Case Report | Volume 4 - Issue 1 | Article DOI :
Download PDF
Samantha Webking1*, Mary Morse1, Nevill Duncan4, Daniel Hildebrandt1, Sherif Nasr3, Stephanie Bernik2, Mohamed Aziz3
1American University of the Caribbean, USA
2Mount Sinai Medical Center, New York, NY, USA
3siParadigm Diagnostic Informatics, NJ, USA
4NOVA Southeastern University, FL, USA
Corresponding Author:
Samantha Webking*, American University of the Caribbean, USA, Tel: 850-200-3912
Keywords
Radiation-associated angiosarcomas (RAA); Angiosarcomas (AS); Immunohistochemistry (IHC)
Abstract
Though rare, angiosarcomas are one of the most common tumors to arise following radiation therapy for the treatment of malignancies, such as breast cancer and Hodgkin’s lymphoma. Investigation of radiation-associated angiosarcomas has always proven difficult due to the extremely low incidence. This means that case studies are the predominant type of investigation found in the literature. Breast cancer treatment can lead to chronic lymphedema due to the dissection of axillary lymph nodes, as well as radiation treatment, often following conservative breast surgery. Due to these risk factors, breast cancer patients are at an increased risk of development of angiosarcoma. We present a case of breast angiosarcoma that developed after radiation therapy for breast ductal carcinoma. In this case, there were multiple metastases and recurrences in the involved breast, as well as development of angiosarcoma in the opposite breast. We also provide a brief review of the literature.
Citation
Webking S, Morse M, Duncan N, Hildebrandt D, Nasr S, Bernik S, Aziz M (2022) Recurrent Radiation-Associated Breast Angiosarcoma. Report of a Case with Uncommon Clinical Presentation and Brief Review of the Literature. J Radiat Oncol Res 4: 5.
ABBREVIATION
Radiation-associated angiosarcomas (RAA); Angiosarcomas (AS); Immunohistochemistry (IHC)
INTRODUCTION
Sarcomas are rare malignancies that comprise only 1% of adult cancers. These tumors arise from the mesenchyme, with 80% of sarcomas originating from soft tissues, and the remaining 20% arising from the bone. Angiosarcomas (AS) comprise only 2% of soft tissue sarcoma cases but are highly aggressive, with up to 44% of patients having advanced metastasis disease at the time of diagnosis [8, 10]. There are over 100 subtypes of sarcomas, and they are named via the cells from which they originate. Angiosarcomas arise from the endothelial cells lining the vasculature and lymphatics. Like other sarcomas, angiosarcomas can arise as primary or secondary tumors but often are unable to be linked to a specific cause. Some genetic conditions have been linked to the development of primary diseases, such as Li-Fraumeni and Neurofibromatosis Type I. Secondary angiosarcomas are linked to risk factors such as previous radiation treatment, environmental exposure to carcinogens, and lymphedema [10].
In a 10-year review from 1997 to 2007, breast cancer patients from the University of Kansas Medical Center and Ohio State University Medical Center had a 0.1-0.2% incidence of angiosarcoma. Out of the 11 total cases identified, eight cases were diagnosed as post-radiation malignancies.13 Though rare; the prognosis for these tumors is often poor. The prognosis of the disease is most consistently linked to the age of the patient, the grade of the tumor, and whether metastases are present at the time of diagnosis. Primary tumors are more common in younger populations with the average age ranging from 50 – 54 years of age. These patients have a better prognosis compared to patients with secondary tumors, with an overall survival rate of approximately 93 months. Comparatively, secondary tumors are found more commonly in older populations, with a median age of 70 to 74 years, and carry a median overall survival of 32 months [14]. Over half of all angiosarcomas present as cutaneous lesions. These malignancies are often mistaken for hematomas or other soft tissue masses [3]. CT scans and MRIs may be helpful in the identification of these tumors, but histological examination is required to definitively diagnose the disease. Due to the endothelial origin, these tumors often stain with vascular markers like CD31, Factor VIII, and VEGF [1].
We report on this rare serious malignancy to highlight the presentation and severity of the disease. Early identification and treatment are essential to increase survival from this aggressive malignancy, but due to its rarity, it can be misdiagnosed. Patients who receive conservative breast surgeries followed by radiation are at an increased of developing secondary angiosarcoma.
