Case Report | Volume 4 - Issue 1 | Article DOI :
Download PDF
Anders Bang-Nielsen*, Morten Westergaard Noack, Aske Mathias Bohm and Morten Laksáfoss Lauritsen
Department of Gastroenterology Surgery, Hvidovre Hospital, University of Copenhagen, Denmark
Corresponding Author:
Anders Bang-Nielsen, Department of Gastroenterology Surgery, Hvidovre Hospital, University of Copenhagen, KettegårdAlle 30, 2650 Hvidovre, Denmark, Tel: + 45 38625368; Email: Anders.Bang-Nielsen@regionh.dk
Keywords
Large bowel obstruction; Ileus; Pancreatic cancer
Abstract
Background: Despite the close anatomical relationship between the pancreatic tail and left colonic flexure, large bowel obstruction due to pancreatic cancer is a rare condition.
Case presentation: We present two cases of large bowel obstruction due to pancreatic cancer.
Conclusion: In case of large bowel obstruction due to pancreatic cancer, an aggressive approach should be considered due to the nature of invasive pancreatic cancer in these cases with a palliative aim
Introduction
Acute mechanical large bowel obstruction is a surgical emergency. The treatment is either stenting or surgery – depending on the nature of the obstruction, anatomic location, dissemination and patient comorbidity. In case of sigmoid volvulus, endoscopy is preferred [1,2].
Common causes of mechanical large bowel obstruction are:
• Malignant: primary colon tumor, recurrent colon tumor, metastatic disease or pelvic malignancies (e.g. ovarian cancer).
• Benign: crohns disease, diverticulitis, volvulus, adhesions, giant lipoma, acute pancreatitis, radiation therapy or fecal impaction [3]. • Colonic neoplasm is the dominating cause followed by volvulus and adhesions [4].
• Obstruction due to pancreatic cancer is exceedingly rare. Only four cases have previously been reported [5].
The anatomical relationship between the pancreatic tail and left colonic flexure, causes the colon to be susceptible to severe and expanding pancreatic disease, in worst cases, causing fistulas, ischemia, ulcers, stenosis [6] or as in this case series, obstruction of the colon due to adenocarcinoma in the pancreatic tail.
Case Presentation
Patient 1
48-years old male, presented with 2 days of diffuse abdominal pain, intermittent vomitus and dizziness. Last defecation and flatus less than 12 hours prior to admission. Known history of chronic pancreatitis, alcohol abuse and previous treatment with extracorporeal shock wave lithotripsy (ESWL) due to pancreatic duct stones. An abdominal computed tomography (CT) scan had revealed thickening of the colonic wall at the left flexure a year before.
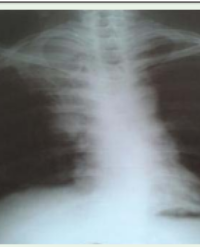
Clinically the abdomen was slightly distended, with direct pain to the epigastrium and left curvature. Furthermore no peritoneal reaction and normal bowl sounds was found. Blood samples where normal, except for a creatinin of 200 μmol/l(ref 60-105 μmol/l). Normal vital signs (blood pressure, pulse, respiratory frequency, temperature and Glasgow coma scalescore) were found. An abdominal ultrasound showed thickening of bowel segments, and gastric retention indicating a possible ileus. An abdominal CT scan was performed, showing large and small bowel ileus with a transition zone at the left colonic flexure with no suspicion of a tumor (Figure 1). An X-ray with retrograde colonic contrast only reached the left colonic flexure (Figure 2). The patient was clinically unaffected, and initial treatment was conservative.

Figure 1: Abdominal CT scan without contrast: Gastric retention, normally calibrated proximal small intestines and distal small intestines distended to 3,5cm with fluid. Ascending and transverse colon distended to 8 cm. Transition zone in the left colonic flexure. Left colon collaborated. No wall thickening of the colon is observed.

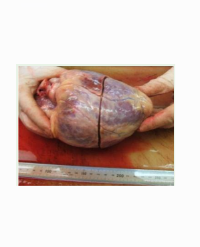
Figure 2: Colonic contrast pouring: Contrast reaching the left colonic flexure where the contrast stops and the colon is seen narrowing.
The next day a colonoscopy was performed, showing an obstruction at the left flexure. Stenting was attempted, but unsuccessful. The patient underwent an emergency explorative laparotomy, where a mass involving the left colonic flexure, the spleen and pancreatic tail, was found, reaching the greater curvature of the stomach, causing gross distension of the large bowel. Descending colon, distal transverse colon, spleen and pancreatic tail was resected enbloc, a transverse colonostomyand a sigmoid fistula were performed.
An intraoperative gastroscopy showed an intact stomach. During the procedure the diaphragm was breached leading to pneumothorax and a pleural drain was inserted. The patient initially recovered well, was treated with, metronidazole, piperacillin/tazobactam, and later anidulafungin due to fungal infection in the blood. On the 15th day after surgery, the patient´s condition worsened rapidly and he passed away on the 16th day after surgery. The histology of the resected specimen showed adenocarcinoma in all the resected organs with primary tumor location in the pancreatic tail.
Patient 2
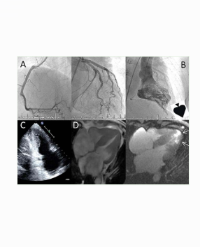
92-year old female presented with a history of progressively distended abdomen during one day. Last defecation the day before, no nausea or vomiting. She was known mitral valve prolapse and mitralin sufficiency, hypertension, hypercholesterolaemia and previous hysterectomy and oophrectomy. Clinically the patient´s abdomen was distended with diffuse pain and dampened bowel sounds. Blood samples were normal. A CT scan showed large bowel obstruction, with a suspected stenosis at the left colonic flexure, with suspicion of a malignant colon tumor T3 N0 M0. The CT scan showed mild degree of ascites, left sided pleural exudate and a small ventral hernia (Figure 3).

