Review Article | Volume 2 - Issue 1 | Article DOI :
Download PDF
Nur Chayati M Kep1,2*, Christantie Effendy3 and Ismail Setyopranoto4
1Faculty of Medicine, Universitas Gadjah Mada, Indonesia 2Faculty of Medicine and Health Sciences, Universitas Muhammadiyah Yogyakarta, Indonesia 3Medical Surgical Nursing Departement, Universitas Gadjah Mada, Yogyakarta, Indonesia 4Department of Neurology, Universitas Gadjah Mada, Yogyakarta, Indonesia
Corresponding Author:
Nur Chayati M Kep, Faculty of Medicine
and Health Sciences, Universitas
Muhammadiyah Yogyakarta, Tegalsari Rt
01 Ngrame Tamantirto Kasihan Bantul,
Indonesia, Tel: +6285794226267;
Keywords
Home care; Quality indicators; Stroke; HCQI; Instrument validation
Abstract
Introduction: Even though many quality indicators of health care have been announced, those which specify in home care services are limited in that none of them describe the stroke patients’ condition.
Aim: To determine through systematic literature review what methods can be used to assess the quality of home care that patients received and to identify what components can be used as a determinant of the quality of home care services.
Methodology: Google Scholar, EBSCO, ProQuest and PubMed database websites were searched for articles and information.
Results: The method that was used is a qualitative study using a literature review with quantitative analysis of a previously accepted research instrument with a questionnaire that has been widely available and considered reliable. The researchers identified thematic differentiation in grouping the quality indicators used by those articles. The first article stated 23 quality indicators, which are distributed as the following: functional (n=8), clinical (n=10), social and treatment (n=5). The second article discussed two groups of quality indicators based on 21 items: prevalence (n=15), and incidence (n=6), while the last article mentioned 16 quality indicators without any category. Overall quality indicators in home care that are used by the three articles are based on the Home Care Quality Indicators Instrument (HCQIs).
Conclusion: Several studies discussed home care quality indicators but no articles specifically analyze home care provision for stroke patients. Further research is needed to clarify the components indicators for stroke patients and more importantly, these indicators should be valid, and reliable.
Citation
Kep NCM, Effendy C and Setyopranoto I. Quality Indicators in Home-Based Care: A Systematic Review. J Gen Med. 2018; 2(1): 1009.
Background
In the context of functional dependencies, home care is a significant alternative treatment for stroke patients. The main role of the home care provider is to teach skills to the family/caregiver and to give informal support. Caregivers are responsible for continuing treatment that has been taught by the medical team [1]. Home care aims to help many people with different levels of dependence to stay at home rather than being treated in a hospital for an extended period of time [2]. In providing care, homecare should be in accordance with the needs of patients, for which all teams must be able to work together to reduce the caregiver’s burden, so the caregiver can better play a role in disease prevention and health promotion.
Quality of care services is the critical aspect that ensures the patient safety, therapeutic effect, patients’ comfort and pleasure, and it also saves time, power, effort, energy, cost and material. Therefore, it leads to the best quality care, with an ease of doing and an ability to adapt to changes [3,4]. The assessment of service quality consists of the structure, process and outcome of the provision of home care [5]. To have quality home care and meet the corresponding demands of the times, the care providers must be able to adapt to the complexity of the patient’s needs and the type of service [6].
Quality in the interpersonal perspective can be measured by the degree of adherence to social values. In the home care setting, a nurse should assess the holistic care and patient-centered care with regard to the value of patients and families [6]. Interpersonal relationships are considered as an essential natural factor and interpersonal skills are considered as professional competences needed to carry out patient-centered care so that high quality of service can be achieved.
One method to identify the level of performance is using quality indicators, which are defined as a marker that indicates whether there is potential for poor service or bad outcomes [7]. Quality indicators measure the care provider’s performance in terms of quality of care that is given. Its function provides a quantitative basis for monitoring and evaluating the services. The evaluation report can be used to identify any deficiency in service and to measure the quality as objective as possible [4].
Recent research mentioned that there are two steps to develop evidence-based clinical indicators, the planning phase and the development phase. The planning phase focuses on choosing the clinical area that will be evaluated, and also selecting and organizing the measurement team. In the development test, the measurement team selects the clinical indicators from scientific sources, designs the specific measurement and then conducts the preliminary test or pilot test to identify the items that need further modification and specification [8].
