Case Report | Volume 2 - Issue 1 | Article DOI :
Download PDF
Qianqian Wang1, Wenjuan Wang2, Wanfeng Fan1, Qian zhou1, Liguang Yang1 and Xinjiang Liu1*
1Department of Radiology, Binzhou Medical University Hospital, China
2Binzhou Medical University, China
Corresponding Author:
Xinjiang Liu, Department of Radiology, Binzhou Medical University Hospital, Binzhou 256603, China, Tel: 13356286368
Keywords
Diffuse Large B-Cell Lymphoma (DLBCL); Primary Female Genital System Lymphoma (PFGSL); Extranodal lymphoma; Diagnosis
Abstract
A 64-year-old woman who was found to have an abdominal mass on ultrasound was misdiagnosed with a uterine fibroid/uterine sarcoma. Pelvic MRI showed multiple soft tissues mass shadows in the pelvic cavity, and the larger shadows were approximately 14.2 cm × 9.7 cm × 15.6 cm, with clear boundaries dominated by an iso long T1 and slightly longer T2, locally visible nodular long T2 and short T2 signal foci, and obvious high signals on DWI and decreased ADC signals. The enhancement of the densification was obviously non-uniform. The immunohistochemical results were positive for CD20, LCA, PAX-5+, CD43 +, c-myc, bcl2 and bcl6 and negative for SAM, Desmin, Myo D1, MPO, CD99, CD30, CD23, S-100, and CD10. The majority (90%) of tumor cells were positive for Ki-67. The diagnosis was a diffuse large b-cell lymphoma. Preoperative diagnosis of primary lymphoma of the uterus is difficult in clinical situations. Primary Female Genital System Lymphoma (PFGSL) is a rare disease that is mostly associated with non-Hodgkin’s lymphoma, usually Diffuse Large B-Cell Lymphoma (DLBCL). The majority of primary uterine DLBCL originates from endometrial stroma
Citation
Wang Q, Wang W, Fan W, Zhou Q, Yang L and Liu X. Primary Diffuse Large B cell Lymphoma of the Uterus: A Case Report and Literature Review. J Radiat Oncol Res. 2018; 2(1): 1007.
Introduction
The global incidence of Non-Hodgkin’s Lymphoma (NHL) is 3%, of which 1% comes from extranodal lymphoma [1]. Diffuse Large B-Cell Lymphoma (DLBCL) is the most common histologic subtype in extranodal lymphoma, accounting for approximately 50% of cases [2]. Primary Female Genital System Lymphoma (PFGSL) of the reproductive system is a rare disease, accounting for only 0.21-1.1% of extranodal lymphoma [2,3]. Frequently occurring parts include the ovary, uterus, vagina and vulva. This paper reports a case of primary lymphoma of the uterus that was misdiagnosed as uterine fibroids.
Case Report
Clinical evidence
The female patient, who was 64 years old, was found to have uterine fibroids by a physical examination 23 years ago. Natural menopause occurred 11 years ago, with no abnormal vaginal bleeding after menopause. Over the past 2 months, the tumor in the lower abdomen was spontaneously palpable and hard, and a color ultrasound examination performed 4 days ago suggested a hypoecho in the pelvic cavity, possibly fibroids with diameters of approximately 10 cm. The patient had no nausea and vomiting, occasional abdominal distension, no diarrhea, no abdominal pain, discomfort in the lumbosacral region, anorectal heaving and distension in January, as well as no frequent urination, urgent urination or pain; no insensitivity to urination; and no abnormal leucorrhea.
Gynecological examination
Vulva development is normal; married and delivered; vagina unobstructed, smooth wall; cervical atrophy, incomplete exposure due to tumor compression, smooth palpation surface, no lift pain and sway pain; palpation of the uterus is not clear; the pelvic cavity touches a hard surface; irregular, movement is acceptable; the upper edge reaches the level of the umbilicus, no obvious tenderness; mild tenderness in the left adnexal region. No obvious abnormalities were found in the right accessory area.
