Case Report | Volume 3 - Issue 3 | Article DOI :
Download PDF
Adigun TA* and Sotunmbi PT
Department of Anaesthesia, University College Hospital, Nigeria
Corresponding Author:
Tinuola Abiodun Adigun, Department of Anaesthesia, College of Medicine, University of Ibadan and University College Hospital Ibadan, Nigeria, Tel: 2349025058328; Email: tonitomi2005@ yahoo.co.uk
Keywords
TURP; Low Ejection fraction; Combined spinal epidural anaesthesia
Abstract
Background: Anaesthetic management of patients with low ejection fraction secondary to dilated cardiomyopathy is a challenge to the anaesthetists as these patients are at increased risk of congestive cardiac failure, arrhythmias and sudden death.
Objective: To report a case of a 66 year old man with low ejection fraction secondary to dilated cardiomyopathy scheduled for Transurethral Resection of the Prostate Gland (TURP).
Method: Combined low dose spinal (2 ml of 0.5% of heavy Bupivacaine) and epidural anaesthesia was used in this patient to avoid drug induced myocardial depression of general anaesthesia. Patient had a bout of hypotension which was treated with 3mg of Ephedrine otherwise intraoperative and postoperative period were uneventful.
Conclusion: Anaesthesia for a patient with low ejection fraction secondary to dilated ardiomyopathy required that the patient should have a meticulous perioperative management to achieve a good outcome.
Introduction
Most patients scheduled for Transurethral Resection of the Prostate Gland (TURP) are elderly and are usually present with cardiovascular, endocrine, renal, cerebral or respiratory diseases thereby increasing their risk for surgery and anaesthesia. Patients presenting with low ejection fraction secondary to Dilated Cardiomyopathy (DCM) present a challenge to the anaesthetist. They have poor prognosis and are at increased risk of congestive cardiac failure, arrhythmias and sudden death [1].
Ejection Fraction (EF) is an important measurement in determining how well the heart is pumping out blood, in diagnosing, as well as tracking heart failure. The normal EF is between 55% and 70% and EF of 40% to 55% indicates damage from previous heart disease [2].
EF 117% excluding any known cause of myocardial disease1. Familiar dilated cardiomyopathy accounts for 20-48% of all DCM1. Patients with low EF may present at any time for anaesthesia. It is essential that the anaesthetist understands the underlying pathology to better manage these patients. We present a case with low ejection fraction of 42% secondary to DCM who underwent TURP under combined low dose spinal epidural anaesthesia.
Case Report
A 66 year old man with symptomatic benign prostate hypertrophy was scheduled for TURP. The patient was a known case of dilated cardiomyopathy for 3 years and the cause of the cardiomyopathy could not be established by the cardiologist. He had a history of orthopnea and exertional dyspnea. No history of alcohol intake or smoking. He was not a known hypertensive, diabetic or asthmatic patient. He had a previous history of cataract extraction under local anaesthesia prior to presentation to the urologist, surgery and anaesthesia were uneventful.
No known drug allergy. His symptom was well controlled on Moduretic one tablet daily and Digoxin 0.125 mg daily. On pre-anaesthetic examination he was not pale, anicteric, acyanosed, no pedal oedema. Cardiovascular examination revealed a pulse rate of 67 beats per minute, blood pressure of 110/70mmHg, Jugular Venous Pressure (JVP) was not raised, heart sounds 1 and 2 were heard no murmur. Respiratory rate was 16 per minute, vesicular breath sounds heard without any added sounds. There were no signs of heart failure like raised JVP, ankle oedema or hepatomegally.
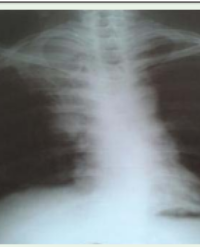
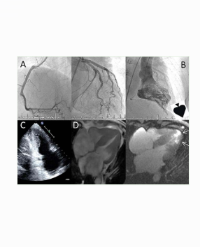
His investigations were as follows; packed cell volume 48%, electrolytes; sodium 140meq/L, potassium 3.8 meq/L, chloride 107 mg/dl, creatinine 106 mg/dl and urea 10mg/dl. Chest radiograph revealed cardiomegally with no signs of pulmonary congestion. Pre operative 12 lead electrocardiographs showed left bundle branch block. Echocardiograph showed global hypokinesia of the left ventricle, poor systolic function, dilated cardiac chambers with bilateral ventricular dysfunction, mild tricuspid regurgitation, no intracardiac clot and ejection fraction was 42%. The international normalizing ratio was 1.0. Patient was classified as American Society of Anaesthesiologist classification physical status of 3.
