Case Report | Volume 2 - Issue 1 | Article DOI :
Download PDF
Kuzucu EA, Çalışkan E, Bayrak ZS, Öcal D, Çağatay M, Saltaş H and Erdem G*
Department of Medical Microbiology, University of Health Sciences, Turkey
Corresponding Author:
Erdem G, Department of Medical Microbiology, University of Health Sciences, D??kap? Y?ld?r?m Beyaz?t Training and Research Hospital, Sehit Omer Halisdemir Caddesi, No:12, 06110, Altindag, Ankara, Turkey, Tel: +90 312 5962680; Email: gul-bahar93@hotmail.com
Keywords
Eikenella corrodens;
Human Bite;
Wound Infection
Abstract
Since Eikenella corrodens is part of the normal oral flora, it can be isolated from fist fight and human-bite injuries. Suspicion of the clinician, collection of adequate specimen, and proper culture technique will improve its isolation in the laboratories. Here we report a case of wound infection due to Eikenella corrodens in a 27-year-old female patient after biting herself during examination at the emergency ward.
Citation
Kuzucu EA, Çalışkan E, Bayrak ZS, Öcal D, Çağatay M, Saltaş H, et al. Eikenella corrodens Wound Infection Secondary to Self-Bite: Case Report. Ann Burns and Trauma. 2018; 2(1): 1005.
Introduction
Eikenella corrodens is a slow-growing, fastidious, nonmotile, facultative anaerobic gram negative bacillus. It is normally found in the flora of oral cavity, upper respiratory, gastrointestinal and genitourinary tracts [1,2]. Although previously believed to be non pathogenic,Eikenella species have been shown to cause various infections in human such as; pulmonary infection, empyema, arthritis, endocarditis, pancreatic abscesses, human and animal bite wound infection [1,3,4]. In many studies E.corrodens has been detected as the causative agent resulting in infections due to human bites. Although human bites are less common than animal bites, injuries caused by human bites must not be underestimated due to high risk of serious complications [1,5]. The bacteriology of human bite wounds reflects aerobic and anaerobic normal oral flora [6].
Because of the overgrowth of fast growing organisms those may be found on the surface of the wounds,Eikenella species can be missed. So during examination of wounds or abscesses after human bites, it must be kept in mind that E.corrodens may be the suspected agent and it should be treated immediately.
Here we report a case of wound infection due to E.corrodens in a patient, with psychiatric disorder, after biting herself during examination at the emergency department.
Case Report
A 27-year-old female patient with no previous history or medication of psychiatric disorder applied to the emergency service of University of Health Sciences, Dışkapı Yıldırım Beyazıt Training and Research Hospital with complaints of nonsense speech, nervousness, self-harm and harm to surrounding people. During examination at the emergency service, she bit the tip of her left thumb seriously. After several blood analyses and radiologic examinations she was hospitalized at psychiatry clinic.
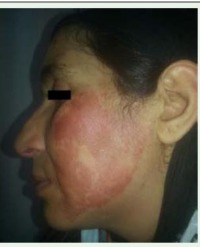
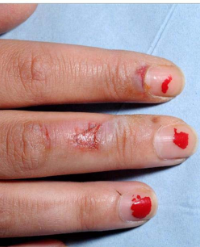
On the second day of hospitalization a malodorous discharge developed on the bite wound. Plastic surgery was consulted (Figure 1A,1B).

Figure 1A: Patients thumb on the second day.

Figure 1B: Patients X Ray on the second day.
Plastic surgery planned reconstructive surgery, dressing was done, elevation and tetanus prophylaxis were suggested, amoxicillin-clavulanic acid 1000 mg orally every 12 hours was started as antimicrobial therapy.
Because of the lack of healing in the lesion, infectious diseases and plastic surgery sections were again consulted. Wound culture swab specimens, which were not collected in the first visit, were collected by recommendation of infectious diseases clinician and ampicillin-sulbactam (2 g ampicillin+1g sulbactam) IVq 6hr for 5 days regimen was started.
Gram-stained smears of the swab specimens revealed; few epithelial cells, few Polymorphonuclear Leukocytes (PMNL), few gram positive cocci and gram negative bacilli.
The specimen was plated on Columbia agar with 5% sheep blood (BDTM,Becton Dickinson), Eosin-Methylene-Blue (EMB, BDTM,) and chocolate agars (BDTM), at the microbiology laboratory, and incubated for 48 hrs at 5-10% CO2 ambient air at 37°C.
At the end of 48 hrs incubation, no growth was observed on EMB agar plate, on the other hand small pitting colonies with bleach like odor and greenish discoloration around, were grown on blood agar plates. Gram negative thin bacilli were seen on Gram stain (Figure 1C,1D).

Figure 1C: Small pitting and oxidase positive colonies.