Intraoperative observations
The uterus increases with size, such as during pregnancy, and congestion, with a brittle, anterior wall only exposed at the bottom of the palace; most of the anterior wall had edema thickening and hardening of the urinary bladder as well as invasion adhesion coverage; double accessories were not observed, but there was an obvious abnormal appearance; the rectum anterior wall had bumps that were approximately 5cm in diameter; the oppressed rectum was larger than the other small intestine segments and was mesenteric was the greater omentum 0.88cm in size with multiple lesions; most of the lines indicate a uterus excision and double appendix resection.
Imaging findings
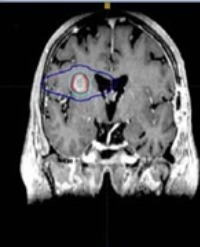
There were multiple large soft tissue shadows in the pelvic cavity, and the larger ones were approximately 14.2cm × 9.7cm × 15.6cm in size; the boundary was still clear. The lesions were characterized by an equal length T1 and slightly longer T2, with locally visible nodular long T2 and short T2 signal foci. The DWI signal was obviously high and the ADC signal was reduced. The part of the enhancement showed obvious non-uniform reinforcement. The uterus was imbedded, the normal musculoskeletal structure was unclear, and the posterior part of the lesion was closely related to the rectum, as shown in Figure 1.

Figure 1: A 64-year-old woman, Primary female genital system lymphoma. Pelvic MRI showed multiple soft tissue mass shadows in the pelvic, T2 coronal position, T2-fs sagittal position, T2-fs axis position, Obviously high signal on DWI, Low Signal on ADC. The part of the enhancement showed obvious non-uniform reinforcement.
Pathology findings
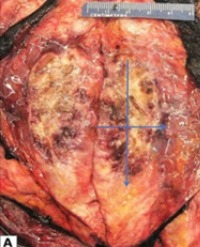
The uterine volume was approximately 6×6×5.5 cm, and the endometrium was smooth with a mass under the endometrium, with a volume of 14×13×10.5 cm. There were numerous white nodules in the left mesosalpinx, with a diameter of 0.1-1.3 cm, and the volume of the left ovary was 1.7×0.8×0.6 cm. There was one gray-white nodule in the mesosalpinx and the right ovary area each, a volumes of 2.7×1.7×0.8 cm and 3.5×3.5×2.5cm, respectively. The cut surface was all soft and gray-red, and there was 1 white fish-like nodule (mesenteric metastasis), with a volume of 3×2.5×1.2 cm, as shown in Figure 2.

Figure 2: Diffuse large b-cell lymphoma, the Pathological gross specimen. The microscopic 10 x10.
We concluded that the masses represented diffuse large b-cell lymphoma.
Immunohistochemical
CD20+, PAX-5+, CD3 -, CD5 -, CD43+, CD10-, the Bcl- 6part+, scattered in weak MUM - 1+, the Bcl - 2+, cyclin D1 scattered +, CD23 -, CD30 -, c - myc part weak +, LCA +, CK-, Vimentin part +, SMA -, Desmin-, MPO -, Myo D1-, Myogenin -, CD99 -, S-100 -, ki - 67 approximately 90% (Table 1).
Table 1: Description of the immunohistochemistry and its significance.
