Case Report | Volume 3 - Issue 1 | Article DOI :
Download PDF
Alberto Schiarillo1, Anna Pensa1, Filippo Mariano2,3, Francesco Lupariello4, Catalina Ciocan5,6*, Daniela Risso1 and Maurizio Navissano1
1Plastic Surgery and Burn Center, Department of General and Specialized Surgery, AOU City of Health and Science, Italy
2Nephrology, Dialysis and Transplantation U, AOU City of Health and Science, Italy
3Department of Medical Sciences, University of Turin, Italy
4Department of Public Health and Pediatric Sciences, Forensic Medicine, University of Turin, Italy.
5Occupational Medicine U, AOU City of Health and Science, Italy 6Department of Public Health and Pediatric Sciences, Occupational Medicine, University of Turin, Italy
Corresponding Author:
Catalina Ciocan, Department of Public Health and Pediatric Sciences, Occupational Medicine, University of Turin, Italy, Tel: 0116933280
Keywords
Phenol Acid; Chemical Burns; Cutaneous; Multiorgan Failure.
Abstract
Aim: Describe the complications and management of a rare case of burn injury by phenolic acid.
Methods: A 45-year-old truck driver sustained a 35% total body surface area (TBSA) burn from an accidental phenolic acid injury. After initial treatment and decontamination with a polyethylene glycol solution, he arrived at the hospital intubated and on vasopressor support. No other traumatic injuries were found. Local assessment revealed a 35% TBSA burn of partial and full thickness on the perineal region, legs, right arm, and a small area of the abdomen. His Revised Baux score was 97. During his recovery, the patient developed hepatic insufficiency followed by renal failure, which required dialysis. A few days later, a total body CT scan revealed multiple ischemic cerebral areas. After 12 days from admission and episodes of bronchial bleeding, the patient died due to a multiorgan failure. A skin biopsy and toxicological analysis for phenol levels were performed during his hospital stay.
Results: In addition to the clinical case analysis, a review of the medical literature regarding cases of death following phenol burns, a histological analysis of the biopsy tissue collected and an analysis of the blood levels of phenol and its derivative o-cresol were conducted.
Conclusions: This case report illustrates the lethality of phenol chemical burns and emphasizes the critical role of multidisciplinary management in addressing multi-organ complications
Abstract
Aim: Describe the complications and management of a rare case of burn injury by phenolic acid. Methods: A 45-year-old truck driver sustained a 35% total body surface area (TBSA) burn from an accidental phenolic acid injury. After initial treatment and decontamination with a polyethylene glycol solution, he arrived at the hospital intubated and on vasopressor support. No other traumatic injuries were found. Local assessment revealed a 35% TBSA burn of partial and full thickness on the perineal region, legs, right arm, and a small area of the abdomen. His Revised Baux score was 97. During his recovery, the patient developed hepatic insufficiency followed by renal failure, which required dialysis. A few days later, a total body CT scan revealed multiple ischemic cerebral areas. After 12 days from admission and episodes of bronchial bleeding, the patient died due to a multiorgan failure. A skin biopsy and toxicological analysis for phenol levels were performed during his hospital stay. Results: In addition to the clinical case analysis, a review of the medical literature regarding cases of death following phenol burns, a histological analysis of the biopsy tissue collected and an analysis of the blood levels of phenol and its derivative o-cresol were conducted. Conclusions: This case report illustrates the lethality of phenol chemical burns and emphasizes the critical role of multidisciplinary management in addressing multi-organ complications
INTRODUCTION
