Transplant Renal Artery Stenosis Following Ex vivo Renal Artery Endarterectomy: Report on Two Cases
Introduction: Transplant renal artery stenosis (TRAS) is the most common vascular complication following kidney transplantation. Deceased donor kidneys exhibiting severe atherosclerosis involving the renal artery, if untreated, represent one cause of TRAS.
Methods: We report herein two cases of TRAS that occurred following back bench ex vivo eversion endarterectomy (EE) prior to deceased donor kidney transplantation (DDKT).
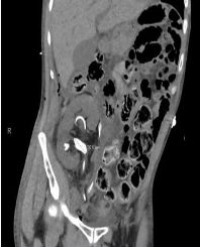
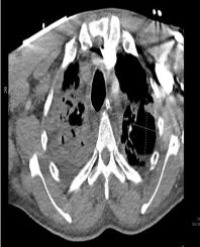
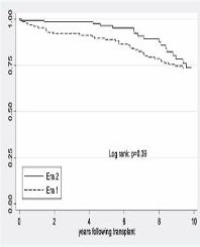
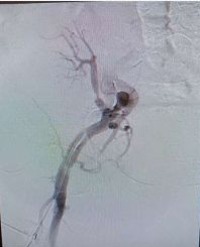
Results: Both patients presented in the first year following DDKT with worsening hypertension and one patient experienced acute kidney injury. Duplex ultrasonography was suspicious for markedly elevated renal artery velocities in the proximal to mid-renal artery segment with evidence for distal turbulence. Subsequent arteriography through an ipsilateral femoral approach confirmed severe TRAS that was successfully treated with balloon angioplasty and stenting. Both patients experienced improvements in blood pressure control, and one patient had resolution of acute kidney injury.
Conclusion: Ex vivo EE may be performed successfully as a rescue procedure to prevent nonuse of donor kidneys with severe intrinsic atherosclerosis. However, these patients may still be at risk for developing TRAS, possibly from a localized dissection occurring secondary to an intimal flap.
Rana Kumar, Arianna Cabrales, Giuseppe Orlando, Christopher Webb, Emily McCracken, Alan C. Farney, and Robert J. Stratta*