Case Report | Volume 4 - Issue 3 | Article DOI :
Download PDF
James Granfortuna*
Department of Hematology and Oncology, Cone Health teaching affiliate UNC Chapel Hill Medical Center, USA
Corresponding Author:
James Granfortuna, Department of Hematology and Oncology, Cone Health teaching affiliate UNC Chapel Hill Medical Center, 1200 N Elm St, Greensboro, NC 27401, USA, Tel: 336-312-4050; Email: james. granfortuna@conehealth.com
Keywords
Brodifacoum Toxicity; Coagulopathy; Synthetic Cannabinoids; Long Acting Warfarin; Rat Poison
Abstract
A recent cluster of patients presenting with idiopathic, severe, coagulopathy was reported in Illinois and traced to contaminated cannabinoids. The contaminating substance was determined to be brodifacoum, a potent, long acting, rodenticide that inhibits vitamin K dependent clotting factor production. Since the original reports from the Midwest, multiple additional cases have been reported in at least 11 states. Brodifacoum toxicity has now reached the proportions of a public health crisis. Patients can present with bruising, epistaxis, oropharyngeal and gum bleeding, excessive menstrual bleeding, hematemesis, hematuria, flank pain, or abdominal pain mimicking an acute abdomen. We present a case of brodifacoum toxicity that was rapidly reversed with parenteral Vitamin K and K-centra, four factor clotting concentrate. The use of intermittent prothrombin complex concentrates has the ability to control life threatening hemorrhage and is a potential important adjunctive treatment to minimize use of large doses of vitamin K.
Case Report
Case history
A 54 year old male in good health except for treated hypertension and remote history of nephrolithiasis. One week prior to admission he developed flu like illness with epigastric discomfort then intermittent nausea and vomiting. He denied fever, chills, hematemesis, hematochezia, melena, or diarrhea. He had mild polymyalgias. He took an over the counter antiemetic, emetrol. On day 4 he began to experience bilateral flank pain radiating to the groin then sudden onset of gross hematuria. He saw his primary care physician on day 6. Urine is positive for blood and bacteria. Hemoglobin 11.7 gm.
Cipro prescribed for presumed urinary tract infection vs prostatitis. Over the next 4 days, he developed profound weakness, orthostatic dizziness, a pounding sensation in his chest, lower extremity swelling, and spontaneous, non traumatic bruising. Past Medical History: Hypertension on Amlodipine 10 mg, renal stones, no surgery except laser treatment of central serous retinopathy. No history of peptic ulcer disease, hepatitis, yellow jaundice, malaria, mononucleosis, or inflammatory arthritis.
Allergy: penicillin as a child: desquamation of skin of hands and feet Family History: Parents and one female sibling healthy. No family history of bleeding disorders. Social History: Divorced. Works in a sheet metal factory. 2 healthy adult children.
Stopped smoking cigarettes in 1999. Drinks 6 beers daily. Denied drug use including cocaine, marijuana, and synthetic marijuana derivatives. Review of Systems: No headache or change in vision except for recent blurred vision when he stood up. Positive intermittent gum bleeding.
Exam
Well nourished Caucasian man in no distress. BP 108/52 pulse107 regular respiration 16 Temperature 98.3
HEENT:large port wine birthmark right neck and face. No mass, exudate, ulcer, hemorrhage in oropharynx.
No cervical, supraclavicular, axillary, or inguinal adenopathy Lungs clear to auscultation and resonant to percussion Regular cardiac rhythm; no murmur, gallop, or rub Abdomen soft, non tender, no mass, no organomegaly,
Genito-urinary: no flank tenderness; circumcised penis, no exudate
Extremities: 2+ pedal edema
Vascular: carotid pulses 2+, no bruits; dorsalis pedis pulses 2+ symmetric; no cyanosis
Neurologic: awake, alert, oriented x 3; cranial nerves grossly normal, motor strength 5/5, reflexes 2+ symmetric at biceps & patellae. Upper body coordination normal. Fundi: optic discs sharp, no hemorrhage or exudate
Skin: diffuse petecchial rash lower extremities. Multiple areas of soft tissue ecchymoses at recent venipuncture site, medial thighs bilaterally, soft tissue of calves extending to dorsum of foot on the left, and down to the heel (Figure 1).

Figure 1: Extensive soft tissue hematomas and ecchymoses.