Burn is an acute and complex injury caused by exposure of skin and/ or subcutaneous tissues to heat, cold, electricity, radiation, or chemical agents [1]. The clinical outcome may vary depending on the depth of the burn, the extension and the localization of the burn, the causal agent, additional diseases and the subsequent complications like infection and/ or metabolic conditions. Chemical burns account for only 3% of all burn injuries but 30% of deaths after burn injury are attributed to chemical burns [2]. Chemical products may be divided into acids, bases, organic compounds and inorganic compounds. Acids act by denaturing and coagulating proteins, alkaline burns cause deeper burns than acids with the saponification on the surface epithelium of the skin and laxity that causes necrosis. Organic solutions cause injury by dissolving the lipid membrane, leading to disruption of physiological processes. Inorganic solutions cause injury through denaturation mechanisms [3-5]. Phenol is a chemical compound both naturally occurring (colorless to-white solid) and manufactured (semi-volatile liquid). It is widely used in the production of phenolic resins, of nylon and other synthetic fibers [6], and as an antimicrobial agent for products, like throat lozenges, mouthwashes, antiseptic lotions, and gargles [7]. In medicine and cosmetics phenol is the most potent of all chemical peeling agents, inducing a controlled injury to the skin and leading to significant improvements in deep wrinkles, scars, and hyperpigmentation [8,9]. Due to its potential toxicity, phenol is included in the priority list of hazardous substances identified by the Agency for Toxic Substances and Disease Registry (ATSDR) [10]. This classification is based on its toxicity, frequency of occurrence at contaminated sites, and potential for human exposure. Since 2009, phenol has been banned in cosmetic products in Europe [11]. Acute phenol toxicity mainly occurs through accidental exposure in domestic environment or workplace [12]; Severe toxicity has been described from accidental ingestions in healthcare settings [13], while “Phenol marasmus” (historical syndrome of malaise, fatigue, and hepatitis) has been reported in recurring occupational exposures in explosives industry and healthcare settings [14]. Nowadays, phenol exposures are more likely to result in dermal exposure following laboratory or industrial spills [15]. Acute exposure may lead to severe tissue irritation and necrosis and central nervous system depression [16], as well as other systemic signs and symptoms like nausea, vomiting, diarrhea, methemoglobinemia, hemolytic anemia, profuse sweating, hypotension, arrhythmia, pulmonary edema and tachycardia. Phenol is readily absorbed through multiple routes of exposure (ingestion, dermal, inhalational) and distributes widely within minutes. It is believed to undergo hepatic metabolism via glucuronidation, sulfonation, and oxidation via CYP2E1 [10-18], than urinary excretion. Dermal absorbtion results in a white precipitate of coagulated proteins. In the absence of rapid decontamination deeper burns may occur leading to erythema, denaturation and gangrene followed by tissue necrosis. Notably, necrosis has been observed even with phenol concentrations as low as 1% [19]. The dermal absorbtion efficiency is almost equal to that of inhalation exposure [20], therefore systemic toxicity may occur rapidly following dermal contact.
Death risk increases exponentially for skin burns interesting sufaces larger than 400 cm² [10-20], and in patients with systemic intoxication. Death was reported in almost 50% of the cases with exposure levels sufficient to induce systemic effects. Systemic intoxication includes cardiovascular shock, cardiac arrhythmias, vomiting, lethargy, metabolic acidosis, hyperventilation, acute renal failure, and methemoglobinemia [21]. All ingestions or dermal exposures to phenol concentrations greater than 5% should undergo an emergency department evaluation. In the management of a phenol-poisoned patient the focus is on primary supportive measures such as ensuring a patent airway, supporting ventilation and oxygenation, and hemodynamic support as needed. Considering that there is no antidote for phenol intoxication, the most effective emergency response is to rapidly dilute phenol within the epidermis before it can be absorbed through the necrotic tissue by using low molecular weight (300-400MW) polyethylene glycol (LMW-PEG) as decontamination fluid [22,23]. When LMW PEG is unavailable, flushing the exposed area with copious amounts of water for 15 minutes may be effective.
CASE PRESENTATION
A 45-year-old man was transferred to the nearest emergency department after a severe chemical burn. The rescuers reported a truck driver injured by a jet of phenol acid while trying to fix the phenol tank cap. The patient reported extended chemical burns and respiratory distress after phenol inhalation. He was admitted intubated with a Glasgow Coma Scale (GCS) score of 3. No other injuries were reported after the CT scan. The skin was decontaminated with copious saline solution followed by cleansing with 50% polyethylene-glycol solution.
