Ioannis Siasios1,4*, Aggeliki Fotiadou1 , Aspasia Tsezou2 , Charalambos Gatos1 , Dimitrios Papadopoulos3 , Vassilios Dimopoulos4 and Konstantinos Fountas1
1Department of Neurosurgery, University Hospital of Larisa, Greece
2Department of Cytogenetics and Molecular Genetics, University Hospital of Larissa, Greece
3Intensive Care Unit, General Hospital of Larisa, Greece
4Department of Neurosurgery, University at Buffalo, USA
Corresponding Author:
Ioannis Siasios, Jacobs School of
Medicine and Biomedical Sciences,
State University of New York, University
at Buffalo Neurosurgery, 100 High Street,
Suite B4 Buffalo NY 14209, New York,
USA, Tel: 716-218-1000;
Fax: 716-218-1010;
Keywords
Decompressive craniectomy;
ICU; Malignant infarct; MCA;
Prothrombotic genes
Abstract
Background: Cerebral infarction is a potentially fatal pathological entity, which has been associated with numerous risk factors, such as family history of stroke, hypertension, dyslipidemia, diabetes mellitus, smoking and trauma. On the contrary, the role of prothrombotic gene polymorphisms as risk factors of stroke has not been yet fully established.
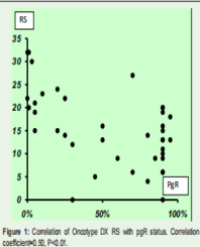
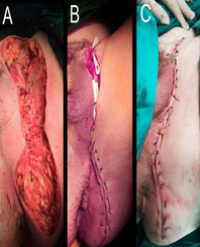
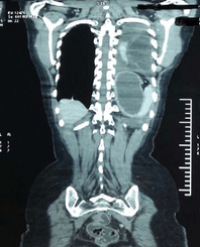
Case presentation: A 24-year old man with a thrombophilic profile sustained a left sided Middle Cerebral Artery (MCA) infarction. He was intubated due to his rapid clinical aggravation and underwent initially a left sided hemicraniectomy and soon after that a right sided hemicraniectomy without any significant response. He died due to severe sepsis in the ICU (Intensive Care Unit) the eleventh day after his admission. The laboratory exams showed that he was homozygote for the point mutation A1298C of the methylenetetrahydrofolate reductase (MTHFR) gene, and heterozygote for the 4G/5G polymorphism of the Plasminogen Activator Inhibitor-1 (PAI-1) gene.
Conclusions: Both mutations may have an association with the development of a stroke. Thus genetic testing could possibly assist physicians in prognosis and treatment strategizing of patients with stroke.
Citation
Siasios I, Fotiadou A, Tsezou A, Gatos C, Papadopoulos D, Dimopoulos V, et al. A deadly combination of the point mutation A1298C in the MTHFR gene, and the 4G/5G polymorphism in the PAI-1 gene of ayoung patient with a left MCA infarct. A case presentation and review of the literature. SM J Surg. 2017; 3(2): 1016.