Figure 1D: Gram negative bacilli on Gram stain.
Results of the biochemical tests were as follows; catalase, indole, urease, and motility tests negative, oxidase test positive. Identification of the strain to the species level was done by both BD Phoenix™(Becton Dickinson,USA) automated system and MALDI-TOF mass spectrometry (Bruker,Germany), and detected as E.corrodens which was also suspected before, with its pitting and bleach like odor colonies. After ampicillin-sulbactam (2 g ampicillin+1g sulbactam) IV q 6hr for 5 days regimen, treatment was continued with 10 days of amoxicillin-clavulanic acid (1000mg orally every 12 hours) therapy.
The patient whose psychiatric symptoms receded was discharged with a diagnosis of dissociative disorder and proposal of infectious diseases, psychiatry, neurology outpatient clinic control.
Oral consent was approved for use of patient’s photos.
Discussion
Although being an inhabitant of the oral cavity and upper respiratory tract, E.corrodens may lead to serious infections after injuries, particularly human bites and fist fight injuries. Stoloff et al., published a series of 33 cases,18(54.5%) of which were due to human bites and fist injuries. In our case, E.corrodens was isolated also from a wound as a result of human bite [2].
Although declined, still 5% of the patients undergo amputation because of serious complications in human bite traumas [6].
To avoid a delay in diagnosis, the clinician must suspect of an infection of E. corrodens if the history of the patient harbours such truma. Isolation depends on collection of adequate specimen, and carefull evaluation of the plates of wound cultures at least after 48hrs of incubation [2].
E.corrodens belong to “AACEK” (formerly “HACEK”) group organisms. This abbreviation stands for Aggregatibacter aphrophilus (formerly Haemophilus aphrophilus and H.paraphrophilus), Aggregatibacter actinomycetemcomitans (formerly Actinobacillus), Cardiobacterium hominis, E.corrodens, and Kingella kingae and other Kingella spp [7]. Since HACEK microorganisms are fastidious, antimicrobial susceptibility testing is impractical for many laboratories, and published reports and guidelines usually guide antimicrobial selection of the clinican [8]. The organism is typically susceptible to many antibiotics, including penicillin G,ceftriaxone, ampicillin, amoxicillin–clavulanic acid, trimethoprim sulfamethoxazole, and fluoroquinolones, but resistant to oxacillin,cefazolin,clindamycin, and erythromycin [3,6,7,9].
E.corrodens is less fastidious, compared with the other organisms in the AACEK group, and may generally be recovered within 24 to 48 hrs on routine blood and chocolate agar media, as in our case [7]. Despite initiation of a broad spectrum, amoxicillin-clavulanic acid, therapy, covering both aerobic and anaerobic flora members of oral cavity, as the severity of symptoms increased, to prevent a possible complication of osteomyelitis, treatment was changed to parenteral ampicillin-sulbactam in this case.
Management of such injuries include immediate multidisciplinary approach; surgery, infectious diseases and laboratory disciplines must act together as in this case [1,10]. Surgical debridement, isolation of the organism and administration of accurate antimicrobial therapy improved the wound healing of our patient.
Acknowledgement
This study is presented at 10th Balkan Congress of Microbiology,16-18 November 2017, Bulgaria.
References
1. Sula B, Tekin R. Soft tissue abscess due to Eikenella corrodens after human bite. Journal of Microbiology and Infectious Diseases. 2016; 6: 36-37.
2. Stoloff AL, Gillies ML. Infections with Eikenella corrodens in a general hospital: A report of 33 cases. Reviews of Infectious Diseases. 1986; 8: 50-53.
3. Paul K, Patel SS. Eikenella corrodens infections in children and adolescents: case reports and review of the literature. Clinical Infectious Diseases. 2001; 33: 54-61.
4. Yakut N, Kepenekli Kadayıfçı E, Karaaslan A, Atici S, Akkoc G, Ocal Demir S, et al. Deep neck infection caused by Eikenella corrodens coinfection with Streptococcus mitis and Streptococcus oralis in an infant. Turkish Journal of Pediatric Disease. 2017; 3: 203-205.
5. Raval P, Khan W, Haddad B, Mahapatra AN. Bite injuries to the hand - review of the literature. The Open Orthopaedics Journal. 2014; 8: 204-208.
6. Goldstein EJC. Bite wounds and infection. Clinical Infectious Diseases. 1992; 14: 633-640.
7. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases (Eighth Edition). Eikenella corrodens. 2015.
8. Coburn B, Toye B, Rawte B, Jamieson FB, Farrell DJ, Patel SN. Antimicrobial susceptibilities of clinical isolates of HACEK organisms. Antimicrobial Agents and Chemotherapy. 2013; 57: 1989-1991.
9. Billingsley EM. Paronychia Organism-Specific Therapy. Medscape Drug Reference. 2016.
10. Tricarda T, Bunda L, Alhefzia A, Lemoine JP, Schneider L, Karger C, et al. Eikenella corrodens bone and hipjoint infection. A case report and literature review. Arch Pediatr. 2016; 23: 1146-1149.