Research Article | Volume 2 - Issue 1 | Article DOI :
Download PDF
Ather Pasha and Rindha Venepally*
Department of General medicine, Deccan College of Medical Sciences, India
Corresponding Author:
Rindha Venepally, MD general medicine,
Deccan College of Medical Sciences,
Hyderabad, Telangana, India,
Tel: 040 2480 2786;
Keywords
Type 2 Diabetes Mellitus; Complications of Type 2 Diabetes Mellitus;
Cardiovascular complications;
Cardiovascular diseases
Abstract
Type 2 Diabetes Mellitus is a medical condition characterized by an elevation of blood glucose level, this metabolic disorder will taken place as a result of either insulin resistance and/or insulin deficiency. It is the most prevalent chronic metabolic disorder worldwide. Type 2 Diabetes Mellitus is the significant cause of premature morbidity and mortality imposing enormous socioeconomic burden globally. As per the current prevalence and trend of T2DM, International Diabetes Federation (IDF) predicted 592 million people will have T2DM by 2035 worldwide. Prevalence of T2DM is escalating at rapid pace in India due to westernization of lifestyle. As per IDF report, the prevalence of T2DM will increase to 101.2 million by 2030 among Indians. Type 2 diabetes mellitus is typically a chronic disease associated with a ten-year-shorter life expectancy. This is partly due to a number of complications with which it is associated, including two to four times the risk of cardiovascular disease, including ischemic heart disease and stroke; a 20-fold increase in lower limb amputations, and increased rates of hospitalizations. In the developed world, and increasingly elsewhere, type 2 diabetes mellitus is the largest cause of non-traumatic blindness and kidney failure. It has also been associated with an increased risk of cognitive dysfunction and dementia through disease processes such as Alzheimer’s disease and vascular dementia. The contemporary associations of type 2 diabetes mellitus with a wide range of incident cardiovascular diseases have been compared in this study. Results showed that Type 2 diabetes mellitus was positively associated with peripheral arterial disease, ischaemic stroke, heart failure, and non-fatal myocardial infarction, but was inversely associated with abdominal aortic aneurysm and subarachnoid haemorrhage, and not associated with arrhythmia or sudden cardiac death. Type 2 DM is a metabolic disease that can be prevented through lifestyle modification, diet control, and control of overweight and obesity. Novel drugs are being developed, yet no cure is available in sight for the disease, despite new insight into the pathophysiology of the disease. Management should be tailored to improve the quality of life of individuals with type 2 DM.
Citation
Pasha A and Venepally R. Incidence of Cardiovascular Diseases in Type 2 Diabetes Mellitus Patients. J Gen Med. 2018; 2(1): 1007.
Introduction
Type 2 diabetes mellitus (also known as type 2 diabetes) is a long-term metabolic disorder that is characterized by high blood sugar, insulin resistance, and relative lack of insulin. The classic symptoms of diabetes are polyuria (frequent urination), polydipsia (increased thirst), polyphagia (increased hunger), and weight loss. Other symptoms that are commonly present at diagnosis include a history of blurred vision, itchiness, peripheral neuropathy, recurrent vaginal infections, and fatigue. The development of type 2 diabetes is caused by a combination of lifestyle and genetic factors. While some of these factors are under personal control, such as diet and obesity, other factors are not, such as increasing age, female gender, and genetics. The World Health Organization definition of diabetes (both type 1 and type 2) is for a single raised glucose reading with symptoms, otherwise raised values on two occasions, of either fasting plasma glucose ≥ 7.0 mmol/l (126 mg/dl) or with a glucose tolerance test, two hours after the oral dose a plasma glucose ≥ 11.1 mmol/l (200 mg/dl) [1,2]. Management of type 2 diabetes focuses on lifestyle interventions, lowering other cardiovascular risk factors, and maintaining blood glucose levels in the normal range. Type 2 diabetes mellitus is typically a chronic disease associated with a ten-year-shorter life expectancy. This is partly due to a number of complications with which it is associated, including two to four times the risk of cardiovascular disease, including ischemic heart disease and stroke; a 20-fold increase in lower limb amputations, and increased rates of hospitalizations. In the developed world, and increasingly elsewhere, type 2 diabetes mellitus is the largest cause of non-traumatic blindness and kidney failure. It has also been associated with an increased risk of cognitive dysfunction and dementia through disease processes such as Alzheimer’s disease and vascular dementia. Cardiovascular disease refers to a class of diseases that involve the heart and/or blood vessels. Cardiovascular disease includes Coronary Artery Diseases (CAD) such as angina, myocardial infarction, stroke, heart failure, hypertensive heart disease, rheumatic heart disease, cardiomyopathy, heart arrhythmia, congenital heart disease, aortic aneurysms, peripheral artery disease, and thromboembolic disease. Cardiovascular disease is a major cause of disability and premature death throughout the world, and contributes substantially to the escalating costs of health care. High blood pressure results in 13% of CVD deaths, while tobacco results in 9%, diabetes 6%, lack of exercise 6% and obesity 5%. The contemporary associations of type 2 diabetes mellitus with a wide range of incident cardiovascular diseases have been compared in this study. Results showed that Type 2 diabetes mellitus was positively associated with peripheral arterial disease, ischaemic stroke, heart failure, and non-fatal myocardial infarction, but was inversely associated with abdominal aortic aneurysm and subarachnoid haemorrhage, and not associated with arrhythmia or sudden cardiac death [3-6]. We show that peripheral arterial disease and heart failure are the most common initial presentations of cardiovascular disease in patients with type 2 diabetes. Type 2 diabetes is associated with reduced risk of abdominal aortic aneurysm and possibly subarachnoid haemorrhage. These findings have implications for disease modelling and clinical risk assessment [7].