| Marker |
Description |
Status in our |
Significance |
| patient |
| CD20 |
Pan-B-cell antigen |
+ |
Indicates B-cell origin |
| CD43 |
Pan-T-cell antigen |
+ |
Indicates T-cell origin |
| CD30 |
Tumor necrosis factor receptor; |
- |
Used in diagnosis of Hodgkin's lymphoma |
| lymphocyte activation antigen |
| CD3 |
pan-T-cell antigen |
- |
Indicates T cell origin of lymphocytes |
| BCL6 |
Germinal center marker |
+ |
positive in T-cell, DLBCL, Burkitt’s, Follicular, and Hodgkin's lymphomas |
| BCL2 |
Proto-oncogene; prevents cells from |
+ |
positive in Follicular, Burkitt’s, DLBCL, Hodgkin's, Mantle Cell, and |
| Marginal Zone lymphomas |
| Multiple Myeloma 1 |
Intra- and post-germinal center B-cell |
+ |
Helps distinguish between germinal center and non-germinal center DLBCL |
| (MUM1) |
marker |
| Ki-67 |
Labile, non-histone nuclear protein. Marker |
0.9 |
Higher nuclear staining indicates more aggressive tumor |
| of cell proliferation |
| CD10 |
Cell membrane metallopeptidase; germinal |
- |
positive in germinal center DLBCL, Burkitt’s, Follicular, Hairy cell |
| center marker |
lymphomas. Occasionally expressed in uterine smooth muscle tumors |
| Smooth muscle actin |
Expressed by smooth muscle cells |
- |
Indicates smooth muscle origin |
| (SMA) |
| Desmin |
Expressed by smooth muscle cells |
- |
Indicates smooth muscle origin |
| S100 |
Cytoplasmic EF-hand Ca2+-binding |
- |
Marker of neural tissue and melanocytic differentiation |
| protein |
Discussion
PFGSL is a rare disease that is mostly associated with non-Hodgkin’s lymphoma, usually diffuse large b-cell lymphoma [4]. Nasioudis et al. [3] found that 667 cases in the SEER database were primary tumors in female genital lymphoma from 1988 to 2012. The most common histological subtypes were diffuse large B cells (59.8%) and follicular lymphoma (11.9%), which occurred in the ovary (37%), cervix (21.4%) and uterus (16.5%). Of these, 62.8% underwent surgery. The majority of primary uterine DLBCL originated from endometrial stroma. The discovery of DLBCL in uterine fibroids has been reported only twice before. Zhao [5] reported a 73-year-old female with an endometrial mass of 17 cm, which was diagnosed as a primary DLBCL. The DLBCL originated from uterine fibroids, and the tumor extended to the adjacent myometrium, including intravascular tumor thrombosis. Alexandra Martin [2] reported a case with a uterine mass of 10×8×5.8 cm, with white-brown orbicular nodules. The biopsy showed benign hysteromyoma accompanied by mucinous changes, and hysteromyoma showed abnormal nodules infiltrated by local lymphocytes. The tumor was composed of large atypical lymphocytes with an obvious enhancement of mitosis and active apoptosis in large nuclei and diverse nucleoli. Ana Regalo [6] reported a large b-cell lymphoma of the cervix. Pelvic MRI showed an uneven mass of the cervix, the size of which was 7.9×7.6×6.9 cm; interstitial destruction; and obvious involvement of the bladder. Patro [7] reported a case of uterine primary diffuse large b-cell lymphoma with a specimen size of 13.5 ×10× 8 cm. The myometrium was diffusely thickened, with a fish-like appearance. On immuno-histochemical evaluation, tumor cells were found to be immuno-positive for CD 20, and LCA and were immuno-negative for CD 3, CD 5, MPO, CD 23 and CD 10. p53 showed a positive response, and 80% of tumor cells were positive for Ki-67.
A preoperative diagnosis of primary lymphoma of the uterus is difficult in clinical situations. Patients with a primary lymphoma of the uterus often have no symptoms or non-specific abdominal symptoms, including abdominal pelvic pain, abdominal distension, vaginal bleeding or bleeding in their urine, or gastrointestinal symptoms [8,9]; only 17% of non-Hodgkin’s lymphoma patients reported physical symptoms, such as fever, night sweats or weight loss. Zhu Yilu [10] believed that the significant high signal of diffusion weighted imaging (DWI)was characteristic of uterine lymphoma on MRI, but the final diagnosis still required pathology. Fox and Vang [11] et al. developed the following diagnostic criteria [2,7,9]: 1) the reproductive system is the only affected organ; 2) no bone marrow or peripheral blood abnormalities; 3) no history of lymphoma; and 4) the presence of lymphoma at a distant site should be separated from the primary lymphoma for several months.