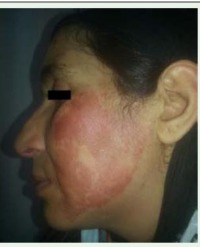
During the first six hours the patient presented 2 episodes of ventricular tachycardia. Six hours later, he was transferred to our regional Burn Centre of the Orthopedy and Trauma Center (CTO) in Turin, Italy. Upon arrival, he was re-intubated and sedated than cardiovascular support was provided with diuretics, amines, and fluid repletion according to the Parkland formula [24]. The burns were irrigated with standard saline solution. The initial assessment revealed partial and full-thickness burns covering 35% of the Total Body Surface Area (TBSA) on the perineal region, legs, right arm, and a small area of the abdomen (Figures 1,2). His Revised Baux score was 97 [25,26]. Within the first few hours, he developed severe acute kidney injury (AKI) with anuria and he underwent dialysis. In the following days, he developed severe hepatic dysfunction with indication for liver transplant. However, his liver function improved within 48 hours with only conservative therapy. Three days later a total body CT scan revealed ischemic cerebral damage, likely due to anoxia, as well as hemorrhagic pancreatitis and abdominal effusion without intestinal perforation. During his recovery, all the cultural tests were negative, including blood cultures during fever spikes, urine cultures, tracheal aspirate, and quantitative microbiology skin biopsies.

Figure 1 : Burns on the anterior surface of the lower limbs at day 3 post-admission, note the “infiltrated” appearance of the skin rather than necrotic.

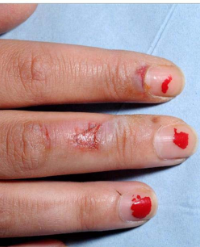
Figure 2 Detail of the burn evolution in the right leg on day 7 where appearance of vesicles is observed
During dialysis, phenol and o-cresol blood levels were monitored. The methodology and all data regarding phenol and o-cresol blood and urinary levels will be reported in a future publication. Regarding the burn wounds, there were no clearly demarcated areas of burn and the skin tissue did not appear frankly necrotic, therefore susceptible to spontaneous healing. For these reasons the first option was the conservative treatment. Under sedation, the burn wounds were irrigated with saline and an antiseptic solution every two days and medicated with antiseptic dressings. The fourth day skin biopsy was performed. He was treated with vasoactive support therapy and dialysis throughout the entire hospitalization. The 10th day, his medical condition was complicated by bronchial bleeding and disseminated intravascular caogulation with subsequent multiple organ failure. The patient died after 12 days. The autoptic exam confirmed the cause of death as multiorgan shock.
Skin biopsy
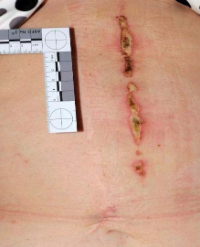
A skin sample was taken from the burn lesion of the left thigh on the fifth day of hospitalization. The sample was analyzed at the Pathology Department of our hospital. A fragment of skin with thin epidermis and linear profile, showing widespread epidermal necrosis and including areas of subepidermal and intraepidermal blister detachment located suprabasally at the orifice of follicular structures. The superficial and mid dermis is slightly thickened with mild inflammatory infiltrate characterized by granulocytic features and showing aspects of leukocytoclasis arranged in an interstitial manner and focally around blood vessels, with focal necrosis of the walls of small vascular structures. Focal erythrocytic extravasation (Figure 3).