The purpose of developing quality indicators is to identify the clinical areas that need improvement and to provide a measurement for quality care provision [7]. In order to evaluate the effectiveness of home care interventions, standards of performance assessment are required for documenting the changes that occur in patients [9]. The aims of this systematic review are firstly to find out what methods can be used to assess the quality of home care that patients received and secondly to identify the currently existing quality indicators that are evidence based and are used to monitor and to evaluate stroke patients in home care setting.
Methods
Data source
An article search process was conducted from January to May 2016, through the Google Scholar database, PubMed, Proquest, and Ebsco. The key words used in the search for the articles were “quality indicator”, “quality of care”, “quality homecare”, “home care evaluation” “quality of health care” and “stroke patient” using the Boolean word “AND”.
Study selection
Selection of the articles was based on the research objective that discusses quality indicators for home care services, especially in patients with chronic diseases, with a focus on stroke patients. Homecare is conducted by a multidisciplinary team, and quality evaluation of homecare programs is taken from patients, families and caregivers. The published articles taken from 2007 to 2016, are only in English language, full text, and include both qualitative and also quantitative researches. Three reviewers performed the eligibility assessment independently.
Data extraction
The number of articles that was obtained using the above keywords was 205 articles. Then after the initial selection based on the appropriate title and abstract, only 51 articles were considered. Based on the inclusion and exclusion criteria, finally there were only three articles that could be analyzed. Analysis of the articles was conducted using the content analysis method, without any statistical test. The process of extracting articles can be seen in the workflow chart in Figure 1.

Figure 1: PRISMA flow diagram for search and selection of studies for structured review [12].
The authors classified indicators according to the dimension of quality of care as structure, process, or outcome indicators [5].
Results
General description Article searching was completed over a 5 month period, and as a result 205 articles related to the home care quality indicators were found. Finally only 3 articles from critical appraisal processes were selected that are appropriate with inclusion criteria. However, there were no articles that discussed home care quality indicators specifying stroke condition. Over all, the three selected articles used a common instrument from Hirdes et al., [9] who had earlier developed the quality indicators instrument for home care provision.
Quality of care indicators in home care service include 23 items that are divided into clinical, functional and social outcomes. Instrumental Activity Daily Living (IADL) as part of functional indicators becomes a centre of attention in homecare because most of the home care population experience decline in their IADL. Whereas clinical indicators consist of physical and mental states such as mood condition, and procedural indicators can be seen for example from flu vaccination awareness. Feeling alone and distress are social indicators that also commonly happen in patients [10].
Meanwhile, Mofina uses 22 items as quality of home care indicators, which are divided into 2 groups, namely prevalence and incidence [11]. The prevalence of quality of home care indicators consists of inadequate meals, weight loss, dehydration, no medication review by medical doctor, Activity Daily Living (ADL)/rehabilitation potential and no therapies, falls, social isolation, delirium, negative mood, disruptive or intense daily pain, inadequate pain control, neglect or abuse, any injuries, no influenza vaccination, and hospitalization. Moreover, bladder incontinence, skin ulcers, ADL impairment, impaired locomotion in home, cognitive decline and difficulty in communication are the incidences of quality of home care indicators. The studies’ characteristics used in this review are shown in Table 1 and Table 2.
Table 1: The journal method used in the review.
| Journal |
Research design |
Methodology |
Data collection* |
Samplesize |
Number of quality indicators |
Selection criteria¶ |
| Foebel et al.2015 [10] |
Prospective |
Quantitative |
Questionnaire |
1.354 |
23 indicators |
Guidelines |
| Mofina, AM.2010. [11] |
Prospective |
Quantitative |
Questionnaire |
111.804 |
21 indicators |
Guidelines |
| Bos et al.2007. [7] |
Cross sectional |
Quantitative |
Questionnaire |
65 |
16 indicators |
Guidelines |
* instrument used to gather the data from respondents; ¶ source of data instrument
Table 2: Categorization of HCQIs based on structure, process and outcome.
