Methods for Determining Gingival Biotype
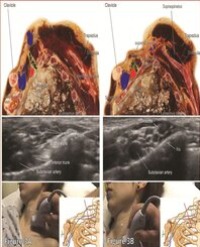
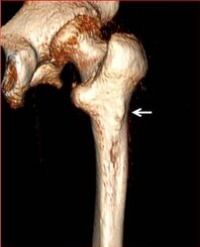
To quantify tissue thickness, a variety of invasive and non-invasive approaches have been developed. The visual examination direct methods include transgingival probing, endodontic reamers and files, probe transparency (TRAN), ultrasonic methods, and a cone-beam computed tomography (CBCT) scan are some of these options listed in Table 2.

Table 2:Different techniques available for the assessment of gingival biotype
Gingiva is visually assessed and evaluated based on its overall look during a visual examination. Benefits include: The extent of soft tissue cannot be measured using this procedure, which is simple and non-invasive. Due to a substantial inter examiner variation, accuracy is low (9).
Presurgical Oral Examination
The following should be covered in a comprehensive oral evaluation prior to surgery (10).
Quality and quantity of bone:The facial expression and labial position, and the grin can all be considerably influenced by the contour ,thickness, height, of the facial alveolar plate (11). The alveolar plate’s architecture varies greatly from one individual to another (12). It takes bone with a bucco-lingual diameter of 6 mm and a mesio-distal dimension of 5–6 mm to support the dwelling of a conventional 3.75–4 mm implant. Implant angulation affects the facial alveolar plate’s height and thickness. A broad, flat bone in the face that supports soft tissue in an abnormally more coronal position is connected to a lingual tilting of an implant. A thin, scalloped face alveolar bone that is frequently found in an apical position is linked to a labial implant inclination. The facial alveolar plate may need to be expanded both vertically and horizontally following implant insertion. For the overtime maintaining soft tissue height, this is crucial (13–15). The root positions of nearby teeth may contribute to boundaries in bone amount in the mesio-distal dimension. The required room for implant implantation may be created through orthodontic movement used to alter the position of the root. A smaller horizontal separation between teeth and an adjacent implant may negatively impact the level of bone on the tooth side(14).
Dental morphology
The anterior aesthetic area around the mouth is where this relationship between tooth form and periodontal biotype is most obvious. The tooth’s triangular form is connected to a narrow periodontium with scallops (Biotype I). The interproximal contact area of this biotype is connected to a long, thin papilla, and it is situated in the crown’s coronal third. The tooth’s connection to a thick, flat periodontium is square in shape (Biotype II)(2). A short, wide papilla is supported by the interproximal contact area, which is situated in the middle third of the crown (5).
Occlusion and occlusal forces: The linked bone density and thickness indicate the orientation, magnitude, and time of masticatory stresses on implants. The facial alveolar plate’s width and height appear to be negatively correlated with the angular implant forces. To focus as much of the masticatory forces as possible on an implant’s longitudinal shaft, occlusal correction may be necessary in order to achieve a favourable prognosis (16). To determine if an implant restoration would be in compliance with the demands of proper phonetics and occlusion, prosthodontic treatment planning is frequently necessary.
Adjacent periodontium: Nearby periodontally healthy teeth’s cemento-enamel junction and the crown-abutment junction mainly line up (17–19). The consequences of significantly reduced periodontium around teeth next to implants are (I) more substantial clinical implant crown and (ii) diminished papilla size or absence. To enable the restoration to blend with a natural profile, a conventional 3.75- or 4-mm-diameter implant should be positioned 3- 4 mm apical to the buccal soft tissue level of the neighbouring teeth. To provide allows a progressive change from the implant platform’s 4-mm diameter to the crown’s 7-8 mm size at the gingival edge, a vertical distance of 3-4 mm is required. If a maxillary lateral incisor needs to be replaced, the implant can be placed more coronally since there is less space needed for transition because the typical crown diameter at the gingival level is about 5 mm.
Lip position, lip mobility and smile line: The main anatomical aspect of the lips is their vermilion border, or the redness around the mouth. The vertical groove on the middle top lip, where the Vermilion-skin interface is most clearly marked, is referred to as the philtrum. The centre Vermilion beneath the philtrum is filled out by a clearly pronounced upper-lip tubercle. The site of the implants, the peri implant architecture, and the dental architecture all have a considerable impact on the tonus, form, and tubercle of the Vermilion, as well as the philtrum (20). In comparison to the maxilla, the mandible has less of a demand for an aesthetic result, allowing the dentist to place more of an emphasis on long-term implant health than on aesthetics.