Figure 3: Slides stained with hematoxylin and eosin at 20x magnification
Autopsy observations
At external examination, the body showed evolving sequelae of chemical burns in the areas already described in the clinical records, with partial- and full-thickness involvement of the skin. The internal examination revealed generalized cerebral edema, with markedly softened consistency of the brain parenchyma. The liver weighed 2,380 g and appeared markedly softened, with a parenchyma that, on section, displayed a conspicuously evident lobular architecture. The kidneys weighed 220 g (right) and 245 g (left), both showing reduced consistency and a poorly defined corticomedullary junction. These findings were consistent with the systemic distribution of phenol-related injury, affecting skin, central nervous system, liver, and kidneys, and corroborated the diagnosis of multiorgan failure as the cause of death.
LITERATURE REVIEW
A literature review was conducted aiming to assess all reported cases of phenol intoxication via transdermal contact. Only full-articles in English were selected. The first reported cases date back to 1868 in Birmingham [27]. On that occasion three women accidentally applied carbolic acid instead of Sulphur lotion, uniformly, over the entire body surface. Physicians recommended the skin decontamination by washing with warm water and soft soap. One of the three patients deceased about forty hours after the application of the acid, despite medical treatment attempts, considered valid at that time, including inducted emesis, application of leeches, administration of milk and brandy. RT Johnstone [28], reported in 1948, a case of a 22-year-old male who accidentally spilled a bottle of carbolic acid, saturating the “right leg, right side of the abdomen and the chest”. The colleagues immediately removed his shirt and threw water over the upper part of his body. He then went on his own to a physician’s office, but fifteen minutes after his arrival he collapsed and died. The autopsy revealed, in addition to the local first-and second-degree burns, “hyperemia and edema of the lower lobes of both lungs, and marked hyperemia and edema of both kidneys, pancreas and spleen”. No cardiac or hepatic alterations were reported. Pancreas, spleen and kidneys tested positive for carbolic acid, and the chemist reported a level five times higher than the usual level found in these tissues at autopsy. In 1949, Cronin and Brauer [29], described a case in which a 10-year old boy who was hospitalized with serious burns was treated dermally with 7.5 L of an antiseptic solution containing 2% phenol for 2.5 days. During this period his urine became dark and his respiration became labored, fell into a coma, and died. Postmortem analysis of urine showed the presence of 200 mg/L of conjugated phenol. In 1973 Griffith [30], describes a case of a young man of 23 y.o deceased ten minutes after a spray of liquid phenol covered his thighs. It was estimated that the area involved was 25 per cent of the total skin surface. Post mortem findings revealed that there was acute hemorrhagic congestion of both lungs, acute haemorrhagic congestion of liver and spleen and intense oedema of the kidneys, with scattered haemorrhage. The cause of death was cardiac and respiratory depression due to acute phenol poisoning.
In 1982, Soares and Tiff [31], reported two fatal cases attributed to absorption of phenol through intact skin. One was a 17-year-old male who died within 30 minutes after accidental contact with a 30% phenol solution. The affected areas were the face, neck, and the right side of the trunk. The other case was a 4-week-old baby girl whose seborrheic dermatitis was mistakenly treated with undiluted Castellani’s paint (a mixture of phenol, basic fuchsin, resorcinol, acetone, ethanol, and water). She deceased 5 hours later. In 1994 Horsh [32], described the case of a 22-year-old male, injured by a water-phenol solution during repair work on a pipeline valve. He weighed 85 kg for 194 cm height. The solution covered his face, chest wall, hand and both arms for a total burned surface area (TBSA) of 20.5 per cent. The patient acused nausea and vomit. His burns were treated with silver sulphadiazine ointment. Subsequently the patient recovered and the lesions healed completely within 12 days. In 1997, DeBono R e coll [33], strongly recommended for further precautions to be added to the instructions on phenolic household disinfectant bottles. They described the case of a 65-year-old male that referred to their unit with painless, fulll-thickness burns to his right hand after using a phenolic household disinfectant for carpet cleaning 6 days previously. The patient used a mop for cleaning and used both hands (bare) to squeeze the mop. Three days after, he noticed that parts of the skin of his right hand had become pale grey and blistered and after other 2 days the skin patches turned black. On examination he was found to have full-thickness chemical burns and digital tip gangrene. The affected areas were completely painless and anaesthetic. The wounds were thoroughly irrigated with 0.9 per cent saline and treated conservatively using a Flamazine hand bag and early physiotherapy. The dead tissue eventually sloughed off and was replaced with granulation tissue which epithelialized uneventfully. Another case of acute severe phenol dermal burn after accidental phenol splash was described by Parikh TJ in 2015 [34]. The author reported the case of a 