Case Report | Volume 1 - Issue 1 | Article DOI :
Download PDF
Othman D*, Abdel-Rehim S and O’Boyle C
Burns and Plastic Surgery Unit, Nottingham University Hospitals NHS Trust, UK
Corresponding Author:
Diaa Othman, Burns and Plastic Surgery
Unit, Nottingham University Hospitals
NHS Trust, Nottingham, UK,
Tel: +44 115 969 1169;
Abstract
Burns are a common global cause of injury; however iatrogenic burns are rare and preventable mode of injury. We report two cases who sustained superficial partial thickness burns from ECG monitoring leads during Magnetic Resonance Imaging (MRI). The two patients have sustained 0.2% and <1% superficial partial thickness burn of their Total Body Surface Area (TBSA) respectively. Common features included a relatively long duration of spine MR scanning (90 and 30 minutes) and high Body Mass Index (BMI). Both patients made uneventful recovery and were discharged within 24 hours of admission. It is still uncertain whether injuries were thermal or electrically-induced, however several mechanisms have been implied. These include electromagnetic inductionheating, the antenna effect and current induction through a closed loop. In this report, we discuss the proposed mechanisms of injury and highlight the fundamental need for staff education, and preparing national guidelines and safety checklists to prevent similar injuries in the future.
Citation
Othman D, Abdel-Rehim S and O’Boyle C. MRI-Induced Burns from ECG Leads: Thermal or Electrical Burns?. Ann Burns and Trauma. 2017; 1(1): 1004.
Introduction
Burn injuries often have emotional and physical consequences on patients and their families. Burns units are most commonly presented with thermal injuries (95%), followed by chemical and electrical burns (5%) [1]. Most thermal burns are flame-induced, scald or contact burns from household items. Most thermal burns are sustained outside of the hospital setting; however, a small minority may also occur during patient investigations or treatment. We report two cases who sustained superficial burns from an unusual mechanism induced by ECG cables used during Magnetic Resonance Imaging (MRI).
Burns caused by MRI are rare [2].While most physicians are aware of the absolute contraindications to MRI,less are familiar with the potential for an MRI-induced thermal or electrical burn associated with electrical monitoring devices. Dempsey et al.,[3] review article represents the largest series of MRI associated burns to date. Approximately 150 cases of burns to patients during MRI procedures were described;interestingly only one case has been reported to have burns at the site of an ECG cable, while most other ECG-related burns have been related to ECG metal electrodes.
The clinical application of MRI equipment is not risk-free.Those two cases are amongst the f irst to be reported from magnetic resonance imaging in our institution.The purpose of this case report is to highlight the mechanisms of injury, safety measures and current guidelines issued by the Department of Health (DoH) whilst monitoring patients in the MR environment.
Case Report
Case 1
A 59-year old woman who presented to spinal surgeons with reduced sensation down her right leg. Her past medical history included ovarian cystectomy, hysterectomy, numerous lumbar and cervical spine fusions, discectomies and decompression for cauda equine syndrome. On this admission and as part of the diagnostic work-up, she had MRI of the brain and whole spine using the “Phillips Intera 1.5 Tesla Magnet” MR device. It is thought that the patient was of a nervous disposition and it was agreed that she would best tolerate the investigation under general anesthesia. The scan was undertaken with full anesthetic monitoring, consisting of: 3-lead ECG (coated carbon/ graphite fibers); blood pressure cuff and oxygen saturation probe. MRI compatible equipment was utilized for this purpose, including GE Healthcare MRI Monitor (DATEX- Ohmeda S/5). Total duration of the scan lasted approximately 90 minutes.
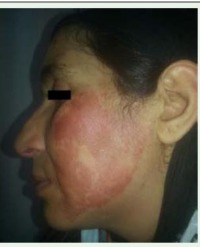
On emergence from the anesthetic, the patient started complaining of a burning sensation on her anterior chest and abdominal wall. On further examination, there was an erythematous, blistering line radiating from the xyphoid process to a few centimeters above the umbilicus, approximately 1cm in width (Figure 1).

Figure 1: An erythematous, blistering line radiating from the xyphoid process to a few centimeters above the umbilicus, approximately 1cm in width.
The line and pattern corresponded to a burn from a braided 3-lead ECG.