| Item indicators |
S |
P |
O |
References |
| ADL improvement |
|
|
√ |
[7,10,11] |
| ADL decline |
|
|
√ |
[7,10,11] |
| Bladder incontinence decline |
|
|
√ |
[10,11] |
| Bladder incontinence improvement |
|
|
√ |
[10,11] |
| Cognitive improvement |
|
|
√ |
[10] |
| Cognitive decline |
|
|
√ |
[10,11] |
| Communication improvement |
|
|
√ |
[7,10,11] |
| Communication decline |
|
|
√ |
[10,11] |
| Falls |
|
|
√ |
[7,10,11] |
| IADL improvement |
|
|
√ |
[10] |
| IADL decline |
|
|
√ |
[10] |
| Any injuries |
|
|
√ |
[7,10,11] |
| Mood improvement |
|
|
√ |
[10] |
| Mood decline/ negative mood |
|
|
√ |
[7,10,11] |
| Pain not controlled |
|
|
√ |
[7,10,11] |
| Pain improvement |
|
|
√ |
[10] |
| Daily severe pain |
|
|
√ |
[7,10,11] |
| Continued caregiver distress |
|
|
√ |
[10] |
| Alone and distresses |
|
|
√ |
[7,10,11] |
| Used to go out |
|
|
√ |
[10] |
| No flu vaccine in last 2 years |
|
|
√ |
[7,10,11] |
| Hospitalization and emergency departement use |
|
|
√ |
[7,10,11] |
| Weight loss |
|
|
√ |
[7,10,11] |
| Neglect or abuse |
|
|
√ |
[7,11] |
| Inadequate meals |
|
|
√ |
[7,11] |
| Social isolation |
|
|
√ |
[7,11] |
| No assistive device among clients with difficult locomotion |
|
|
√ |
[7,11] |
| Delirium |
|
|
√ |
[7,11] |
| No medication review by at least one physician |
|
√ |
|
[7,11] |
| Dehydration |
|
|
√ |
[7,11] |
| Skin ulcers |
|
|
√ |
[11] |
Type of indicators: S (structure) (n=0), P (Process) (n=1) and O (Outcome) (n=30)
Table 1 show that the three articles used a quantitative analysis method for gathering the data. Two studies represent experiences made in Europe [7,10] and the other one in the USA [11]. According to study design, two are prospective studies [10,11] and one is a cross sectional study [7] but all of the selected studies aim to assess the quality of care given to home care patients. All indicators proposed were taken from previously established, generally accepted and considered reliable guidelines.
From the 3 studies, the number of quality indicators is different among them. Thirty items are related to outcome quality indicators and one is a process indicator (Table 2). All of them adopt the same instrument, the Home Care Quality Indicators (HCQIs) that is downgraded from the Minimum Data Set HCQIs instrument. Indicators that are stated in HCQIs have a strong relationship with the quality of home care services statistically. The main characteristic of all of the studies is the quality of care assessment and not the approach to the validity of home care quality indicators [11].
Discussion
Quality indicators are a measurement tool that has some advantages for monitoring and evaluating the governance, and management of supported daily functions and activities [12]. Indicators serve as a quantitative based instrument that guides clinicians, organizations, and planners to obtain improvement in care and in processes of care that are provided [13].
The scope of service quality presently is not to focus on the performance of health workers, but more directed to the services received by patients or the public, so that the instrument used to assess the quality of service is also different depending on the scope of what will be examined [5]. Quality indicators can be accessed through three approaches: structure, process and outcome [5]. Structure indicators assess the organization as a main source of care, for example, facilities, equipments, human sources, and organization characteristics. Characteristics of organization include nursing and medical staff, teaching and research activity, supervision, performance and payment system. Process indicators review what the health professionals have given to the customers such as medical treatment, nursing care, rehabilitation program, health education, prevention program with involvement of patients themselves and their family. Outcome indicators measure individual or population health changes either desired or not. They can be used as a measure of knowledge, behavior, and patient satisfaction. To date there is nothing better than these three components because of how the structure and outcome-process are interconnected. Overall, process and outcome are considered valid measures of quality by the international medical community.
To evaluate the home care services for guaranteeing their quality, an accurate evaluation instrument is required. This instrument should be responsible for reliability and validity. This study found that the instrument that is used mostly is from the available guidelines. In depth interviews and face to face interviews are considered the best way to obtain the quality of service opinions and to identify any specific problems in health care. The interviewing process for gathering the information about the quality of home care can be obtained from the patient, the family/caregiver and health officer [14].
In this review of three recent related studies, the authors found the common indicators that are used to measure the quality of home service care and their development. Most of them are outcome indicators. Through this review, the author has an overview of the most relevant aspects that should be observed when assessing home care while those that are more relevant with stroke care are limited. The guidelines method is used to select them even though little information has been described about their validation method.
The home care philosophy changes the patient’s condition from being the receiver of care to becoming an independent patient [15]. The outcome of home care service with a patient centered rehabilitation practice approach should be built with active participation from the patient and family. There are basically 4 home care outcomes: Extended Activities of Daily Living (EADL), Activities of Daily Living (ADL), Quality of Life (QoL) and Cognitive Impairment (CI) status [16]. The focus on positive outcomes emphasizes an intervention service that has the priority for quality home care provision [17].