Initial lab
Hemoglobin 5.3, Hematocrit 14.7, WBC 5,400, 72% neutrophils, 15 lymphocytes, 12 monocytes, Platelets 205,000, uncorrected reticulocyte count 1.6%.
Prothrombin time: >90 seconds, INR>10; PTT: >200 seconds Na 130, glucose 139, BUN 17, creatinine 1.2 AST 15, ALT 12, bilirubin 0.7, 0.2 direct, LDH 123, Total Protein 4.9, Albumin 3.0, calcium 8.5.
Urine: yellow, clear, large positive hemoglobin, 0-5 RBCs, 0-5 WBCs, negative protein, negative nitrite.
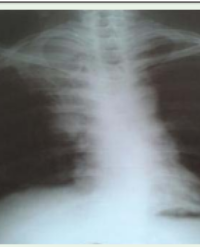
Imaging: non-contrast CT abdomen and pelvis with renal stone protocol showed extensive blood in retroperitoneum and renal collecting system (Figure 2).

Figure 2: (a) CT abdomen and pelvis: hemorrhage into the renal collecting system. (b) CT abdomen and pelvis: Extensive hemorrhage throughout the bilateral retro and extra peritoneal spaces.
Fibrinogen 503 mg%; d-dimer 1.0 (lab normal up to 0.48), COOMB’s direct antiglobulin test negative; Haptoglobin 217 Review of peripheral blood film: normochromic normocytic red cells, no spherocytes, schistocytes, polychromasia or inclusions, mature neutrophils, no toxic granulations, no early myeloid forms, mature lymphocytes, some of the monocytes appeared immature but not blastic, platelets normal in number and morphology.
Clinical course
PT/PTT repeated to exclude lab error and was reproducibly abnormal.
Sample sent to University hospital lab for plasma mixing studies and factor VIII level to rule out factor deficiency vs inhibitor to coagulation.
itamin K 10 mg IV administered. K-Centra 4 factor prothrombin complex concentrate given 25 units/kg.
Red cell transfusion given.
Repeat coagulation tests about 2 hours after K-centra showed near complete correction consistent with factor deficiency subsequently confirmed by plasma mixing studies and a factor VII level of 2% of control. Oral vitamin K continued daily. In less than 24 hours following K-centra, PT & PTT were rising and hemoglobin falling.
Additional K-centra and transfusions given hospital day 4. A thrombin time was done to exclude dysfibrinogenemia and was normal.
Factor VII returned at 2%; factor II,44%(50-154); factor V, 112% (70-150); factor X, 51%; factor VIII 310% (80-150).
On hospital day 5, patient again confronted re use of synthetic cannabinoid products which he denied on admission interview and now admitted to use on day before and day of appearance of his initial GI symptoms. Diagnosis was confirmed by a brodifacoum drug level of 27.1 microgram/ml sent to the Wisconsin State Laboratory of Hygiene, U of Wisconsin, Madison, WI. Daily vitamin K, 10 mg was continued.
Serial PT/INR and factor VII lab testing done. PT/INR normalized by day 28 after ingestion. The patient was kept on 10 mg of Vitamin K daily. On day 8 there was stabilization of his PT/INR at 22.9 seconds, INR 2.0. A factor VII level was up to 21%. By day 15, there was further improvement with PT/INR nearly normal and a concomitant factor VII level of 34%.