Texture, volume, colour, and structure of soft tissue: The oral mucosa normally consists of a coral-pink masticatory mucosa and a glossy red alveolar mucosa (21). Collagen fibres make up the moveable alveolar mucosa loosely, and the epithelium is lacking rete pegs, nonkeratinized, and is thin. The masticatory mucosa’s epithelium, in contrast, is immovable, thick, keratinized, and made of dense, well-organized collagen fibres. The masticatory mucosa is stippled, robust, and securely linked to the periosteum, making it resistant to thermal, chemical, and physical stress (22). The upper lip’s contour is often parallel to the gingival border of the maxillary teeth. The canines and central incisors of the maxilla share a mucosal margin that is equal in height. In comparison to the canine and central incisor, the mucosal border of the maxillary lateral incisor is 0.5–1.0 mm more coronal. When someone smiles normally, the labial tone and location cause to be visible: 75–100% of the maxillary anterior teeth and any associated soft tissue (20).
Tissue Reaction to Therapy: Tissue biotypes are a major factor influencing the outcome of aesthetic treatment. The findings show that inflammation, trauma, and surgery affect these two tissue biotypes injury in different ways. Thick bone plates linked with thick biotypes respond differently to extraction than thin bone plates associated with thin biotypes. Thick biotypes minimize atrophy of the coat of arms after extraction (23).
However, extraction-induced trauma can result in fractures of thin biotype, labial apical and lingual plates and traumatic ridge resorption sides. Bone and gingival tissues differ between biotypes of thick and thin tissue, and these differences have a substantial influence on Preparation of the position of the implant and the treatment preparing the width of the gingival and bone uniformity of the apex and soft tissue is instantly tied to tissue (24). To build an aesthetics each prosthesis not to mention matches size, shape, and location, and colour of the next tooth, but also the soft tissue all over the tooth implant and the surrounding gingiva and mucosa, resulting in an aesthetically acceptable replacement to establish compatibility. It also aids in the preservation of bone structure. To achieve the best aesthetic effects, enhancement of both soft and rigid tissues should be done at the same time, performed in addition to implantation (25).
Indices: The ICAI, PES/WES, and a novel index called the “Peri-Implant and Crown Index (PICI),” which the authors had developed, were all approved and employed in Table 3. The PES/WES (pink aesthetic score/white aesthetic score) criteria, which include five white and five pink parameters, were utilised to compare the pink (PES) and white (WES) of single implant reconstructions to the contralateral tooth.
The ICAI was also utilised to compare the pink and white aesthetics reconstructions with a single implant to those of neighbouring and contralateral teeth. Table 3 lists the four pink and five white criteria that were evaluated and rated
Finally, the new PICI was developed for this study in order to compare the pink and white aesthetic qualities to the appearance of the contralateral tooth using visual analogue scales. Three pink, white, and subjective total criteria make up the PICI (Table 3).

Table 3:Guidelines for the three Esthetic Indices and Comparative Esthetic Calculation
The extreme left of the visual analogue scale for pink and white aesthetics suggests that the implant restoration will be totally different from the contralateral tooth while the right indicates that the crown of the implant will be similar to the tooth in contralateral side (26)
CEI (Criteria for Esthetic Index) for Implant Supportedanterior Maxillary Restorations
The suggested CEI (Criteria for Esthetic Index) is summarised in Table 4. Index).

Table 4:CEI for an Anterior Maxillary Implant- supported restoration S, P and R Assessment Ratings and Evaluation Grades.
The soft tissue index (S), predictive index (P), and implant-supported restoration index (ISR) make up this aesthetic index (R). Specific criteria within each area were assessed and rated as adequate (rating 20%), compromised (rating 10%), or poor (rating 0%).
Soft tissue shape, colour and texture alterations, vertical deficiency, and mesial and distal papillae appearance are all characteristics of the S that have been previously identified. The P evaluated the proximal and horizontal contour inadequacy, gingival tissue biotype, implant apico-coronal location, and distal interproximal bone height are all factors to consider.
A periodontal probe was used to calculate from the dental implant’s centre to an imagined line drawn on the buccal bone flange surrounding teeth to determine the horizontal contour defect. Appropriate, compromised, and poor grades were determined as distances of 0, 1 to 3, and >3 mm, respectively.
