Case Report | Volume 4 - Issue 1 | Article DOI :
Download PDF
Negar Moheb¹˒³, Shaweta Khosa³, Bhavesh Trikamji⁴ and Shri K Mishra¹˒²˒³
¹Department of Neurology, David Geffen School of Medicine at UCLA, USA
²Department of Neurology, Keck School of Medicine at University of Southern California, USA
³Department of Neurology, Olive View UCLA Medical Center, Sylmar, USA
?Department of Neurology, Harbor UCLA Medical Center, Torrance, USA
Corresponding Author:
Shri K Mishra, Department of Neurology, University of Southern California, Keck School of Medicine, USA, Tel: 322- 409-7381; +1 323 409 8686; Fax: 323 226-5869; Email: smishra@usc.edu
Keywords
Rubinstein-Taybi Syndrome; Cervical Spinal Stenosis; Spasticity; Myelopathy
Abstract
Rubinstein-Taybi Syndrome (RTS) is a rare autosomal dominant genetic disease characterized by growth deficiency, broad thumbs and great toes, intellectual disability and characteristic craniofacial appearance. Neurological manifestations of RTS include: seizures, primary brain tumors, cranio-spinal and posterior fossa anomalies. We describe a 21 year-old male with past medical history of congenital heart disease, kypho-scoliosis, intellectual disability, and global developmental delay. Neurological examination revealed spasticity with atrophic changes in all the extremities. Brain MRI was unremarkable and spinal MRI revealed multi-level degenerative changes in cervical spine with cervical spinal stenosis for which patient underwent C4-C6 laminectomy with postero-lateral fusion. In spite of de-compressive surgery, the spasticity persisted making RTS as the most likely etiology of spasticity. Patient spasticity was managed with baclofen and tizanidine. The goal of this case report is to extend our current knowledge on RTS and to define new international guidelines for diagnosis, care and treatment.
Introduction
Rubinstein-Taybi syndrome (RTS) or Broad thumb-hallux syndrome is an extremely rare congenital disorder characterized by short stature, intellectual disability, distinctive facial features, broad thumbs and first toes base, congenital cardiac abnormalities and skeletal anomalies. Although patients frequently present with cardiorespiratory, musculoskeletal, genitourinary and endocrine abnormalities, neurological manifestations are not rare. The most common neurological manifestations of RTS include: seizures, primary brain tumors, cranio-spinal and posterior fossa anomalies [1]. The estimated prevalence of RTS is one case per 125,000 live births [2]. Associations between compressed spinal cord due to fusion of vertebrae and RTS has been reported before and it was suggested that laminectomy and spinal cord untethering procedures can benefit most of the patients [3,4]. Myelopathy is the clinical manifestation of spinal cord compression causing upper motor neuron neurologic dysfunction such as gait disturbance, increased reflexes, spasticity, muscle weakness and/or numbness.
Case Report
We report a 21 years old male patient who presented to the neuromuscular clinic with spasticity in bilateral upper extremities. He was diagnosed with Rubinstein-Taybi syndrome at the age of 15 based on clinical features. A diagnosis of RTS was later con-firmed on genetic testing.
He had a past surgical history of congenital cervical stenosis with myelopathy for which he underwent C4-C6 laminectomy and posteriolateral fusion, scoliosis, kyphosis, repaired congenital heart defects (ASD, Pulmonary stenosis and PDA), intellectual disability and global developmental delay. Patient’s mother is the informant and she takes care of his Activities of Daily Living (ADLs). Patient is wheelchair bound and communicates by nodding his head for yes or no. His current medications include Baclofen 10 mg BID and Tizanidine 2mg BID, for severe spasticity.
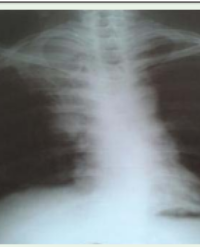
Neurological examination was significant for atrophic changes in bilateral upper and lower extremities. Patient had increased tone with spasticity in bilateral upper extremities, more on the left compared to the right. Right elbow demonstrated full range of motion while left elbow revealed contractures at 145 degrees. Patient had a Brain MRI in 2011, which was unremarkable.
Thoracolumbar MRI in 2013 revealed worsening of thoracic scoliosis compared to the previous study. There was a nonspecific focal hyper-intense T2 signal in the Conus medullaris of cervical spine. Multilevel degenerative changes of cervical spine with post surgical changes from C4 through C6 including cervical cord volume loss and abnormal signal change were noted.