CASE PRESENTATION
A 61-year-old woman presented with two upper abdominal nodular skin lesions, one on the right and one on the left. The right lesion measured 1 cm and the left lesion measured 0.8 cm. The patient had a history of a total hysterectomy at the age of 51 due to extensive leiomyomas. She also had a history of localized right breast ductal carcinoma five years before her current presentation, which was treated by lumpectomy, postoperative radiation therapy, and hormonal treatment. She had no other significant medical history. Her family history included her father died of advanced colon cancer at the age of 72.
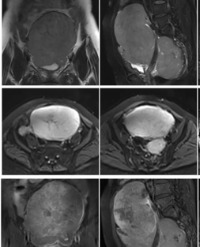
The two abdominal skin lesions were surgically excised with adequate safe surgical margins. The histomorphologic features and immunohistochemistry (IHC) studies were consistent with a diagnosis of cutaneous angiosarcoma, intermediate grade. At that time, there was no evidence of other similar lesions elsewhere. Three months later, the patient noticed a right breast lump gradually increasing in size, but she did not seek immediate medical attention. With a marked increase in size, the patient reported to our facility for examination. Breast examination revealed a large breast mass including and surrounding the site of the prior breast carcinoma excision. The overlying skin showed thickening and blue dark pink discoloration. After non-specific findings on a mammogram, MRI was performed and showed Heterogeneous signals on both T1-weighted and T2-weighted images outlining approximately 11x9 cm mass. Tissue evaluation was recommended. A core biopsy was performed. Microscopic examination revealed irregular anastomosing vessels containing endothelial cells with moderate nuclear pleomorphism, enlargement, and atypia. Atypical mitotic figures were also identified (Figure 1 A-B).

Figure 1: Microscopic examination of right breast mass.
1A: Low power view showing irregular anastomosing vessels containing atypical endothelial cells (H&E stain x20) 1B: High power view showing Pleomorphic endothelial cell with scattered atypical mitosis (H&E stain x60) 1C: Angiosarcoma tumor cells positive for CD31, 1D: Angiosarcoma tumor cells positive for Factor VIII
Histomorphology was similar to that seen in prior skin biopsies; however, more solid areas were seen. IHC studies were performed and the tumor cells were positive for Vimentin, CD34, CD31 (Figure 1C), Factor VIII (Figure 1D), and Fli-1, while negative for Cytokeratin AE1/AE3, S100, Desmin, and EMA. The morphologic features in addition to the IHC profile were consistent with the diagnosis of radiation-associated breast angiosarcoma. Prior right breast carcinoma was reviewed and showed no evidence of sarcoma.
Due to the large size of the mass, a multidisciplinary tumor board meeting recommended neoadjuvant chemotherapy followed by mastectomy and right breast reconstruction. The patient was treated with combination of doxorubicin, and ifosfamide. She subsequently underwent a mastectomy. The mastectomy specimen showed a large central cystic hemorrhage mass associated with dense fibrous areas measuring at least 8x6 cm extending into the adjacent breast tissue surrounded by post-chemotherapy treatment effect with reactive reparative changes involving 85% of the mass (Figure 2A).

Figure 2: Mastectomy, right breast
2A: Hemorrhagic tumor mass associated with moderate post-treatment reactive reparative changes, 2B: Low power view showing scattered foci of residual angiosarcoma (upper part) in the background of dense fibrocollagenous reaction representing treatment effect lower part)(H&E stain x20), 2C: Intermediate power view showing foci of DCIS (right side) and atypical ductal hyperplasia (left side) (H&E stain x40), 2D: Ductal carcinoma in situ (DCIS) with moderate to high nuclear grade (H&E stain x60).
Foci of residual angiosarcoma scattered within the necrotic cavity were identified (Figure 2B) The breast also showed scattered foci of intermediate to high-grade grade ductal carcinoma in situ (DCIS) and atypical ductal hyperplasia (Figure 2C-D). There was no evidence of axillary lymph node involvement. No post-operative treatment was provided. Five months later, a news dark blue purple lesion appeared on the skin of the reconstructed right breast and microscopic examination confirmed the diagnosis of recurrent angiosarcoma. A wide re-excision was performed with corrective breast reconstruction.
Eight months later, a new nodular skin lesion mass measuring 1.7 cm appeared on the left breast. The lesion was similar to those seen previously in the right breast. Excision and microscopic examination confirmed the diagnosis of angiosarcoma of the left breast with stromal infiltration. Three months later, the patient underwent a left mastectomy, which showed no residual angiosarcoma and no other type of malignancies. No post-operative treatment was provided and the patient elected not to have left breast reconstruction. The patient expired 5 months later due to extensive metastases to the lung, liver, and bone.
