Case Report | Volume 4 - Issue 2 | Article DOI :
Download PDF
Hafed Amin Saidane¹, Mette Vinther Hansen¹, David Scheie² and Shanu Faerch Roemer¹*
¹Department of Neurology, Herlev Hospital, Denmark
²Department of Neuropathology, Rigshospitalet Blegdamsvej, Denmark
Corresponding Author:
Shanu Faerch Roemer, Department of Neurology, University of Copenhagen, Herlev Hospital, Denmark, Tel: +45 38 684246; Email: shanu.faerch.roemer@regionh.dk
Keywords
Parkinsonism; Central nervous system (CNS); Metastasis; Breast cancer
Abstract
We present a case of a woman with progressive parkinsonistic features, and a previous history of breast cancer with no recurrence since 20 years.
Case Presentation
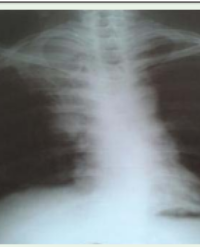
We present a 76-year-old Caucasian woman who was admitted to our Acute Neurology Ward. She had a previous history of hypertension, hypercholesterolemia, GERD, and non-metastatic HER2 positive breast cancer. The breast cancer successfully had been treated radically with left-sided mastectomy, axillary evacuation of nodules with no nodular spreading and no cancer recurrence since 20 years. The treatment was felt to be curative at the time of diagnosis and no concomitant radiation, chemotherapy or anti-HER-2 treatment was offered. Her oncological treatment and follow-up terminated one year after diagnosis of the localized breast cancer. The patient’s primary care provider had first referred her to an outpatient Clinic for Memory and Cognitive disorders due to restless legs syndrome, locomotor and progressive cognitive problems suggestive of dementia. Prior to referral, she presented with bradykinesia during 6 months and for one year she had been on medication for restless legs syndrome with pramipexol in the primary care sector. Both the patient and relatives had noted decreased locomotor speed and difficulty walking. The patient accepted giving-up driving a car. She was still responsible for financial matters with a previous job in bookkeeping, her husband, however, complained of new episodes of miscalculations. Due to progression in visuospatial dysfunction and visual hallucination within one year of diagnosis of Parkinsonism, a diagnosis of Dementia with Lewy Bodies was suspected and the patient instead was admitted to an acute Neurology ward prior to her scheduled outpatient Memory Clinic appointment. On neurological evaluation she presented with non-tremor dominant parkinsonistic features including oligomimia, stooping shuffling gait, movement en-bloc, cork-wheel rigidity of upper limbs and positive pull-test. Finger-tapping bilaterally with decrement, left more than right, alternating movement with bradykinesia but without dysdiadokinesia, saccades were hypometric. There was no evidence of gaze palsy, retrocollis or frontal hyperactivity suggestive of Progressive Supranuclear Palsy. No spasticity or alien limb phenomenon was evident suggestive of Corticobasal degeneration. A bilateral proximal paresis of the hip was noted, however, deep tendon reflexes were normal. Of note, no signs of Babinski were present neither left nor right. Furthermore, the patient appeared moderately cognitively impaired with apraxia, visuospatial dysfunction, impaired immediate recall and memory. She also revealed signs of executive dysfunction including perseveration, disinhibition and poor judgement. Left-sided visual neglect was noted. Complaints had worsened within weeks including leg cramps and headache. Acute CT head, followed by MRI headand spine (Figure 1) were requested suspecting an expansive process, which was confirmed. MRI spine showed widespread leptomeningeal carcinomatosis throughout the spinal canal, with several intramedullary metastases. Whole-body FDG-PET CT confirmed widespread involvement as seen on MRI scans (Figure 1) but was negative for breast cancer recurrence and showed no additional lung or visceral cancer-spread.

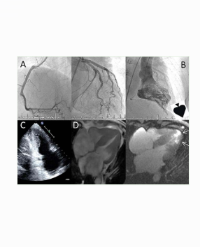
Figure 1: MRI brain reveals a large contrast-enhancing expansive process involving the right basal ganglia and frontal lobe edema, mass-effect and midline shift (A, B). MRI spine (C) and whole body FDG-PET CT with intramedullary metastasis (arrows).
A neurosurgical procedure was performed with stereotactic biopsy of the solitary brain right basal ganglia tumor, suspecting a brain neoplasm, possibly lymphoma due to patient age and medullary seeding, less likely an ependymoma with seeding. Neuropathological evaluation of the brain biopsy, excluded the tumor process to be due to malignant melanoma, glioma, lung cancer, colo-rectal-, bladder cancer or clear cell carcinoma, Surprisingly, the histopathological evaluation revealed a metastatic process which could clearly be distinguished from the surrounding brain tissue and revealed recurrence of the previous HER-2 positive adenocarcinoma (Figure 2). The patient received five sessions of palliative whole brain radiotherapy and was started anti-hormonal treatment. Her performance score, however, was already severely impaired at treatment initiation and the patient was not considered a candidate for adjuvant chemotherapy or antibody treatment. She was released to a hospice, still on anti-hormonal treatment and expired about one month after the diagnosis of breast-cancer brain metastasis.

