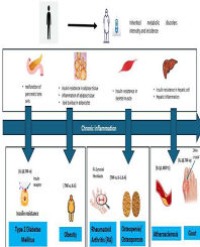
Metabolic Vulnerability and Immune Challenge: Interactions between Inherited Disorders, Metabolic Syndrome, and Infection Risk
Inherited Metabolic Diseases (IMDs) are rare genetic disorders with an enzyme and/or transport system dysfunction of a metabolic pathway. Infections frequently induce Acute Metabolic Decompensation (AMD) in patient with IMDs, and may also compromise the outcome of disorders not primarily recognized as crisis prone. On the other hand, immunocompromise resulting from metabolic defects can render the host more vulnerable to recurrent or severe infections. Metabolic syndrome (MetS) is a cluster of metabolic symptoms, including visceral obesity, insulin resistance, glucose intolerance, dyslipidemia, and hypertension that are interlinked to cause increased population risk of chronic disease and impaired immune defences. The worldwide prevalence of obesity, a main contributor for MetS, nearly tripled between 1975 and 2018 and over half of all adults are predicted to be obese by 2050. In addition to NCDs, MetS modulates host-pathogen interactions, rendering the host more susceptible to severe viral infections including flu and coronaviruses. Here, we review recent findings that challenge this dogma and demonstrate a new concept in the regulation of host defense: early metabolic reprogramming of both immune and nonimmune cells powerfully determines infection outcome, severity of disease, and long term health. This review discusses the relationships between IMDs and infections in a bidirectional manner examining mechanisms, impact of diet, immune metabolic disturbances, and novel treatments.
Sharifull Islam1,2*