Home care quality can be judged from the functional, clinical and social outcomes [10]. Functional indicators include eight components: IADL increased/decreased, increased or decreased ADL, cognitive decline/rising, and communication increased/ decreased. Clinical indicators consist of 10 criteria: weight loss, falls, injury, severe pain, pain controlled, increased pain, improve/decrease mood, bladder function increase/decrease. With the same variables, Mofina separated them into the incidence and the prevalence of home care quality indicators [11].
The three articles used quality indicators from one reliable source, Home Care Quality Indicators (HCQIs). Hirdes et al., [9] developed the first generation of HCQIs from the Minimum Data Set tool, and then this instrument was refined as the second generation of HCQIs by Foebel et al., [10]. Moreover, defining the core set of indicators should consider local values and family and patient preferences. The criteria for quality of service are different in each setting because it is influenced by many factors [5]. Indicators of homecare quality that had been proposed by Bos et al., [7] consisting of 16 components of HCQIs resulted in varying scores in some countries in Europe. Some components are more dominant than the other components although they are on the same continent. Some items also did not match the contexts between one country and another so additional research should involve an international effort to validate a universal or country specific instrument.
In terms of the design, overall the researchers employed quantitative analysis methods. There are other considerations proposed that indicate a preference for the use of mixed methods when evaluating a home care program [18]. Several instruments and methods can be used together with surveys, patient outcomes, quality measurement, qualitative interviews, participant observation, and a pre/post evaluation process. But in practice barriers are often encountered such as the limited number of trained staff to perform multiple evaluation methods, the burden of the collection of data, and unexpected status changes.
Generally homecare stroke patients experience a lowered quality of life, specifically in interpersonal relationship domain, sleep, cognitive level, and mental health and pain, so the homecare purposes are to improve the quality of life, to motivate and to inform the patients of care options [19]. Mostly the home care patients after stroke experience decrease in their functional capacity within 3 months. Although the homecare is able to mitigate this condition, the main activity of homecare is to provide quality care for the patient rather than to facilitate the independence of that patient [16].
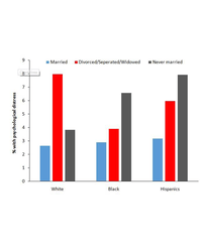
Psychological need is the most unmet need in home care, such as the desire to be accompanied, to do free time activities and to be free from psychological distress. The patients and family also complain about information that can not delivered by health employees. In contrast, physical needs mostly become the main reason for interaction between caregiver and the patients [20]. Therapeutic personal care given by a nurse can minimize the adverse events in home care [21] for example fall incidence, weight loss, urinary tract infection, caregiver distress, decrease in ADL, pressure ulcer, new emergency visit, new hospitalization and non adherence with medication.
The long term home care should be evaluated because it affects the patient’s quality of life. In related research, the quality of life of post fracture patients with home care during the following 36 months (3 years) is reported to show decrease [22]. The quality of life in home care patients overall is mostly lowered [19]. Accordingly, there is a relationship between quality of care and patients’ satisfaction; the lower the quality of care, the higher patients dissatisfaction is about accurate information, inter services coordination, financial support and access to health services in the community. As a result, stroke survivor satisfaction is a key to measure and improve the quality of home care.
A common characteristic of the selected studies is that most of the researches assess the quality of care. There is no study that mentioned about an evaluation of the validity of the quality indicators. As a result it is necessary to analyze the validity, reliability and applicability of each indicator to develop an instrument appropriate for providing home care for stroke patients.
The three studies chosen were conducted in Europe and the USA. As a result, the quality indicators are suitable with the homecare situation in those countries. Some indicators may fit to a specific country or continent but not to others. So the homecare quality indicators as explained in this study need further investigation when they will be applied in other countries and in different target populations.
Conclusion
Based on a thorough literature review, the most reliable components of quality of home care indicators are based on Home Care Quality Indicators Instruments. The quality indicators of home care are also still common to all patients, but no measure of quality of care was available specifically for stroke patients. Further investigation is required for developing an instrument that is appropriate for assessing the quality of home care service for stroke patients based on the generally accepted indicators that have been declared reliable by the quality care providing community.
Authors’ contribution
NC participated in data collection process, arranged the design, carried out the systematic review, coordination and drafted the manuscript. CE participated in analyzing the result and helped to draft the manuscript. IS contributed in study design, drafted the manuscript and reviewed the manuscript.
Acknowledgements
Thank you to Associate Professor, DR. Ratana Somrongthong who suggested more direction for this manuscript improvement, Klinik Bahasa (Language Clinic) Faculty of Medicine Universitas Gadjah Mada and all who support the research process.