Figure 2: A right frontal biopsy was performed showing a disorganized tumoral process with no clear evidence of glandular arrangement (A). Cells revealed pleomorphic nuclei and mitotic figures. Stains were negative for melan A, CD45, GFAP, TTF-1, CK-20, p40 and napsin (not shown). The tumor stained positive for CK7 (B), estrogen-receptor (C) and HER-2 (D) antibodies consistent with a metastatic process from previous breast cancer.
Discussion
This case report presents the rare case of a woman with isolated CNS involvement from a previous localized primary breast cancer. In concordance with the stage at initial breast cancer diagnosis, the patient was a disease-free survivor and had had no recurrence or metastatic disease during the past 20 years prior to admission. It is well known that HER-2 positive breast-cancer frequently metastasizes to the brain [1]. Several studies demonstrate a correlation with tumor stage and risk of brain metastasis [2]. However rare, it has been shown that HER-2 brain metastasis may occur even at 20 years of followup low-grade HER-2 positive breast-cancer [3,4]. In accordance with this, our patient had been diagnosed with grade II HER2- positive breast cancer 20 years prior to diagnosis of breast-cancer brain metastasis. Renewed mammography was not requested by the oncologist prior to the patient´s death, due to rapid deterioration at time of relapse. At time of breast cancer diagnosis the patient solely, underwent left-sided mastectomy and axillary evacuation of lymph nodes revealing no metastatic spread to any lymph-node station (n=11) and no adjuvant treatment was initiated. Isolated widespread CNS involvement with no obvious evidence of tumor recurrence extracranially 20 years after initial breast cancer diagnosis is unusual. One may hypothesize that a HER-2 positive low malignant cancer cell clone might have nested in the CNS and escaped immunosurveillance being trapped behind a closed blood-brain barrier.
Although, rapid progression of Parkinsonism with progressive cognitive symptoms such as hallucination is highly consistent with a clinical diagnosis of dementia with Lewy body, any neurological symptoms in patients with previous HER-2 positive breast-cancer irrespective of previous tumor grade and disease-free interval should prompt consideration of requesting an immediate brain scan in order to exclude CNS metastasis. Of note, the patient did not have any complaints of headache in the months ahead of admission, a red-flag which would otherwise guard most health care providers, and possibly correlated to the development of mass effect seen on MRI scans (Figure 1). This case highlights the need for awareness of long-term breastcancer brain metastasis, even in low-grade HER-2 positive patients.
The widespread metastatic disease of brain and spinal cord at time of diagnosis in our patient was rapidly fatal. Long-term survival (>5 yrs) of metastatic HER-2 brain metastasis has been reported, especially in patients receiving adjuvant treatment [5]. Although, speculative, a scan of both brain and spinal cord at time of prodromal Parkinsonian symptoms such as restless legs syndrome or at time of presentation of Parkinsonism, might have led to a more favorable outcome in our patient.
Acknowledgement
Consent was obtained from the patient and relatives prior to the patient’s death.
References
1. Kabraji S, Ni J, Lin N, Xie S, Winer EP, Zhao JJ. Drug resistance in HER2- positive breast cancer brain metastases: blame the barrier or the brain? Clin Cancer Res. 2018: 1078-0432.
2. Azim HA, Abdel-Malek R, Kassem L. Predicting Brain Metastasis in Breast Cancer Patients: Stage Versus Biology. Clin Breast Cancer. 2018; 18: 187- 195.
3. Pan H, Gray R, Braybrooke J, Davies C, Taylor C, McGale P, et al. 20-Year Risks of Breast-Cancer Recurrence after Stopping Endocrine Therapy at 5 Years. N Engl J Med. 2017; 377: 1836-1846.
4. Saraf A, Grubb CS, Hwang ME, Tai CH, Wu CC, Jani A, et al. Breast cancer subtype and stage are prognostic of time from breast cancer diagnosis to brain metastasis development. J Neurooncol. 2017; 134: 453-463.
5. Murthy P, Kidwell KM, Schott AF, Merajver SD, Griggs JJ, Smerage JD, et al. Clinical predictors of long-term survival in HER2-positive metastatic breast cancer. Breast Cancer Res Treat. 2016; 155: 589-595.
Citation
Saidane HA, Hansen MV, Scheie D and Roemer SF. A Rare Cause of Parkinsonism. SM J Clin Med. 2018; 4(2): 1035.