Discussion
Vitamin K is an essential cofactor for the enzyme gamma glutamyl carboxylase. Carboxylation of glutamate residues on a number of proteins, most importantly, some of the coagulation factors, results in their activation. Vitamin K antagonists inhibit the synthesis of Vitamin K dependent clotting factors II, VII, IX, and X. Their anticoagulant effect is due to interference in the cyclic conversion of Vitamin K 2,3-epoxide back to the reduced form of Vitamin K by Vitamin K epoxide reductase (VKOR). Partially carboxylated and decarboxylated proteins have reduced procoagulant activity. In 1940, Dicoumarol was shown to be the agent in sweet clover that induced hemorrhage in cattle. Warfarin, 4-hydroxy3(3-oxo-1-phenylbutyl) coumarin was developed as a more potent anticoagulant and initially used as a rodenticide until 1954 when it was approved for use as an anticoagulant in humans. Superwarfarins are chemically modified forms of warfarin developed when resistance to warfarin began to develop in rodents. Two derivatives with the highest toxicity are difenacoum and brodifacoum. Brodifacoum was found to be highly lethal in rats and other animals. It is estimated that a 15 mg amount would be lethal for a 60 kilogram human. In addition to being 100 times more potent in inhibiting vitamin K dependent clotting factors, with a tenfold higher affinity for the VKORC enzyme system, the addition of substituted phenyl rings significantly increases their hydrophobicity leading to enhanced tissue accumulation and retention and a prolonged half life of 30 days or greater compared with 36-42 hours for warfarin. This compound can stay in the system for months. The increased hydrophobicity is also felt to be associated with coagulant independent toxicities related to changes in capillary permeability and morphology. This may be particularly important with respect to nephrotoxicity and may result in glomerular hemorrhage, red cell cast formation and acute kidney injury. Accidental and intentional brodifacoum toxicity has been reported in thousands of people. One estimate is over 16,000 cases per year in the United States alone. Diffuse, multisystem bleeding is the common presenting manifestation including mucocutaneous sites, gastrointestinal, spontaneous hematomas, soft tissue and intramuscular hemorrhage, and rarely, intracranial bleeding [1-9].
On March 8, 2018, a cluster of cases of unexplained severe coagulopathy were reported in Illinois. (10,11,12).They were traced to synthetic cannabinoids found to be laced with brodifacoum. It is not certain whether the brodifacoum was added to enhance the euphoric effects of the cannabinoid or just purely for malicious reasons. The cannabinoid component is not detected on routine urine drug screening. These cannabinoids are not federally regulated and can be bought over the counter. A number of synthetic cannabinoids have been marketed under various names including K2, spice, yellow giant, black giant, and blue giant. They are usually sprinkled on herbal material and smoked but can also be obtained in a liquid form [10-13]. This patient purchased the material in a local Quickstop convenience store. This was the third reported case in North Carolina.
The same week that this patient was admitted to the hospital, the FDA issued a warning statement on July 19, 2018 [14]. This followed an initial clinical alert from the CDC posted on April 23. Since the initial reports, additional cases, now numbering over 150, have been reported in multiple states with at least 8 deaths. The North Carolina Department of Health and Human Services issued an alert for our state on 7/31/18 [15].
Brodifacoum contaminated cannabinoids present a major health hazard which can lead to prolonged coagulopathy and death. In some instances up to 100 mg of Vitamin K daily for weeks to months has been necessary to sustain clotting factor production. The average price of 5 mg of Vitamin K is approximately $70. One estimate of a 2 week course of treatment is $8,000 [10,11].
Although Brodifacoum inhibits the same vitamin K dependent clotting factors as warfarin and can be reversed with Vitamin K [16- 18], vitamin K may take a number of hours to reach its full effect and require repetitive, large doses, particularly when being used to reverse a long acting warfarin derivative. Prolonged use and high volumes of fresh frozen plasma are impractical. A four factor Prothrombin Complex concentrate (PCC) with increased levels of factor VII compared with previous PCCs became available in 2013 and has the capacity to rapidly reverse warfarin toxicity [19,20]. The availability of K-centra presents an important adjunct to Vitamin K therapy for the rapid reversal of severe warfarin related coagulopathy and is now the recommended product of choice per 2016 CHEST guidelines [21]. Optimal dosing is not established. Preliminary data suggests lower doses may be as effective as higher doses. We are looking at this prospectively at our institution. We chose a low dose regimen of 25 units per kilogram which proved to be highly effective and was only repeated one additional time.
Summary
A 54 year old man presented with acute soft tissue, genitourinary tract, and retroperitoneal bleeding. Prothrombin and Partial thromboplastin times were markedly elevated. Coagulopathy was rapidly and completed reversed with the initial use of both vitamin K and K-Centra four factor clotting concentrate then maintained with oral Vitamin K. Brodifacoum toxicity was suspected and subsequently confirmed.
This case illustrates the importance of a high clinical level of suspicion and prompt evaluation of an unexplained coagulopathy in persons who may have ingested a brodifacoum contaminated cannabinoid product and extends the use of K-centra 4 factor clotting concentrate as a rapid, although temporary, antidote when faced with life threatening hemorrhage.
References
1. Nathan King, Minh-Ha Tran. Long Acting Rodenticide (Superwarfarin) Poisoning: A review of its historical development, epidemiology, and clinical management. Transfusion Medicine Reviews. 2015; 29: 250-258.