35-year-old patient who was brought to the hospital 90 min after massive exposure to a 94% phenol solution. Decontamination was done with high-density water and glycerol. Early complications in the form of metabolic acidosis and acute renal failure required hemodialysis. Patient also developed pleural effusion and acute respiratory distress syndrome treated with draining and noninvasive ventilation. Even though he suffered multiple organ failures and extended burn the patient survived. The case of a 9-year-old girl exposed to Creolin(®) was reported by Vearrier D and coll in 2015 [35]. The mother applied Creolin(®)to the girl’s head and upper torso. The patient presented with signs of cutaneous and systemic phenol toxicity characterized by dermal burns, depressed mental status, cardiac dysrhythmias, and elevated hepatic transaminases but she responded very well to treatment. She was discharged to home on the fourth day. Sugden P [36], reported in 2001 the case of a 15-year-old apprentice footballer s admitted with a history of recurrent bilateral in growing great toenails, having previously had unsuccessful wedge excisions. He was previously treated in the orthopaedic unit of an outlying hospital with bilateral Zadik’s procedure with phenol ablation. Three days postoperatively he presented burns to the dorsum of both great toes. Initially these were treated with dressings and he was referred to another hospital for plastic surgery evaluation. On examination there was a full thickness burn to the dorsum of the left great toe with a large soft tissue defect exposing the distal phalanx, the right great toe had a smaller area of skin necrosis. Under general anaesthesia the necrotic tissue was débrided from the left toe, leaving most of the distal phalanx exposed. This necessitated amputation of the distal phalanx and the healthy plantar skin was used as a flap to achieve soft tissue coverage. The right toe required minimal débridement and was treated conservatively. Both toes healed satisfactorily with no further complications. A study conducted at Kaohsiung Medical University Chung-Ho Memorial Hospital, Taiwan [37], included four cases of phenol dermal burn. Data were retrospectively analyzed. The victims were all male with a mean age of 44 years old. Cases 1 and 2 had suffered from a 10% total body surface area (TBSA), second-degree burn caused by 99% phenol in the same accident, which resulted from a sudden explosion of a conveying hose. Case 1 had face, neck, and trunk burns; Case 2 face, neck, and left upper extremity burns. Case 3 was a victim of an abrupt explosion of a container with 95% phenol and had a 10% TBSA second- to third-degree burn over the face and left lower extremity. Case 4 had been injured by a spill-out of 15% phenol which resulted in his face, shoulder, and lower extremities suffering a 7% TBSA second-degree burn. They all received copious water irritation for at least 30 min in the first aid. PEG 400, was applied on burned areas in three cases as further decontamination. Mild interstitial pulmonary edema in the left lung was observed in Case 4 for the first four admission days which improved 3 days after intensive pulmonary care. Because the phenol burn involved facial areas, all 4 cases reported ophthalmologic problems (mild conjunctivitis, superficial punctate keratitis and severe keratitis) An initial elevation of liver function (GOT and GPT value) was noted in the first 3–5 post-burn days. All of the wounds had good response to silver sulfadiazine ointment and healed completely 10–14 days after burn. The wounds were all uneventful at the regular follow-up except uneven hypo- / hyper-pigmentation over the burn areas and imperceptible hypertrophy scars. In 2016 Li Z. [38], described a case of 21-year-old man who underwent an attempted removal of a large tattoo utilizing a tattoo machine that injected a phenol-containing solution. At the end of the 3 hours procedure, he collapsed and died. At autopsy, large areas of white skin discoloration with focal necrosis and sloughing were present overlying areas of previous tattooing. Toxicology was positive for phenol in cardiac blood and liver tissue and death most likely arose from cardiotoxicity. On April 26, 2018, a 55-year-old male patient with severe phenol burn complicated with acute poisoning was admitted to the Second Affiliated Hospital of Zhejiang University School of Medicine [39]. The patient rapidly developed multi organ failure manifested by altered consciousness and restlessness, anuria, and respiratory failure. He received early treatment including wound decontamination, rapid massive infusion and hemodialysis, hemoperfusion, continuous renal replacement therapy for speeding up phenol excretion and organ function maintenance. The patient recovered successfully and was discharged on post injury day 29. The most recent case reported [40], was an industrial resin worker who suffered phenol burns in both lower extremities due to a work accident. The estimated total body surface area (TBSA) was 11%. The change in skin tone and pigmentation after exposure to phenol suggested the possibility of full-thickness (third-degree) burns; however, contrary to the gross finding of burns, the actual depth was equivalent to a second degree burn. His wound showed signs of epithelialization 7 days after the burn injury without debridement or skin grafting, with daily water irrigation and dressing alone. The patient was discharged from the hospital on day 2.