Figure 3: Participant observation during regular training with LY and the centre staff.
A colonoscopy was planned with the intention of placing a selfexpanding metal stent (SEMS). The patient’s condition worsened before the procedure, and an emergency laparotomy, was performed. Total colectomy, distal pancreas resection and splenectomi were performed, and a suction drain placed. The day after the procedure the patient became hemodynamically unstable, with bleeding in the drain, and underwent an explorative laparotomy. Bleeding from a small gonadal vessel was identified A colonoscopy was planned with the intention of placing a selfexpanding metal stent (SEMS). The patient’s condition worsened before the procedure, and an emergency laparotomy, was performed. Total colectomy, distal pancreas resection and splenectomi were performed, and a suction drain placed. The day after the procedure the patient became hemodynamically unstable, with bleeding in the drain, and underwent an explorative laparotomy. Bleeding from a small gonadal vessel was identified
Discussion
Patients presenting with pancreatic cancer usually complain of jaundice, abdominal pain and/or loss of appetite/weight loss [7]. Bowel obstruction in these patients is most likely due to carcinosis in the small bowel. Initial workup should include contrast enhanced abdominal CT, to evaluate possible advanced disease, and early fluid resuscitation despite, normal blood samples and vitals. Chronic pancreatitis is on rare occasions known to cause stenosis of the left colonic flexure [6]. In these cases surgery should be considered [8].
We have presented two cases where large bowel obstruction, initially suspected of colonic cancer and chronic pancreatitis, was due to pancreatic cancer. The patients must be treated for the large bowel obstruction primarily, either by stenting, resection and/or anastomotic bypass as possible choices of treatment. In these cases the cancer is advanced with a short expected lifespan, and procedures should be performed with a palliative aim.
Since the oncological treatment is different for colonic and pancreatic cancer, it is important to obtain biopsies, if a SEMS is placed and no resection is done. In case of large bowel obstruction, due to pancreatic cancer invading the colon, a more aggressive approach is recommended, although the procedure has a palliative aim.
Conclusion
The six patients in the published cases with large bowel obstruction, due to pancreatic tail cancer, passed away within months, hereby highlighting the palliative aim of treatment and care.
Acknowledgement
Author contribution: A Bang-Nielsen is lead author and drafted the manuscript. MW Noack, AM Bohm and ML Lauritsen and A Bang-Nielsen designed the study, did picture editing and edited the article. All authors have approved the article.
Informed consent statement: All involved persons have given their informed consent for obtaining medical records and to be included in this case report. Institutional review board statement: The study was reviewed and approved by the Department on Gastrointestinal surgery Institutional Review Board.
References
1. Pujahari AK. Decision Making in Bowel Obstruction: A Review. J Clin Diagn Res. 2016; 10: 7-12.
2. McCullough JA, Engledow AH. Treatment options in obstructed left-sided colonic cancer. Clin Oncol. 2010; 22: 764-770.
3. Baron TH. Acute colonic obstruction. Gastrointest Endoscopy Clin N Am. 2007; 17: 323-339.
4. Yeo HL, Lee SW. Colorectal Emergencies: Review and Controversies in the Management of Large Bowel Obstruction. J Gastrointest Surg. 2013; 17: 2007-2012.
5. Griffin R, Villas B, Davis C, Awad ZT. Carcinoma of the Tail of the Pancreas Presenting As Acute Abdomen. JOP. 2012; 13: 58-60.
6. Gardner A, Gardner G, Feller E. Severe Colonic Complications of Pancreatic Disease. J Clin Gastroenterol. 2003; 37: 258-262.
7. Forrest JF, Longmire WJP Jr. Carcinoma of the pancreas and periampullary region. Ann Surg. 1979; 189: 129-138.
8. Van Minnen LP, Besselink MGH, Bosscha K, Vang Leeuwen MS, Scipper ME, Gooszen HG. Colo.
Citation
Bang-Nielsen A, Noack MW, Bohm AM and Lauritsen ML. Large Bowel Obstruction due to Pancreatic Cancer - A Case Series. SM J Clin Med. 2018; 4(1): 1033.