DISCUSSION
Angiosarcomas are aggressive rare malignancies that arise from endothelial cells of the vasculature or lymph vessels. Accounting for only 2% of soft tissue sarcomas, angiosarcomas are most common in elderly patients. They can be found anywhere on the body, and due to the high rate of metastasis in patients, the diagnosis must be made early. Nearly 60% of all angiosarcomas present as cutaneous lesions [1].
The patient reported here was originally treated for her ductal carcinoma with a lumpectomy followed by postoperative breast radiation. Though radiation is essential in the treatment of breast cancer, it is also a risk factor for the development of angiosarcoma in areas of radiation exposure [3]. Radiation therapy is associated with decreased breast cancer mortality rates among patients of younger age, higher nuclear grade, and larger-sized tumors [9]. The risk of development of angiosarcoma following breast conservative surgery is 0.04 to 0.15% [3]. Due to increased diagnosis of breast cancer, as well as improved treatment outcomes, breast cancer patients have increased survival rates. The increase in the number of patients treated with breast conservation across the last few decades has led to the increased incidence of secondary angiosarcoma in patients with prior radiation treatment [3].
Primary angiosarcoma tends to arise in younger patients and is often without known risk factors. Secondary angiosarcomas tend to develop in older populations and are commonly associated with radiation therapy and areas of chronic lymphedema [5]. Other risk factors for the development of angiosarcoma include environmental toxins and inheritable diseases. Genetic factors are attributed to 3% of primary angiosarcomas. Environmental carcinogens such as vinyl chloride and chronic arsenic exposure are the leading known cause of hepatic angiosarcomas. There seems to be little distinction between men and women in the development of this malignancy, but cutaneous lesions are more common among male patients. The median age for development is 60 – 71 years of age [1]. Angiosarcomas often are difficult to discern from other types of cutaneous cancers, such as anaplastic melanoma or epithelial carcinomas. Due to the vagueness of symptoms, as well as the wide range of similar appearing neoplasms, benign or malignant, histological examination of the tumor is required for a definitive diagnosis [1]. The diagnosis of radiation-induced sarcoma requires four determinants. These four determinants were introduced by Cahan et al and consist of (1) development of the sarcoma in the irradiated field, (2) a latency period of at least 4 years, (3) histologic proof of sarcoma, (4) no evidence of sarcoma in the primary tumor [8].
The presentation of angiosarcomas can widely vary. Symptoms may include nausea, vomiting, changes in bowel habits, or abdominal pain. Cutaneous angiosarcomas, which are the most common, often present as blue or red nodules. They are often mistaken for hematomas, further leading to the delay of diagnosis. Radiologic examination of the tumor can also aid in the diagnosis of breast angiosarcoma. Findings are usually non-specific on mammography. On ultrasound, the masses could present with hyperechoic or a mixed echogenicity pattern based on their vascular channels or cellular components. Benign lesions typically have a hyperechoic pattern, and this is one of the reasons why breast angiosarcoma can be misdiagnosed as benign. These lesions may ulcerate and bleed, which can help in identification.18, 20 MRI can be used to delineate a clot from a tumor. Both CT and MRI may be useful in the delineation of angiosarcomas from other tumors and the identification of metastasis. Numerous studies have reported the potency of MRI in determining the malignancy of angiosarcoma. Angiosarcoma exhibits high signal intensity on T2-weighted. images; significant enhancement is observed in the early stages; and the enhancement curve is in a washout pattern. Large masses have high signal intensity on both the T1-weighted and T2-weighted images, causing thrombocytopenia and secondary bleeding [15,16]. Imaging manifestations of breast lymphoma are nonspecific and the age of onset for this disease is similar to that for breast angiosarcoma. Patients with breast lymphoma have a higher incidence of presentation with swollen axillary lymph nodes, which can help the differentiation between the two breast diseases. A breast angiosarcoma presenting as a solitary mass should be also differentiated from phyllodes tumor [15].
Immunohistochemistry is still required to provide a definitive diagnosis. Due to their origin from endothelial cells, endothelial markers such as Factor-VIII, CD31, CD34, and VEGF can be used for immunohistochemistry antigen targets. CD31 can be found in over 50% of angiosarcomas [10]. Radiation-induced angiosarcoma often appears as irregular anastomosing vessels containing endothelial cells with nuclear atypia [4]. Molecular studies on post-radiation breast angiosarcoma are limited. George D. Wilson et al. performed next-generation sequencing using a targeted panel of 160 cancer-related genes. Genomic variants were identified for mutation and trinucleotide-based mutational signature analysis. The study identified individual genomic variants including variants in EGFR and BRAF that occurred in all samples of cases. In addition, genes associated with the role of BRCA1 in DNA damage response were commonly altered in all of the cases of radiation-induced angiosarcoma [17].