Patients and Method
Study design: This is a hospital based prospective observational study.
Approval : This study received approval from college ethical committee.
Setting: Owaisi Hospital, Hyderabd.
Participants: 411 patients admitted in Owaisi Hospital.
Study period: December 2015-October 2017
Observations and Results
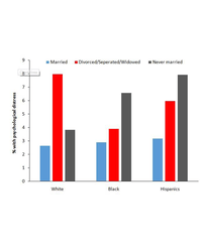
The objective of this study was to investigate and compare associations between type 2 diabetes mellitus and future risk of 12 of the most common initial cardiovascular presentations in men and women. We defined individuals as having diabetes at baseline (type 1, type 2, or uncertain type) on the basis of coded diagnoses recorded in hospital episode statistics at or before study entry. Participants who developed new-onset diabetes during follow-up were analysed according to their baseline status of no diabetes. We compared people with type 2 diabetes to those without diabetes; we excluded people with type 1 diabetes or diabetes of uncertain type. In each participant with diabetes, we assessed glycaemic control by taking the mean of all the HbA1c measurements from 3 years before study entry to 3 years after, ignoring values occurring after an endpoint. For continuous variables (BMI, HDL cholesterol, total cholesterol, and systolic blood pressure) we used, as a baseline value, the most recent measurement recorded in the year before study entry, but included measurements outside this time window in imputation models. Social deprivation was included in models as quintiles of the index of multiple deprivations, a score calculated for each participant’s neighborhood on the basis of social indices such as income, education, and employment. Data recorded before study entry was used to classify participants as never smokers, ex-smokers, or current smokers at baseline. The study included 411 individuals, of whom 356(86.6%) did not have diabetes and 55(13.4%) had type 2 diabetes. People with type 2 diabetes had lower mean HDL cholesterol and higher mean BMI than people without diabetes. The use of statins and antihypertensive medication was greater in people with type 2 diabetes than in those without diabetes, and increased over time. The prevalence of any type of diabetes in all individuals aged 40–50 years (with or without previous cardiovascular disease) was 17.1%. Peripheral arterial disease was the first presentation in 9 (16·2%) of the 55 patients with type 2 diabetes who had cardiovascular events, and heart failure was the first presentation in 8 (14·1%) of these patients. Cumulative incidence curves show substantial differences in the direction and strength of the associations between each of the cardiovascular manifestations and type 2 diabetes mellitus (Table 1) (Figure 1).

Figure 1: Distribution of initial presentations of cardiovascular disease in participants with and without type 2 diabetes and no history of cardiovascular disease.
Table 1: Baseline characteristics of people without cardiovascular diseases at baseline, according to type 2 diabetes status.
| |
No |
Type 2 |
| Diabetes |
Diabetes |
| Age, years(average) |
45 years |
60 years |
| Social deprivation |
19.40% |
27.30% |
| Smoking status |
| Current smoker |
17.60% |
14.40% |
| Ex-smoker |
11.40% |
29.90% |
| Never smoked |
65.80% |
63.70% |
| Systolic blood pressure, mm Hg |
127 |
134 |
| Diastolic blood pressure, mm Hg |
81.4 |
81.7 |
| Total cholesterol, mmol/L |
5.54 |
4.67 |
| HDL cholesterol, mmol/L |
1.3 |
1.13 |
| BMI, kg/m2 |
26.4 |
30.3 |
| Random glucose concentration, mmol/L |
5.65 |
10.2 |
| Fasting glucose concentration, mmol/L |
5.21 |
9 |
| Glycaemic control |
| HbA1c recorded |
12.331 |
14.578 |
| HbA1c, mmol/mol |
47.8 |
59.7 |
| HbA1c <48 mmol/mol (6·5%) |
69.10% |
27.80% |
| HbA1c <48 mmol/mol (6·5%) |
16.90% |
31.09% |
| HbA1c ≥58 mmol/mol (7.5%) |
13.60% |
45.60% |
| Diabetes treatment in year before study entry |
| Diet only |
NA |
34% |
| Metformin |
0.10% |
54% |
| Sulfonylurea |
<0.1% |
41.50% |
| Insulin |
<0.1% |
12.40% |
| DPP-4 inhibitor, meglitinide derivative, or GLP-1 |
<0.1% |
1.40% |
| receptor agonist |
| Cardiovascular preventive treatment in year before study entry |
| Statin |
2.10% |
37.20% |
| Any antihypertensive medication |
17.90% |
56.90% |
| ACE inhibitor |
7% |
33.80% |
| Angiotensin receptor blocker |
0.90% |
7.40% |
| β blocker |
5.60% |
18.30% |
Statistical analysis
We plotted crude cumulative incidence curves for each cardiovascular endpoint for people with no diabetes and those with type 2 diabetes, using age as the timescale. Follow-up was censored at the occurrence of a primary endpoint, death, de-registration from the practice, or the last data collection for the practice, whichever occurred first (Figure 2).