Discussion
Rubinstein-Taybi Syndrome (RTS) is a rare autosomal dominant genetic disorder. Rubenstein and Taybi first reported this in 1963 on seven cases which included a group of anomalies such as short, broad thumbs and great toes, facial abnormalities, psychomotor retardation, highly arched palates and history of recurrent respiratory infections [5]. It is associated with congenital anomalies of cardiovascular system such as ventricular septal defect, patent ductus arteriosus, coarctation and stenosis of the aorta and pulmonic stenosis [6]. It is characterized by mutations in the CREB-binding protein (CREBBP) gene and it has been suggested that a micro-deletion in chromosome segment 16p13.3 could be the cause [7,8]. Alterations in the E1Abinding protein p300 (EP300) can also cause this disorder [9,10] Cervical vertebral abnormalities as C1-C2 instability, osodontoideum, hypoplasia of the dens and fusion of the cervical vertebrae has been reported, with possible stenosis at the craniovertebral junction, which may cause cervical myelopathy [11]. Tanaka et al suggested that some underlying conditions of RTS may mask the symptoms of a tethered spinal cord and careful attention to the symptoms is necessary to prevent further neurological problems [4]. We describe a patient with known/confirmed diagnosis of RTS who presented with spasticity in bilateral upper extremities. It is hard to predict the exact etiology of spasticity but based on the fact that cervical cord stenosis was fixed with laminectomy and postero-lateral fusion, RTS remains the only possible cause of patient’s symptoms. We report an interesting finding in this patient, which is probably a sequel to this devastating disease. Early recognition and treatment can help improve the quality of life in most of these patients.
Conclusion
RTS is an extremely rare condition for which although some clinical aspects have been clearly identified, a lot of multicenter studies are needed to expand our current knowledge on the clinical phenotype. Cervical vertebrae anomalies are common manifestations of RTS. Although laminectomy and reducing spinal cord compression can lead to improvement in most patients, some patients will still experience myelopathy symptoms and special attention should be paid to prevent further neurological consequences. We report an interesting case of RTS with spasticity in all the extremities. The ultimate goal of this case report is to extend our current knowledge on RTS and to define new international guidelines for diagnosis, care and treatment of patients with RTS. Early intervention, special education, vocational training to address developmental disabilities is critical in the management of this rare disorder.
References
1. Giacobbe A, Ajmone PF, Milani D, Avignone S, Triulzi F, Gervasini C, et al. Electroclinical phenotype in Rubinstein-Taybi syndrome. Brain Dev. 2016; 38: 563-570.
2. Milani D, Manzoni F, Pezzani L, Ajmone P, Gervasini C, Menni F, et al. Rubinstein-Taybi syndrome: clinical features, genetic basis, diagnosis and management. Ital J Pediatr. 2015; 41: 4.
3. Yamamoto T, Kurosawa K, Masuno M, Okuzumi S, Kondo S, Miyama S et al. Congenital anomaly of cervical vertebrae is a major complication of Rubinstein-Taybi syndrome. Am J Med Genet A. 2005; 35A: 130-133.
4. Tanaka T, Ling BC, Rubinstein JH, Crone KR. Rubinstein-Taybi syndrome in children with tethered spinal cord. J Neurosurg Pediatr. 2006; 105: 261-264.
5. Rubinstein JH, Taybi H. Broad thumbs and toes and facial abnormalities. A possible mental retardation syndrome. Am J Dis Child. 1963; 105: 588-608.
6. Stevens CA, Bhakta MG. Cardiac abnormalities in the Rubinstein-Taybi syndrome. Am J Med Genet. 1995; 59: 346-348.
7. Petrij F, Giles RH, Dauwerse HG, Saris JJ, Hennekam RC, Masuno M et al. Rubinstein-Taybi syndrome caused by mutations in the transcriptional coactivator CBP. Nature. 1995; 376: 348-351.
8. Lee CG, Cho E, Ahn YM. Maternally inherited autosomal dominant intellectual disability caused by 16p13.3 microduplication. Eur J Med Genet. 2016; 59: 210-214.
9. Roelfsema JH, White SJ, Ariyürek Y, Bartholdi D, Niedrist D, Papadia F, et al. Genetic heterogeneity in Rubinstein-Taybi syndrome: mutations in both the CBP and EP300 genes cause disease. Am J Hum Genet. 2005; 76: 572-580.
10. Wincent J, Luthman A, van Belzen M, van der Lans C, Albert J, Nordgren A et al. CREBBP and EP300 mutational spectrum and clinical presentations in a cohort of Swedish patients with Rubinstein-Taybi syndrome. Mol Genet Genomic Med. 2016; 4: 39-45.
11. Robson MJ, Brown LM, Sharrard WJ. Cervical spondylolisthesis and other skeletal abnormalities in Rubinstein-Taybi syndrome. J Bone Joint Surg Br. 1980; 62: 297.299.
Citation
Moheb N, Khosa S, Trikamji B and Mishra SK. Neurological Manifestations of Rubinstein-Taybi syndrome: A Case Report. SM J Clin Med. 2018; 4(1): 1032s1