Infrared Imaging Tools for Diagnostic Applications in Dermatology
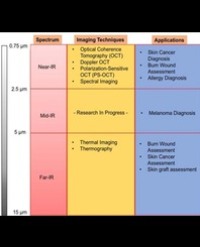
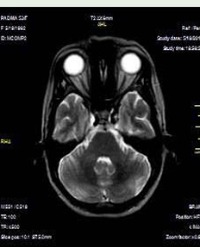
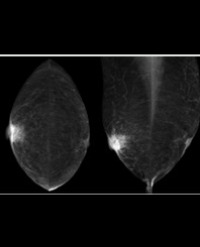
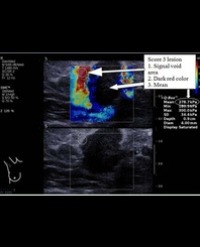
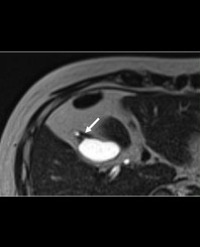
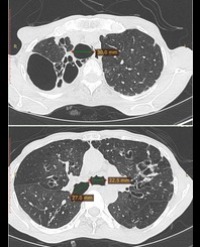
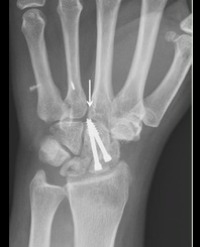
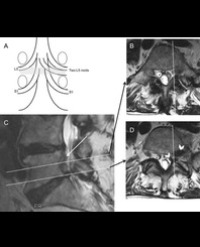
Infrared (IR) imaging is a collection of non-invasive imaging techniques that utilize the IR domain of the electromagnetic spectrum for tissue assessment. A subset of these techniques construct images using back reflected light, while other techniques rely on detection of IR radiation emitted by the tissue as a result of its temperature. Modern IR detectors sense thermal emissions and produce a heat map of surface temperature distribution in tissues. Thus, the IR spectrum offers a variety of imaging applications particularly useful in clinical diagnostic area, ranging from high-resolution, depth-resolved visualization of tissue to temperature variation assessment. These techniques have been helpful in the diagnosis of many medical conditions including skin/ breast cancer, arthritis, allergy, burns, and others. In this review, we discuss current roles of IR-imaging techniques for diagnostic applications in dermatology with an emphasis on skin cancer, allergies, blisters, burns and wounds.
Abhijit Achyut Gurjarpadhye1,2, Mansi Bharat Parekh1, Arita Dubnika1,3, Jayakumar Rajadas1,4, Mohammed Inayathullah1,5*