High risk informed consent and written consent was obtained in view of the cardiac disease and poor ejection fraction. We decided to go with regional anaesthesia (combined spinal epidural anaesthesia) technique reason for the selection was explained to the patient. Patient continued with his cardiac medication and diazepam 5mg a night before and on the morning of surgery.
On arrival in the operating room, peripheral venous cannulation was established with 18 G Intravenous cannula and 0.9% Normal saline infusion was administered at 250ml per hour. Non invasive blood pressure, pulse oximeter and electrocardiograph were attached for continuous monitoring. Base line vital signs were pulse 72/ minute, blood pressure 120 /80 mmHg, oxygen saturation was 99%. Emergency drugs like adrenaline, inotropes and amiodarone were kept ready.
In the sitting position, epidural needle was inserted at L1/2 under aseptic technique and epidural catheter was inserted after a test dose of 3 ml of lidocaine with adrenaline to eliminate intravascular or intrathecal injection. Spinal anaesthesia was instituted at L3/4 space and 2ml of 0.5% of heavy Bupivacaine was injected into the subarachnoid space after a free flow of cerebrospinal fluid. The sensory level was up to T10.
Oxygen was given via nasal prong at the rate of 2l/minute. After 10 minutes of spinal anaesthesia, the blood pressure dropped to 90/50 mmHg, intravenous ephedrine 3 mg was given and the blood pressure increased to 110/65mmHg. There was no episode of arrhythmia. Total fluid infused was one litre of 0.9% normal saline and surgery lasted one hour. Throughout the surgery the patient was pain free, conscious and comfortable.
At the end of the surgery patient was transferred to the high dependency unit postoperative vital signs were pulse 95 /minute, blood pressure115/ 80mmHg , and oxygen saturation 100% in room air. After 2 hours of surgery a bolus of 5 ml of plain Bupivacaine of 0.125% was given by epidural catheter and the catheter was removed 12 hours postoperatively. Postoperative period was uneventful.
Discussion
Increasing aging of the population leads to high prevalence of comorbidities including heart failure in the elderly. Normal ejection fraction is between 55%-70% and EF of 40% to 55% indicates damage from previous heart disease [2]. EF <35% is considered to be an optimal predictor of postoperative cardiac event [3]. However, patients having low ejection fraction secondary to dilated cardiomyopathy are prone to increased risk of congestive cardiac failure and sudden death from ventricular arrhythmias [1].
Preoperative preparation is an important part of the management in this patient; it must be meticulous as the patient has minimal cardiac reserve. The patient was managed medically in conjunction with the cardiologist for proper optimization [3].
Our patient was placed on digoxin, an inotrope to improve his cardiac contractility and cardiac output before surgery. He was on diuretic because of dyspnea and orthopnea. He was not on any antiarrythmitic drugs. Preoperative electrolytes should be measured and corrected preoperatively as a decrease in potassium can lead to arrhythmias as patient on diuretic has a risk factor for low potassium although our patients’ electrolytes were normal.
Packed cell volume should be maintained above 30% in elective cases to increase the oxygen carrying capacity of the blood. The anaesthetic management goals in patients with cardiomyopathy and low EF include avoidance of drug - induced myocardial depression, maintenance of normovolemia, avoidance of fluid overload, avoidance of sudden hypotension, prevention of increased ventricular afterload and maintenance of stable condition in the postoperative period [6].
With these factors in mind we opted for combined low dose Spinal Epidural Anaesthesia (CSEA) as opposed to general anaesthesia. Regional anaesthesia has advantage of attenuating the neurohumoral stress response to surgery, produces vasodilatation thereby reducing after load, reducing the incidence of thromboembolic phenomenon, avoid polypharmacy and enhance early ambulation [7].
Early recognition of cardiac, cerebral changes and TURP syndrome were other benefits of regional anaesthesia during a TURP. General anaesthesia is not desirable in this patient due to myocardial depressant effect of intravenous and inhalational anaesthestic agents and the stress of larngoscopy [6]. The TURP in this patient was performed under CSEA, spinal anaesthesia is the anaesthetic technique of choice for TURP in our centre and is usually enough for the procedure, however, patient with low ejection fraction may not tolerate high dose of bupivacaine hence low dose spinal block and extension with epidural catheter may be reasonable in the management of this patient.
Patients with low ejection fraction undergoing caesarean section and TURP have previously been done successfully under CSEA [8-10]. Indira et al. in a case report employed CSEA during caesarean section in a patient with ejection fraction less than 25%, similarly Osinaike and Ogar in our institution used CSEA in a patient with peripartum dilated cardiomyopathy with ejection fraction of 39% scheduled for caesarean section also CSEA was used also in a patient for transurethral resection of prostrate [8,9]. CSEA has the advantages of both spinal and epidural anesthesia.