The R looked at the Colour and translucency of implant supported restorations, surface roughness and ridges, implant/ crown incisal edge position, Table 1 shows, for each grade there is a variance in parameter ratings. Appropriate, compromised, or inadequate crown width/length ratios were determined as 0.85,0.85 to 1.0,>1.0.
Each of the indices’ components (S, P, and R) is portrayed separately to make the CEI more useful. As previously stated, each component comprised of five distinct characteristics that were classified as adequate (20%), compromised (10%), or poor (10%). (0 percent)(27).
Clinical Significance: When planning treatment, soft tissue biotypes should be considered because they have an impact on the final therapy outcome. The thickness and contour of the soft tissue are crucial diagnostic criteria that alter the cosmetic result of implant repair. The long-term stability of the implant and the gingival margin around the adjacent tooth depends on the proper facial bone height and thickness (Table 5)(28).

Table 5:Treatment for thick and thin gingival biotype
Biotype and Immediate Implant Placement: Wohrle first reported on the Immediate implantation and provisionalization technique in the aesthetic zone. It has since been used in a number of studies and has proven to have the ability of effective high-success/survival therapy rates and gingival health that is stable in structure. The width of the keratinized gingiva in the central buccal part of the socket should be at least 2 mm, and the biotype of the gingiva should be thick (more than 2 mm). To be able to maintain the stability in the primary implant, the apical bone behind the extraction socket must be at least 4 mm.
The tips among the interdental contact and the most coronal papillae should be the mesial and distal papillae. The gap between the extraction socket’s face bone and the implant should be at least 2 mm to keep the soft tissue profile of the implant for ideal aesthetics. The most difficult goal of implant treatment in the aesthetic field is to achieve Stability of soft and rigid tissues throughout time. Retraction of the mucosa in the central face is one among the most popular problems after a quick implantation.
The anatomical factors associated with the retraction of the central face after the gingival biotype and the keratinized mucosal width are two factors that influence rapid implantation. When implants were implanted in individuals with thin gingival biotypes and keratinized mucosa less than 2 mm broad, there was more recession. Despite simultaneous bone management, 8.3% of sockets with narrow V-shaped facial bone defects larger than 3 mm observed central facial recession after immediate implantation and provisionalization, larger than 1.5 mm after a year (29).
Limitations
Psychological factors: While helping to restore oral function and attractiveness, implant dentistry can occasionally fall short of exceedingly high patient expectations. It is critical to realise that not every patient receives a flawless treatment result from dental implants. It is occasionally possible to achieve equivalent or even better aesthetic outcomes by replacing anterior teeth with resin-bonded restorations or traditional fixed partial dentures. In order to avoid exaggerated expectations and misconceptions, proper patient-dentist communication and documentation are required (30,31).
Health vs. esthetics: The most successful objective of peri implant interference is to diminish and reduce morbidity, such as mucosal inflammation and peri-implantitis. While dental implants elevates a poor aesthetic outlook, which may hinder people and adversely affect sociability, lifestyle, and performance, this is not the main goal of these procedures (32,33). The health status surrounding teeth and dental implants is influenced by the interplay between prospective pathogens and the immunological reaction of the host. It is believed that local host-parasite interactions are influenced by the composition and design of dental implants. The aspects of layout of implant that influence the elevation of soft tissue and bone surrounding implants, meanwhile, are still not completely understood (34).
Interimplant anterior scalloped papilla: The alveolar bone crest serves as the basic guide for peri-implant mucosal height; nevertheless, the determinants of the development of interimplant papilla are complicated and cannot be entirely under the control of implant design characteristics or surgical treatments. Although in the morphology of tooth, contact point of the interdental area, and the quality and alignment of soft tissue fibres can all affect outlook of soft tissue, height and thickness of the bone. A significant barrier to the appearance and control of soft tissue around implants is the paucity of dento-gingivo alveolar circular, semi-circular, intergingival, transeptal, and interpapillary fibres. A key issue in dental implant aesthetics is the absence of interimplant papillae, which results in an interimplant black triangle (34).
Provisional phase: For optimum healing, the kind of temporary prosthesis utilised during the healing process is essential. The interim restoration’s design has to take into account comprehensive diagnostic data and aim to cause the soft tissues as little discomfort and pressure as possible after surgery (35). A suitable interim restoration can offer helpful recommendations regarding the aesthetic appeal (18)