DISCUSSION
Phenol is a highly toxic compound capable of causing systemic toxicity even when absorbed through intact skin. Our case illustrates a rare but catastrophic outcome of accidental occupational phenol exposure, resulting in severe burns, multiple organ failure, and death, despite early decontamination and intensive supportive care.
Compared to previous reports, our patient presented with one of the most extensive phenol-related injuries documented, with a TBSA of approximately 35% involving critical anatomical regions. While the literature contains several fatal cases following phenol exposure involving smaller surface areas, most deaths occurred rapidly—often within minutes or hours—due to sudden cardiovascular collapse or respiratory arrest [27-30]. In contrast, our patient survived for 12 days, suggesting that early decontamination with polyethylene glycol and intensive support, including continuous renal replacement therapy, may have prolonged survival, albeit without altering the fatal outcome once systemic injury had occurred. The systemic effects seen in our case were severe and coherent with previously reported literature data. Similar to other reported cases [21-28], acute kidney injury occurred within hours. Shortly after the hepatic insufficiency, coagulopathy and cerebral ischemia have installed underlining the extensive multisystem involvement. Although hepatic transplant was considered, the liver parameters showed partial spontaneous improvement, confirming the potential reversibility of hepatic toxicity if support is maintained. The decision for conservative wound management was consistent with recent reports, such as the case by Shigeno A e coll. [40], which highlighted the difficulty in accurately assessing burn depth in phenol injuries. In our patient, clinical evaluation has been made difficult by the protein-coagulating effect of phenol, which creates a leathery eschar that may not reflect true depth. Histological analysis ultimately confirmed full-thickness injury, supporting conservative debridement followed by targeted interventions rather than early excision. The literature review reveals that phenol-related deaths have been described for over a century, with surprisingly similar clinical features: rapid CNS depression, cardiovascular instability, renal and hepatic failure. These findings persist despite advances in critical care, largely due to phenol’s intrinsic properties—lipophilicity, rapid absorption, and direct cellular toxicity. What distinguishes our case is the combination of delayed mortality, serial toxin level monitoring, and detailed supportive care documentation, which provides valuable insight into the natural course and potential therapeutic windows in phenol poisoning. Despite all efforts, the patient’s deterioration into bronchial hemorrhage and disseminated intravascular coagulation (DIC) marked the onset of irreversible shock. This case also underlines that phenol exposure should be considered a life-threatening emergency, especially when TBSA exceeds 10%. Although there is no antidote, decontamination with PEG remains the gold standard and should be initiated as soon as possible. In the clinical management of the patient blood and urine monitoring for phenol and metabolites can guide understanding even though it does not predict the outcome. There is strong evidence conservative wound care is appropriate in the initial management. In the absence of a specific antidote, supportive treatment remains the cornerstone. Last but not least, our experience highlights the lethality of phenol burns and underlines the importance of occupational safety measures, rapid emergency protocols, and ongoing research into effective detoxification strategies.