Funding
The research was funded by the Directorate General of Higher Education and University of Muhammadiyah Yogyakarta, Indonesia.
References
1. Gratao ACM, Talmelli LF da S, Figueiredo LC, Rosset I, Freitas CP, Rodrigues RAP. Functional Dependency of Older Individuals and Caregiver Burden. Rev Esc Enferm USP. 2013; 47: 134-141.
2. Ajlouni MT, Dawani H, Diab SM. Home Health Care (HHC) Managers Perceptions About Challenges and Obstacles that Hinder HHC Services in Jordan. Glob J Health Sci [Internet]. 2015; 7: 121-129.
3. Sale D. Quality Assurance. 1996; 1-143.
4. Stalpers D, Kieft RAMM, Linden D Van Der, Kaljouw MJ, Schuurmans MJ. Concordance between nurse-reported quality of care and quality of care as publicly reported by nurse-sensitive indicators. BMC Health Services Research. 2016; 1-8.
5. Donabedian A. The quality of care. How can it be assessed? JAMA. 1988; 260: 1743-1748.
6. Nakrem S. Understanding organizational and cultural premises for quality of care in nursing homes: an ethnographic study. BMC Health Services Research. 2015; 15: 508.
7. Bos JT, Frijters DHM, Wagner C, Carpenter GI, Finne-Soveri H, Topinkova E, et al. Variations in quality of Home Care between sites across Europe, as measured by Home Care Quality Indicators. Aging Clin Exp Res. 2007; 19: 323-329.
8. Mainz J. Developing evidence-based clinical indicators: a state of the art methods primer. Int J Qual Health Care. 2003; 15: i5-11.
9. Hirdes JP, Fries BE, Morris JN, Ikegami N, Zimmerman D, Dalby DM, et al. Home care quality indicators (HCQIs) based on the MDS-HC. Gerontologist. 2004; 44: 665-679.
10. Foebel AD, van Hout HP, van der Roest HG, Topinkova E, Garms-Homolova V, Frijters D, et al. Quality of care in European home care programs using the second generation interRAI Home Care Quality Indicators (HCQIs). BMC Geriatrics; 2015; 15: 148.
11. Mofina AM. A Comparison of Home care Quality Indicators and The Influence of Risk Adjustment Between Two Provinces. 2010.
12. Klazinga N, Stronks K, Delnoij D, Verhoeff A. Indicators without a cause. Reflections on the development and use of indicators in health care from a public health perspective. Int J Qual Health Care. 2001; 13: 433-438.
13. Althabe F, Bergel E, Cafferata ML, Gibbons L, Ciapponi A, Aleman A, et al. Strategies for Improving The Quality of Health Care in Maternal and Child Health in Low and Middle Income Countries: Overview of Systtematic Review. Paediatr Perinat Epidemiol. 2008; 22: 42-60.
14. Firbank OE. Connecting the voices of users, caregivers and providers on service quality. Int J Health Care Qual Assur. 2012; 25: 403-420.
15. Parson J, Rouse P, Robinson EM, Sheridan N, Caonnolly MJ. Goal setting as a feature of homecare services for older people : does it make a difference ? Age Ageing. 2012; 41: 24-29.
16. Parsons JG, Parsons MJ. The effect of a designated tool on person-centred goal identification and service planning among older people receiving homecare in New Zealand. Heal Soc Care Community. 2012; 20: 653-662.
17. Gethin-Jones S. Familial perceptions of the impact of outcome-focused homecare with older people experiencing dementia and living alone. Emerald Gr Publ. 2014; 18: 90-96.
18. Goldman RE, Parker DR, Walker J, Eaton CB, Borkan JM. Recommendations for a Mixed Methods Approach to Evaluating the Patient-Centered Medical Home. Ann Fam Med. 2015; 13: 168-175.
19. Baumann M, Bihan E Le, Chau N. Associations between quality of life and socioeconomic factors, functional impairments and dissatisfaction with received information and home- care services among survivors living at home two years after stroke onset. BMC Neurol. 2014; 14: 1-25.
20. Andrea C, Castillo M. The Needs of Older People with Dementia Living at Home. University College London; 2008.
21. Wai W, Sun L. A Mixed Methods Study : Examining the Relationship between Therapeutic Self-Care and Adverse Events for Home Care Clients in Ontario, Canada. 2014.
22. Tarride J, Burke N, Leslie WD, Morin SN, Adachi JD, Papaioannou A, et al. Loss of health related quality of life following low-trauma fractures in the elderly. BMC Geriatrics. 2016; 1-11.