Cold swabs were immediately applied to the burnt area, analgesia, and 500 IUs booster dose of human immunoglobulins for tetanus were given. The patient was then transferred to our burns unit. She sustained 0.2% superficial partial thickness burn of her Total Body Surface Area (TBSA). She remained heamodynamically stable and apyrexial. Laboratory investigations revealed hemoglobin 12g/ dL, white cell count 13x109/L,neutrophils 8.3, platelets 849x109/L, sodium 137mmol/L, potassium 4.6mmol/L, Urea 9.7mmol/L and creatinine 135mmol/L. ECG and other investigations, including urine myoglobinuria, were all unremarkable. Urgent plain abdominal radiograph and abdominal ultrasound were ordered, both of which excluded intra-abdominal visceral injury that may have occurred from old metallic surgical clips. The patient was therefore treated conservatively with Urgotul® SSD dressing and gauze. She appeared to be clinically dehydrated and was subsequently prescribed 1litre of Hartmann’s solution over 4 hours, followed by 1litre over 8hours. The patient made an uneventful recovery and was discharged within 24 hours of admission, with one week follow up at the out-patient dressing clinic.
Case 2
A 44-year-old male patient who presented with chronic lower back pain was admitted for whole spine MRI. His past medical history included hypertension which was controlled with an oral anti-hypertensive medication otherwise rest of his physical exam and medical history were unremarkable. As the patient was suffering from claustrophobia and upon his request, the MR scanning was performed under general anesthesia. MR device and anesthetic monitoring equipment used were the same as described the previous case.
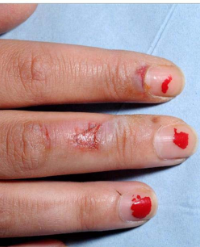
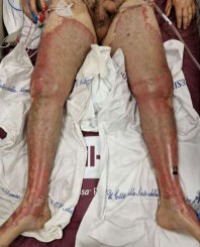
Total duration of MR scanning lasted 30 minutes. Upon wakening from anesthesia, the patient started to complaint of pain around umbilical region. Physical examination revealed a linear pattern of erythematous and blistered skin measuring approximately eight centimeters long on the anterior abdominal wall (Figure 2).

Figure 2: A linear pattern of erythematous and blistered skin measuring approximately eight centimeters long on the anterior abdominal wall.
Because of our experience with the previous case we suspected that his burns were induced by ECG cables. First aid measures included application of cold swabs and burn injury was treated conservatively with conventional burn dressings.
Discussion
MR scanners do not produce the adverse effects of ionizing radiation like CT and X-rays. MRI uses two components; a magnetic field and radio frequency to construct an image of the body.The magnetic field aligns hydrogen atoms in body water, and then radio frequency waves re-align the atoms to produce a rotating magnetic field, which produces signals to build images.The type of signal produced depends on the type of tissue from which the radio waves bounce-off [4,5].
Conduction of thermal energy through ECG cables or electrodes might seem to be the most straight forward mechanism of injury. However, heating during MRI can be evoked by several mechanisms [3]:
1. Electromagnetic induction heating: A change in the flux of the magnetic induction through a fixed circuit gives rise to an Electromotive Force (EMF).This consequently creates currents with changing amplitudes of magnetic field which results in joule heating of the conducting specimen.
2. Heating Due to the Antenna Effect: Transmission of an electric current along the length of the cables,with maximal density at the tip of lead (antenna effect).
3. Current induction: In an electrically conductive loop, intercepting a changing magnetic flux results in either a thermal or electrical burn.The former injury would result from heating of the skin and subsequent thermal radiation,whereas the latter is consequent when body tissues complete an electrical circuit with the wires because of capacitive coupling at the epidermis.
Energy from radiofrequency fields increases the oscillation of molecules and generation of heat. Human physiology compensates for this by inducing vasodilatation of skin capillaries which allows dissipation of heat. An imbalance between heat absorption and heat loss, or accumulation of heat underneath a contact object would lead to thermal injury. Electrical burns may not be painful immediately and may cause damage at temperatures as low as 43°C6. Our two patients had BMI (Body Mass Index) > 35 and spent a considerable time in the MR unit (90 minutes case 1 and 30 minutes in case 2).
Similar patient’s characteristics and duration of scanning were observed in the Dempsey review article, therefore suggesting that other factors may also increase the risk of thermal or electrical injuries while in the MR environment. Patients undergoing spinal or other orthopaedic investigations usually spend longer durations within the scanner, which predisposes them to greater heat stress and physiological insult. High BMI may also increase this risk, perhaps after difficult positioning of the patient or direct contact of patient body parts with the MR device. On further discussion with the operating radiographer, no conductive loops had been witnessed in the first case, however the pattern of injury described above evokes the belief that the ECG cable was in direct contact with patient skin.