CONCLUSION
Although rare, fatal outcomes from phenol burns have been consistently documented over the past 150 years, highlighting the potent systemic toxicity of this compound when absorbed through the skin. The cases reviewed show that death may occur within minutes to hours of exposure, even with limited total body surface area (TBSA) involvement, and that neither the presence of full-thickness burns nor the absence of external damage reliably predict severity. Systemic absorption through intact or compromised skin can rapidly lead to multiorgan dysfunction, including acute kidney injury, hepatic congestion, pulmonary edema, metabolic acidosis, and cardiotoxicity. The clinical evolution often progresses very fast, emphasizing the need for immediate and effective decontamination. Notably, even with aggressive supportive care, the prognosis in extensive exposures or when early organ failure is present remains poor. Several factors appear to influence outcomes: phenol concentration, delay in decontamination, TBSA affected, and the anatomical site of exposure. Children and individuals with facial or mucosal involvement seem particularly vulnerable, as demonstrated by the rapid deterioration seen in pediatric and facial exposure cases. Despite some recent reports of survival after significant phenol exposure, thanks to prompt intervention and modern supportive therapies, the margin between survival and fatality remains narrow. These findings reinforce the critical importance of industrial safety protocols, early recognition, and emergency management of phenol exposure. Future research should aim to define standardized treatment algorithms and improve strategies to limit dermal absorption and systemic toxicity.
REFERENCES
- Diler B, Dalgic N, Karadag CA, Dokucu AI. Epidemiology and infections in a pediatric burn unit: experience of three years. Çocuk Enfeksiyon Dergisi/J Pediatr Infect. 2012; 6: 40-45.
- Luterman A, Curreri P. Chemical burn injury. In: Jurkiewcz M, Krizek T, Mathes S, editors. Plastic surgery: principles and practice. St. Louis, MO: Mosby. 1990: 1355-440.
- Richards A, Dafydd H. Key Notes on Plastic Surgery. Chichester, UK: John Wiley & Sons, Ltd. 2014.
- Kozawa S, Kakizaki E, Muraoka E, Koketsu H, Setoyama M, YukawaN. An autopsy case of chemical burns by hydrochloric acid. Leg Med(Tokyo). 2009; 11: S535-S537.
- Akelma H, Karahan ZA. Rare chemical burns: Review of theLiterature. Int Wound J. 2019; 16: 1330-1338.
- Toxicological Profile for Phenol. Atlanta (GA): Agency for Toxic Substances and Disease Registry (US). 2008.
- Substance-Specific Applied Research Program Priority Data Needs: Phenol [Internet]. Agency for Toxic Substances and Disease Registry/ Division of Toxicology and Environmental Medicine (ATSDR/DTEM). 2009.
- Stuzin JM. Phenol peeling and the history of phenol peeling. Clin Plast Surg. 1998; 25: 1-19.
- Bensimon RH. Croton oil peels. Aesthet Surg J. 2008; 28: 33-45.
- Phenol | Toxic Substances | Toxic Substance Portal | ATSDR.
- Regulation - 1223/2009 - EN - Cosmetic Products Regulation - EUR- Lex.
- Downs JW, Wills BK. Phenol Toxicity. 2023.
- Haddad LM, Dimond KA, Schweistris JE. Phenol poisoning. JACEP. 1979; 8: 267-269.
- Merliss RR. Phenol marasmus. J Occup Med. 1972; 14: 55-56.
- Horch R, Spilker G, Stark GB. Phenol burns and intoxications. Burns.1994; 20: 45-50.
- IARC Working Group on the Evaluation of Carcinogenic Risks to Phenol. In: Re-evaluation of Some Organic Chemicals, Hydrazine and Hydrogen Peroxide. International Agency for Research on Cancer. 1989.