Figure 2: Statistical analysis.
Discussion
Peripheral arterial disease is one of the most common first presentations of cardiovascular disease. Furthermore, of the 12 diseases studied, peripheral arterial disease showed the strongest association with type 2 diabetes. Heart failure was also one of the most common first presentations (accounting for 14·4% of events in people with type 2 diabetes). Our definition excludes heart failure occurring after acute myocardial infarction, but we have to interpret this result with caution because we know that our data sources miss some cases of myocardial infarction. Possible mechanisms might include long-term hypertension, chronic hyperglycaemia, microvascular disease, glycosylation of myocardial proteins, diabetic nephropathy, and autonomic neuropathy. A novel finding was the association of type 2 diabetes with reduced incidence of two major aneurysmal diseases: abdominal aortic aneurysm and subarachnoid haemorrrhage. An inverse association between diabetes and abdominal aortic aneurysm has been suggested by cross-sectional studies of abdominal aortic aneurysm screening and case-control studies [8-13].
Conclusions
Type 2 diabetes mellitus was positively associated with peripheral arterial disease, ischaemic stroke, heart failure, and non-fatal myocardial infarction, but was inversely associated with abdominal aortic aneurysm and subarachnoid haemorrhage, and not associated with arrhythmia or sudden cardiac death. Heart failure and peripheral arterial disease are the most common initial manifestations of cardiovascular disease in type 2 diabetes. The differences between relative risks of different cardiovascular diseases in patients with type 2 diabetes have implications for clinical risk assessment and trial design. Management should be tailored to improve the quality of life of individuals with type 2 diabetes mellitus.
References
1. Scirica BM, Bhatt DL, Braunwald E. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus. N Engl J Med. 2013; 369: 1317-1326.
2. Emerging Risk Factors Collaboration Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet. 2010; 375: 2215-2222.
3. Kannel WB, McGee DL. Diabetes and cardiovascular disease: the Framingham study. JAMA. 1979; 241: 2035-2038.
4. Nordon IM, Hinchliffe RJ, Loftus IM, Thompson MM. Pathophysiology and epidemiology of abdominal aortic aneurysms. Nat Rev Cardiol. 2011; 8: 92-102.
5. Peters SAE, Huxley RR, Woodward M. Diabetes as risk factor for incident coronary heart disease in women compared with men: a systematic review and meta-analysis of 64 cohorts including 858,507 individuals and 28,203 coronary events. Diabetologia. 2014; 57: 1542-1551.
6. Rapsomaniki E, Timmis A, George J. Blood pressure and incidence of twelve cardiovascular diseases: lifetime risks, healthy life-years lost, and age specific associations in 1·25 million people. Lancet. 2014; 383: 1899-1911.
7. Denaxas SC, George J, Herrett E. Data resource profile: cardiovascular disease research using linked bespoke studies and electronic health records (CALIBER). Int J Epidemiol. 2012; 41: 1625-1638.
8. Department for Communities and Local Government English indices of deprivation 2010: technical report.
9. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2014; 37: S81-S90.
10. National Collaborating Centre for Chronic Conditions. Type 2 diabetes: national clinical guideline for management in primary care.
11. Health and Social Care Information Centre. Department of Health Quality and outcomes framework.
12. Siu AL. Screening for Abnormal Blood Glucose and Type 2 Diabetes Mellitus: U.S. Preventive Services Task Force Recommendation Statement. Annals of Internal Medicine. 2015; 163: 861-868.
13. Malanda UL, Welschen LM, Riphagen II, Dekker JM, Nijpels G, Bot SD. Self monitoring of blood glucose in patients with type 2 diabetes mellitus who are not using insulin. Cochrane Database of Systematic Reviews. 2012; 1: CD005060.