The UK DoH reports that the commonest adverse incidents of MRI are current and contact burns [7]. In December 2007, the Medicines and Healthcare Products Regulatory Agency (MHRA), an executive agency of the UK DoH, issued “Safety Guidelines for Magnetic Resonance Imaging Equipment in Clinical Use” [8], as did the Association of Anesthetists in May 2002 [9]. We summarized a list of relevant recommendations below:
1. Appropriate positioning of patient and avoid direct contact of any body part with the scanner.
2.Ensure that no conductive loops forms with any parts of the patient’s body i.e. avoid skin-to skin contact.
3.The use of clothing or blankets as a form of insulation is not recommended, use foam pads, 1–2 cm thick, to insulate the patient from cables and MR device.
4.Use only MR compatible leads and monitoring devices.
5.A nominated consultant anaesthetist should be responsible for anesthesia services in MR units. Space and access to full anesthetic equipments should be available.
6.For unresponsive/ anaesthetized patients, routine checks should be performed to ensure no formation of conductive loops or occurrence of any other injury.
7.Patients should be monitored during anesthesia, sedation and recovery in compliance with minimum monitoring standards.
8.Ensure that the patient is instructed to inform staff immediately if they feel any pain or unusual sensation.
In case 1, the anaesthetist documented patient’s details and vital data on our hospitals surgical operative chart. This includes a front sheet with the current World Health Organisation (WHO) surgical checklist. On retrospective analysis of patient’s medical records, it was noted that the surgical checklist was not used. Although it is not common to use the WHO surgical checklist outside operative theatres settings, use of checklists as risk assessment tools, may help to decrease the rate of similar adverse effects in future. A Nottingham review of patient safety during plastic surgery procedures found significant reduction in clinical incidents following the implementation of the WHO surgical checklist. Such risk assessment tools provide structured frameworks that standardize and regulate the delivery of care across hospitals and specialized units and promote communication between different staff members’ ultimately aid reduction of patients’ morbidity and mortality [10].
The imlementation of a checklist for MRI under general anesthesia and/or other such procedures, using the guidelines above, will only be effective and reliable if all relevant staff members have been educated and trained to use those safety checklists. Checklists cannot merely be practiced as tick-boxing activities; staff should be made aware of the potential risks of MRI so they can objectively work towards their prevention.This should involve conveying the safety recommendations by DoH and the Association of Anesthetists, and promoting their accessibility to all levels of staff that have patient contact during MRI.
Conclusion
Burns are a common form of injury within public; however iatrogenic burns such as those induced by MR scanning are extremely rare and preventable.The latter may be attributed to variables that have been overlooked, as in these two cases at time of injury.These variables appear common amongst most reports of MRI-induced burn injuries, and include 1) length of stay within MR scanners and 2) patient’s BMI, which can contribute to poor positioning within the device. There is still uncertainty whether burn injuries were thermally or electrically-induced, and several mechanisms of injury have been suggested. Nevertheless, our report has shown the importance of educating staff in the prevention and immediate detection of the complications of MRI under general anesthetic. It also highlights the fundamental need for preparing national guidelines and safety checklists, which must be vigorously observed, implemented and maintained for MRI and other such procedures, by all relevant members of staff. This will maintain patient safety, improve clinical practice and prevent similar injuries within our hospital and other institutions across the country.
References
1. Hettiaratchy S, Dziewulski P. ABC of burns. BMJ. 2004; 328: 1366-1368.
2. Landman A, Goldfarb S. Magnetic Resonance-Induced Thermal Burn. Annals of Emergency Medicine. 2008; 52: 308-309.
3. Dempsey MF, Condon B. Thermal Injuries Associated with MRI. Clinical Radiology. 2001; 56: 457-465.
4. Grainger RC, Allison D, Adam, Dixon AK. Diagnostic Radiology: A Textbook of Medical Imaging. 4th edition. New York. 2001.
5. Novelline RA. Squire’s fundamentals of radiology. 5th edition. Harvard University Press; 1997.
6. Knopp MV, Essig M, Debus J, Zabel HJ, Van Kaick G. Unusual burns of the lower extremities caused y a closed conducting loop in a patient at MR imaging. Radiology.1996; 200: 572-575.
7. Department of Health. Safety Guidelines for Magnetic Resonance Imaging Equipment in Clinical Use. DoH. 2007.
8. http//.mhra.gov.uk. Last accessed 13/01/2011.
9. The Association of Anaesthetists of Great Britain and Ireland. The Provision of Anaesthetic Services in Magnetic Resonance Units. 2002.
10. Rehim S, Morritt A, Perks G. W.H.O Surgical Checklist and its Practical Application in Plastic Surgery. Plastic Surgery International. 2011; 1-5.