- Babich H, Davis DL. Phenol: a review of environmental and health risks. Regul Toxicol Pharmacol. 1981; 1: 90-109.
- Vearrier D, Jacobs D, Greenberg MI. Phenol Toxicity Following Cutaneous Exposure to Creolin®: A Case Report. J Med Toxicol. 2015; 11: 227-231.
- European Commission (luxembourg): Luxembourg. Summary Risk Assessment Report - ECHA. European Chemicals Bureau. 2006.
- Kucheki M, Simi A. Phenol Burn. The Int J Occup Environ Med. 2012;1: 41-44.
- International Programme on Chemical Safety (IPCS). inchem.org. Phenol (EHC 161, 1994). 1994.
- Conning DM, Hayes MJ. The dermal toxicity of phenol: an investigation of the most effective first-aid measures. Br J Ind Med. 1970; 27: 155-159.
- Hunter DM, Timerding BL, Leonard RB, McCalmont TH, SchwartzE. Effects of isopropyl alcohol, ethanol, and polyethylene glycol/ industrial methylated spirits in the treatment of acute phenol burns. Ann Emerg Med. 1992; 21: 1303-1307.
- Mehta M, Tudor GJ. Parkland Formula. 2025.
- Osler T, Glance LG, Hosmer DW. Simplified estimates of the probability of death after burn injuries: extending and updating the baux score. J Trauma. 2010; 68: 690-697.
- Christofides C, Moore R, Nel M. Baux Score as a Predictor of Mortality at the CHBAH Adult Burns Unit. J Surg Res. 2020; 251: 53-62.
- Machin ES. Fatal Cases of Poisoning by the Absorption of Carbolic Acid. Br Med J. 1868; 1: 220.
- Johnstone RT. Occupational medicine and industrial hygiene. St. Louis, THE C. V. MOSBY COMPANY. 1948: 216.
- CRONIN TD, BRAUER RO. Death due to phenol contained in foille; report of a case. J Am Med Assoc. 1949; 139: 777-779.
- Griffiths GJ. Fatal acute poisoning by intradermal absorption of phenol. Med Sci Law. 1973; 13: 46-48.
- Soares ER, Tift JP. Phenol poisoning: three fatal cases. J Forensic Sci.1982; 27: 729-731.
- Horch R, Spilker G, Stark GB. Phenol burns and intoxications. Burns.1994; 20: 45-50.
- DeBono R, Laitung G. Phenolic household disinfectants--further precautions required. Burns. 1997; 23: 182-185.
- Parikh TJ. Acute concentrated phenol dermal burns: Complications and management. Ind J Crit Care Med. 2015; 19: 280-282.
- Vearrier D, Jacobs D, Greenberg MI. Phenol Toxicity Following Cutaneous Exposure to Creolin®: A Case Report. J Med Toxicol. 2015; 11: 227-231.
- Sugden P, Levy M, Rao GS. Onychocryptosis-phenol burn fiasco.Burns. 2001; 27: 289-292.
- Lin TM, Lee SS, Lai CS, Lin SD. Phenol burn. Burns. 2006; 32: 517-521.
- Li Z, Zhang H, Li SH, Byard RW. Fatal Phenol Toxicity Following Attempted Tattoo Removal. J Forensic Sci. 2016; 61: 1143-1145.
- Pan Xuanliang, Chen Guoxian, You Chuangang, Han Chunmao, Wu Pengcheng. A case of severe phenol burns combined with acute poisoning. Chinese J Burns. 2020; 36: 746-747.
- Shigeno A, Miyao D, Futagami H, Nakajima S, Kuroki Y, Osuka A. Phenol burns treated with conservative therapy: A case report. Burns Open. 2024; 8: 115-119.
Citation
Schiarillo A, Pensa A, Mariano F, Lupariello F, Ciocan C et al, (2025) Fatal Multi-Organ Failure Following Occupational Chemical Burn after Exposure to Phenolic Acid: A Case Report and Literature Review, Ann Burns and Trauma 4: 7.