Case Report | Volume 3 - Issue 6 | Article DOI :
Download PDF
Charles DeCarlo¹, John Phair², Katie Weichman³, Evan Lipsitz², and Karan Garg²*
¹Department of Vascular and Endovascular Surgery, Massachusetts General Hospital, USA
²Department of Cardiovascular and Thoracic Surgery, Montefiore Medical Center, USA
³Department of Plastic and Reconstructive Surgery, Montefiore Medical Center, USA
Corresponding Author:
Karan Garg, Department of Cardiovascular and Thoracic Surgery, Montefiore Medical Center, 3400 Bainbridge Ave, Bronx, NY 10467, USA, Tel: 718-920-8584; Email: kgarg@montefiore.org
Keywords
Hypothenar hammer syndrome; Ulnar artery aneurysm; Aneurysm; Hand surgery; Vascular surgery
Abstract
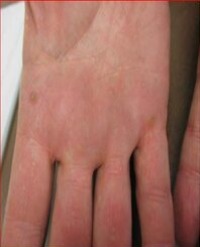
Objectives: Hypothenar hammer syndrome is a rare clinical entity, typically presenting unilaterally, in middle-aged men, with a history of persistent trauma to their hypothenar eminence. We report a case of bilateral hypothenar hammer syndrome in a 77-year-old man with no recent occupational exposure.
Methods: We performed an extensive literature search using the Pubmed database and identified less than 175 results on hypothenar hammer syndrome. Only 12 articles referenced bilateral hypothenar hammer syndrome. Additionally, only 16 articles included patients 65 and older. The following search terms were used: hypothenar hammer syndrome, bilateral, “two aneurysms,” “multiple aneurysms,” and symptoms.
Results: A 77-year-old man who presented with pulsatile hypothenar masses bilaterally and was diagnosed with hypothenar hammer syndrome. He worked as a carpenter 15 years before presentation. He currently uses a rolling walker. CT angiography confirmed the presence of two aneurysms in his dominant right hand, the largest measuring 1.8 cm in diameter. The patient had a motor function deficit along the distribution of the ulnar nerve on the right hand. He underwent resection of the aneurysms in the right hand and reconstruction of the ulnar artery.
Conclusion: Unusual aspects of this case include age of presentation, bilateral aneurysms, and lack of recent occupational exposure. We assert that the use of a rolling walker may have contributed to the progressive aneurysmal degeneration of his ulnar artery.
Citation
DeCarlo C, Phair J, Weichman K, Lipsitz E and Garg K. An Unusual Presentation of Hypothenar Hammer Syndrome. SM J Case Rep. 2017; 3(6): 1064.