Genital lymphoma is rare, without standard treatment guidelines, and is often treated with surgery and chemotherapy combined with radiotherapy according to the patient’s situation. Diffuse large b-cell lymphoma chemotherapy usually adopts the r-chop regimen, namely, rituximab combined with cyclophosphamide, doxorubicin and prednisone [12,13]. Tarec [14] believes that DLBCL involvement in the uterus is associated with a high risk of secondary central nervous system involvement, and these patients should be considered for central nervous system staging and prevention.
References
1. Cubo AM, Soto ZM, Cruz MA. Doyague MJ, Sancho V, Fraino A, et al. Primary diffuse large B cell lymphoma of the uterine cervix successfully treated by combined chemotherapy alone: A case report. Medicine (Baltimore). 2017; 96: 6846.
2. Martin A, Medlin E. Primary, non-germinal center, double-expressor diffuse large B cell lymphoma confined to a uterine leiomyoma: A case report. Gynecol Oncol Rep. 2017; 22: 78-81.
3. Nasioudis D, Kampaktsis PN, Frey M. Witkin SS, Holcomb K. Primary lymphoma of the female genital tract: An analysis of 697 cases. Gynecol Oncol. 2017;145: 305-309.
4. Samama M, van Poelgeest M. Primary malignant lymphoma of the uterus: a case report and review of the literature. Case Rep Oncol. 2011; 4: 560-563.
5. Zhao L, Ma Q, Wang Q, Ying Zeng, Qingya Luo, Hualiang Xiao. Primary diffuse large B cell lymphoma arising from a leiomyoma of the uterine corpus. Diagn Pathol. 2016; 11: 9.
6. Regalo A, Caseiro L, Pereira E, José Cortes. Primary lymphoma of the uterine cervix: a rare constellation of symptoms. BMJ Case Rep. 2016; 2016.
7. Patro MK, Bal AK, Santosh T, Mishra B. Primary Non-Hodgkin’s Lymphoma of Diffuse Large B-Cell Phenotype [DLBCL] of Uterine Corpus: A Rare Case Report with Brief Review of the Literature. J Obstet Gynaecol India. 2016; 66: 675-678.
8. Chen R, Yu Z, Zhang H, Ding J, Chen B. Primary malignant lymphoma of the uterus and broad ligament: a case report and review of literature. Onco Targets Ther. 2015; 8: 265-268.
9. Nasioudis D, Frey MK, Chapman-Davis E, Caputo TA, Holcomb K. Fertility preserving surgery for advanced stage ovarian germ cell tumors. Gynecol Oncol. 2017; 147: 493-496.
10. Zhu YL, Qian HF, Shen J. MRI diagnosis of primary lymphoma of uterus. Modern practical medicine. 2012; 1052: 1038-1039.
11. Vang R, Medeiros LJ, Deavers MT. Current problems with staging lymphomas involving the ovary. Am J Surg Pathol. 2006; 30: 1202-1203.
12. Shen H, Wei Z, Zhou D, Zhang Y, Han X, Wang W, et al. Primary extra-nodal diffuse large B-cell lymphoma: A prognostic analysis of 141 patients. Oncol Lett. 2018; 16: 1602-1614.
13. Upanal N, Enjeti A. Primary lymphoma of the uterus and cervix: two case reports and review of the literature. Aust N Z J Obstet Gynaecol. 2011; 51: 559-562.
14. El-Galaly TC, Cheah CY, Hutchings M, Mikhaeel NG, Savage KJ, Sehn LH, et al. Uterine, but not ovarian, female reproductive organ involvement at presentation by diffuse large B-cell lymphoma is associated with poor outcomes and a high frequency of secondary CNS involvement. Br J Haematol. 2016; 175: 876-883.