Spinal anaesthesia component offers the rapid onset and reliability of spinal block with low drug dosage and the duration of anaesthesia can be extended with epidural catheter [8,9]. Epidural catheter is also used to provide the postoperative pain relief. Low-dose local anaesthetic is commonly administered to limit the level of block in order to minimize the haemodynamic changes [7,10].
However, CSEA has its disadvantages, including that higher level of neuronal blockade causing rapid precipitous reduction in the systolic blood pressure resulting in severe reduction in venous return and cardiac output [11]. However, this can be countered by administering vasopressors with mixed alpha and beta adrenergic properties e.g. ephedrine [11].
Fluid management is an important part in this management of this patient. To reduce fluid overload, one litre of normal saline was given throughout the period of the surgery to decrease the risk of congestive cardiac failure. Patient had a bout of hypotension following sympathetic blockade, this was corrected with ephedrine rather than fluid.
Monitoring is an important part of management in this patient, several authors have used invasive monitoring to manage more symptomatic cases [12], others have used non –invasive monitoring technique for asymptomatic and haemodynamically stable patients [8,9]. Elective use of invasive monitoring (arterial and central venous) is justified in symptomatic patient with an elevated JVP, third and fourth heart sound and clinical evidence of low cardiac output or echocardiographic evidence of significant myocardial depression [12].
Although this patient had low ejection fraction and dilated cardiomyopathy, he did not have any form of invasive monitoring such as invasive blood pressure, central venous pressure, cardiac output monitoring and myocardial performance by trans-oesophageal echocardiography during the anaesthesia due to high cost in a low resource centre like Nigeria but non - invasive blood pressure monitoring was at frequent intervals (2 minutes) with continuous ECG and pulse oximetry were used successfully in the management of this patient. Supplemental oxygen was administered to ensure that the oxygen saturation remained between 98%-100%.
Conclusion
Combined spinal low dose and epidural anaesthesia is a safe and feasible technique of anesthesia in low ejection fraction undergoing TURP.
References
1. Thiagarajah PH, Thiagarajah S, and Frost EA. Anesthetic considerations in patients with cardiomyopathies-a review. Middle East J Anaesthesiol. 2009; 20: 347-354.
2. Heart Failure Society of America, Lindenfeld J, Albert NM, Boehmer JP, Collins SP, Ezekowitz JA, et al. HFCA 2010 Comprehensive heart failure practice guideline. J Card Fail. 2010; 16: 1-194.
3. Poldermans D, Bax JJ, Boersma E, De Hert S, Eeckhout E, Fowkes G, et al. Guidelines for pre-operative cardiac risk assessment and perioperative cardiac management in non-cardiac surgery. Eur Heart J. 2009; 30: 2769- 2812.
4. Rigolli M and Whalley GA. Heart failure with preserved ejection fraction. J Geriatr Cardiol. 2013; 10: 369-376.
5. Sanderson JE. Heart failure with a normal ejection fraction. Heart. 2007; 93: 155-158.
6. Shrestha BR, Thepa C. Peripartum cardiomyopathy undergoing ceasarean section under epidural anaesthesia. Kathmandu University Medical Journal. 2006; 4: 503-505.
7. Gupta K, Gupta S, Jose S, Balachander H. Low dose spinal anesthesia for peripartum cardiomyopathy. J Anaesthesiol Clin Pharmacol. 2011; 27: 567- 568.
8. Indira K, Sanjeev K, Sunanda G. Sequential combined spinal epidural anesthesia for caesarean section in Peripartum cardiomyopathy. Indian J Anaesth. 2007; 51: 137-139.
9. Osinaike B, Ogar J. Anaesthesia for Caesarean section in a patient with pericardium cardiomyopathy. Cardiovascular Journal of Africa. 2011; 22: 152-154.
10. Kim SY, Cho JE, Hong JY, Koo BN, Kim JM, Kil HK. Comparison of intrathecal fentanyl and sufentanil in low dose dilute bupivacaine spinal anaesthesia for transurethral prostatectomy. Br J Anaesth. 2009; 103: 750-754.
11. Sanatkar M, Sadeghi M, Esmaeili N, Sadrossadat H, Shoroughi M, Ghazizadeh S, et al. The hemodynamic effects of spinal block with low dose of bupivacaine and sufentanil in patients with low myocardial ejection fraction. Acta Medica Iranica. Acta Med Iran. 2013; 51: 438-443.
12. Sharrock NE, Bading B, Mineo R, Blumen JD. Deliberate hypotensive epiduraepidural anaesthesia for patients with normal and low cardiac output. Anesth Analg. 1994: 79: 899-904.
Citation
Adigun TA and Sotunmbi PT. Combined Spinal Epidural Anaesthesia for TURP in a Nigerian Geriatric Patient with Low Ejection Fraction- Case Report. SM J Clin Med. 2017; 3(3): 1027.