Surgical removal of the tumor remains the focus of treatment, with radiotherapy and chemotherapy also being utilized. Angiosarcomas spread rapidly and diagnosis is often delayed due to their rarity and vague presentations. Postoperative radiotherapy has been used to decrease the rates of reoccurrence. Radiotherapy is also utilized in patients with inoperable tumors. Half of the patients with angiosarcomas will develop local recurrence and distant metastases. Cytotoxic chemotherapy is the preferred treatment method for metastatic disease [1].
The prognosis for angiosarcoma is often poor due to its aggressive nature. At the time of diagnosis, up to 44% of patients experience metastases which are most commonly identified in the brain, and lung. Like other sarcomas, angiosarcomas most commonly spread hematogenously [10]. Studies showed that for primary tumors, the average age is 50 – 54 years, and the overall survival is 93 months on average. Comparably, secondary angiosarcoma tumors arose in older populations, with an average age of 70 to 74 months, and were associated with an average overall survival of 32 months.14 Other studies reported the overall 5-years survival was identified as 30-40%.1 The prognosis for recurrence for angiosarcoma patients was most importantly linked to the size of the tumor, histologic grade, and the stage at the time of diagnosis [8,10]. A review generated from Massachusetts General Hospital (MGH) found that 83% of patients with tumors larger than 20cm were found to have distant metastases. This differs from tumors 2.5cm or less in size, which had a metastasis rate at the time of diagnosis of only 6% [12].
Breast angiosarcomas are often misdiagnosed because they are not seen often and can have deceptively benign characteristics on mammograms and histological analyses.
Preoperative diagnosis by biopsy can be extremely difficult and has a false negative rate of approximately 37%. These numbers can be justified since higher grade angiosarcomas may contain elements of lower grade tumors, especially at the periphery, and remain well differentiated [18,19]. Umesh Jayarajah and group reported a case of bilateral RAA of the breast, but in their case, angiosarcoma developed following bilateral breast carcinoma treated with lumpectomy and post-operative radiation therapy1. In our case, the angiosarcoma of the opposite breast developed without prior carcinoma or radiation treatment. Askin Dogan et al. reported an additional case of RAA; and in their review, they summarized in a large table all prior reported 307 cases spanning the time from 1985 to 2017 [11].
We report this case and hope to add to the data, signifying the risk of angiosarcoma development in this group of patients. With over half of all lesions presenting cutaneous, we are allowed to better bring to the forefront the importance of vigilant observation of our patients with risk factors in their histories, including prior radiation exposure. The case presented also outlines the possibility of angiosarcoma development in the opposite breast with no prior radiation treatment. It also highlights the importance of considering radiation-induced angiosarcoma of the breast as a differential diagnosis in a patient with recurrent breast neoplasms.
ACKNOWLEDGMENT
Special thanks to Angela Burkett and Angela Castillo Franco for their assistance in preparing manuscript images and reviewing the final manuscript.
CONFLICT OF INTEREST
Authors reported no conflicts.
REFERENCES
1. Cao J, Wang J, He C, Fang M. Angiosarcoma: a review of diagnosis and current treatment. Am J Cancer Res. 2019 Nov 1;9(11):2303-2313. PMID: 31815036; PMCID: PMC6895451.
2. Giannakeas V, Sopik V, Narod SA. Association of Radiotherapy With Survival in Women Treated for Ductal Carcinoma In Situ With Lumpectomy or Mastectomy. JAMA Netw Open. 2018;1(4):e181100.
3. Verdin, V., Mattart, L., Cusumano, P. G., De Hertogh, O., De Meester, C., Francart, D., Kirova, Y. M., Nelissen, X., Sacino, F., Vanderick, J., Weerts, J., & Markiewicz, S. (2021). Angiosarcoma associated with radiation therapy after treatment of breast cancer. retrospective study on Ten Years. Cancer/Radiothérapie, 25(2), 114–118. https:// doi.org/10.1016/j.canrad.2020.05.020
4. Bonito, F. J., Almeida Cerejeira, D., Dahlstedt-Ferreira, C., Oliveira Coelho, H., & Rosas, R. (2020). Radiation-induced angiosarcoma of the breast: A Review. The Breast Journal, 26(3), 458–463.
