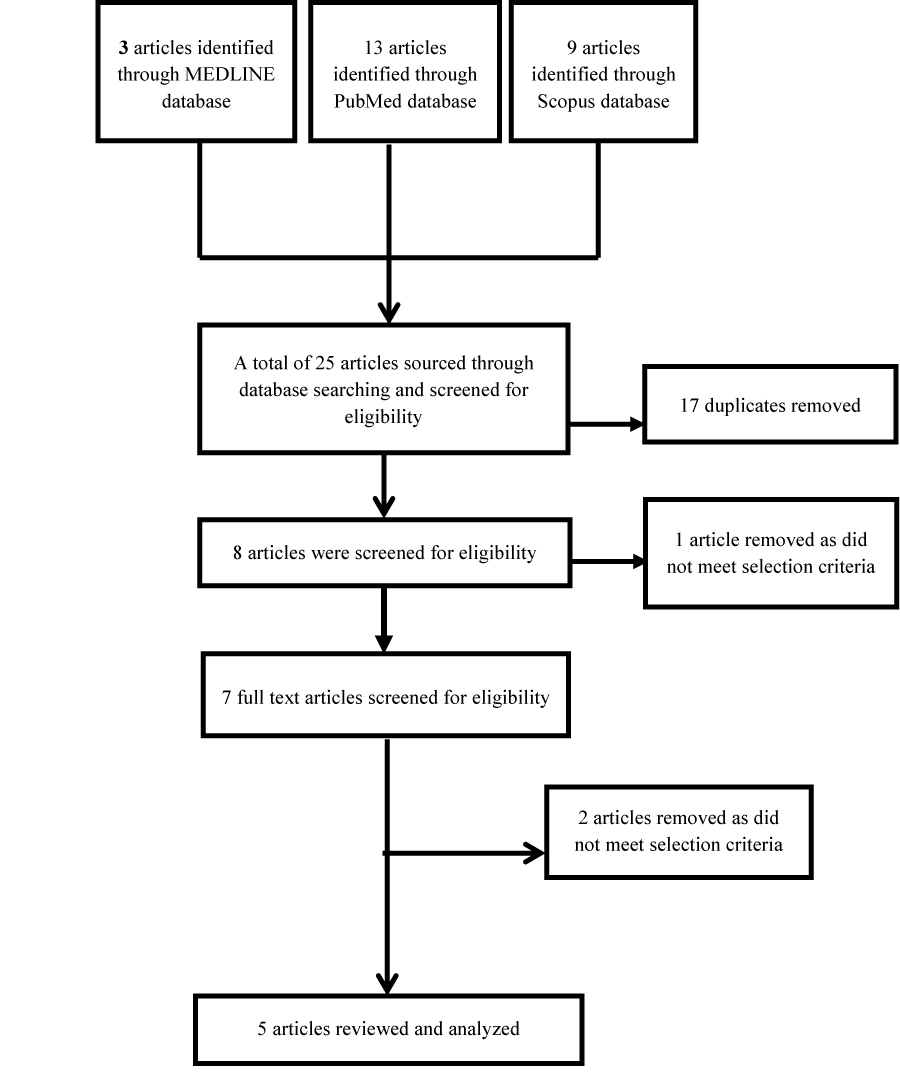 Figure 1: Modified PRISMA Flow diagram (Moher et al. 2015).
Figure 1: Modified PRISMA Flow diagram (Moher et al. 2015).