2. Feinstein DL, Akpa BS, Ayee MA, Boullerne AI, Braun D, Brodsky SV, et al. The Emerging threat of superwarfarins: history, detection, mechanisms, and counter mechanisms. Ann NY Academy of Sciences. 2016; 1374: 111-122.
3. Weitz JN, Sadowski JA, Furie BC, Moroose R, Kim H, Mount ME, et al. Surreptitious ingestion of a long acting vitamin K antagonist/rodenticide, brodifacoum: clinical and metabolic studies of 3 cases. Blood. 1990; 76: 2555-2559.
4. Chandra AB, Methuku NK, Huang Y. Prolonged coagulopathy secondary to superwarfarin brodifacom rodenticide ingestion. Blood. 2010; 116: 4425.
5. Anderson SL, Kattapurram RS, Marrs JC, Joseph NM. Intentional brodifacoum ingestion. Am J Med. 2017; 130: 27.
6. Frando D, Everett G, Manoucheri M. I smell a rat: a case report and literature review of paradoxical thrombosis and hemorrhage in a patient with brodifacoum toxicity. Blood Coagulation Fibrinolysis. 2013; 24: 202-204.
7. Watson KS, Mills GM, Burton GV. Superwarfarin intoxication: two case reports and review of pathophysiology and patient management. J La State Med Soc. 2012; 164: 70-72.
8. Pavlu J, Harrington DJ, Voong K, Savidge GF, Jan-Mohamed R, Kaczmarski R, et al. Superwarfarin poisoning. Lancet. 2005; 365: 628.
9. Sharma P, Bently P. Of rats and men: superwarfarin toxicity. Lancet. 2005; 365: 552-553.
10. Outbreak Alert: Potential life threatening Vitamin K dependent antagonist coagulopathy associated with synthetic cannabinoid use. Centers for disease control and prevention (CDC). 2018.
11. Kelkar AH, Smith NK, Martial A, Moole H, Tarantino MD, Roberts JC. An outbreak of synthetic cannabinoid-associated coagulopathy in Illinois. NEJM. 2018; 379: 1216.
12. Conners JM. Hemorrhagic Highs from synthetic cannabinoids- A new Epidemic. NEJM. 2018; 379: 1275-1277.
13. Booth GS, Mody PZ. Brodifacoum inhalation and its clinical manifestations in a 21 year old Caucasian man. Lab Med. 2016; 47: 63-66.
14. Statement from Commissioner Scott Gottlieb, Peter Marks, Center for Biologics Evaluation and Research; and Janet Woodcock, Center for Drug Evaluation and Research. Statement from FDA warning about significant health risks of contaminated illegal synthetic cannabinoid products that are being encountered by the FDA. US Food and Drug Admin. 2018.
15. Moore Z. Update regarding Vitamin K dependent coagulopathy associated with synthetic cannabinoids use. WakeGOV: Public Health Alerts, Advisories and Updates. 2018.
16. Schulman S, Furie B. How I treat poisoning with vitamin K antagonists. Blood. 2015; 125: 438-442.
17. Thigpen JL, Limdi NA. Reversal of oral anticoagulation. Pharmacotherapy. 2013; 33: 1199-1213.
18. Gunja N, Coggins A, Bidny S. Management of intentional superwarfarin poisoning with long term vitamin K and brodifacoum levels. ClinToxicol (Phila). 2011; 49: 385-390.
19. K-centra: a 4 factor prothrombin complex concentrate for reversal of warfarin anticoagulation. Medical Letter Drug Ther. 2013; 55: 53-54.
20. Milling TJ, Refaai MA, Sarode R, Lewis B, Mangione A, Durn BL, et al. Safety of a 4 factor prothrombin complex concentrate vs plasma for Vitamin K Antagonist reversal: An integrated analysis of two Phase IIIb Clinical Trials. Acad Emerg Med. 2016; 23: 466.
21. Kearon C, Akl EA, Ornelas J, Blaivas A, Jimenez D, Bounameaux H, et al. Antithrombotic Therapy for VTE Disease: CHEST Guideline and Expert Panel Report. CHEST. 2016; 149: 315-352.
Citation
Granfortuna J. Brodifacoum Coagulopathy from Tainted Synthetic Cannabinoids. SM J Clin Med. 2018; 4(3): 1038.