5. Co, M., Lee, A., & Kwong, A. (2019). Cutaneous angiosarcoma secondary to lymphoedema or radiation therapy — a systematic review. Clinical Oncology, 31(4), 225–231. https://doi.org/10.1016/j. clon.2019.01.009
6. Jayarajah, U., Nagodavithane, K., Basnayake, O., & Seneviratne, S. (2020). Unusual presentation of bilateral radiation-induced angiosarcoma of the breast. Case Reports in Oncological Medicine, 2020, 1–4.
7. Grishma R. Sheth, Lee D. Cranmer, Benjamin D. Smith, Lauren Grasso LeBeau, Julie E. Lang, Radiation-Induced Sarcoma of the Breast: A Systematic Review, The Oncologist, Volume 17, Issue 3, March 2012, Pages 405–418,
8. Amajoud Z, Vertongen AS, Weytens R, Hauspy J. Radiation induced angiosarcoma of the breast: case series and review of the literature. Facts Views Vis Obgyn. 2018 Dec;10(4):215-220. PMID: 31367294; PMCID: PMC6658205.
9. Sagara, Y., Freedman, R. A., Vaz-Luis, I., Mallory, M. A., Wong, S. M., Aydogan, F., DeSantis, S., Barry, W. T., & Golshan, M. (2016). Patient Prognostic Score and Associations With Survival Improvement Offered by Radiotherapy After Breast-Conserving Surgery for Ductal Carcinoma In Situ: A Population-Based Longitudinal Cohort Study. Journal of clinical oncology : official journal of the American Society of Clinical Oncology, 34(11), 1190–1196.
10. Ryan, C. W., & Meyer, J. (2022, May 11). Clinical presentation, histopathology, diagnostic evaluation, and staging of soft tissue sarcoma. UpToDate. Retrieved July 10, 2022, from https://www. uptodate.com/contents/clinical-presentation-histopathology diagnostic-evaluation-and-staging-of-soft-tissue-sarcoma?search= angiosarcoma&source=search_result&selectedTitle=1~70&usage_ type=default&display_rank=1 11.
11. Dogan, A., Kern, P., Schultheis, B., Häusler, G., Rezniczek, G. A., & Tempfer, C. B. (2018). Radiogenic angiosarcoma of the Breast: Case Report and systematic review of the literature. BMC Cancer, 18(1).
12. Suit HD, Mankin HJ, Wood WC, Gebhardt MC, Harmon DC, Rosenberg A, Tepper JE, Rosenthal D. Treatment of the patient with stage M0 soft tissue sarcoma. J Clin Oncol. 1988 May;6(5):854-62. doi: 10.1200/ JCO.1988.6.5.854. PMID: 3367188.
13. Wang, X. Y., Jakowski, J., Tawfik, O. W., Thomas, P. A., & Fan, F. (2009). Angiosarcoma of the breast: A clinicopathologic analysis of cases from the last 10 years. Annals of Diagnostic Pathology, 13(3), 147–150.
14. Yin, M., Wang, W., Drabick, J.J. et al. Prognosis and treatment of non-metastatic primary and secondary breast angiosarcoma: a comparative study. BMC Cancer 17, 295 (2017).
15. Wu et al. angiosarcoma Mammography and MRI manifestations of breast BMC Women’s Health (2019) 19:73.
16. Sanders LM, Groves AC, Schaefer S. Cutaneous angiosarcoma of the breast on MRI. AJR Am J Roentgenol. 2006;187:W143–6
17. Thibodeau et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License 3.0 (CC BY 3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
18. Weller O, Lubert J, Shirah J, Fernandes K, Aziz M, et al. (2022) Primary Angiosarcoma of the Breast: Case Report of Uncommon Tumor and Brief Review of the Literature. JSM Breast Cancer Res 3: 4.
19. Bhosale, S., Kshirsagar, A., Patil, M., Wader, J., Nangare, N., & Patil, P. (2013). Primary angiosarcoma of breast: A case report. International Journal Of Surgery Case Reports, 4(4), 362-364.
20. Taghipour Zahir, S., Sefidrokh Sharahjin, N., & Rahmani, K. (2014). Primary breast angiosarcoma: pathological and radiological diagnosis. The Malaysian journal of medical sciences : MJMS, 21(5), 66–70.